Fentanyl-induced rigid chest syndrome after low-dose fentanyl: A case report
Ventilator waveforms as a clue to fentanyl–induced rigid chest syndrome
DOI:
https://doi.org/10.54205/ccc.v34.280804Keywords:
Fentanyl, Fentanyl-induced rigid chest syndrome, Naloxone, Wooden chest syndromeAbstract
Background: Fentanyl-induced rigid chest syndrome (FIRCS) is a rare, life-threatening adverse effect of fentanyl that can cause respiratory compromise and patient-ventilator dyssynchrony and currently lacks definitive diagnostic criteria.
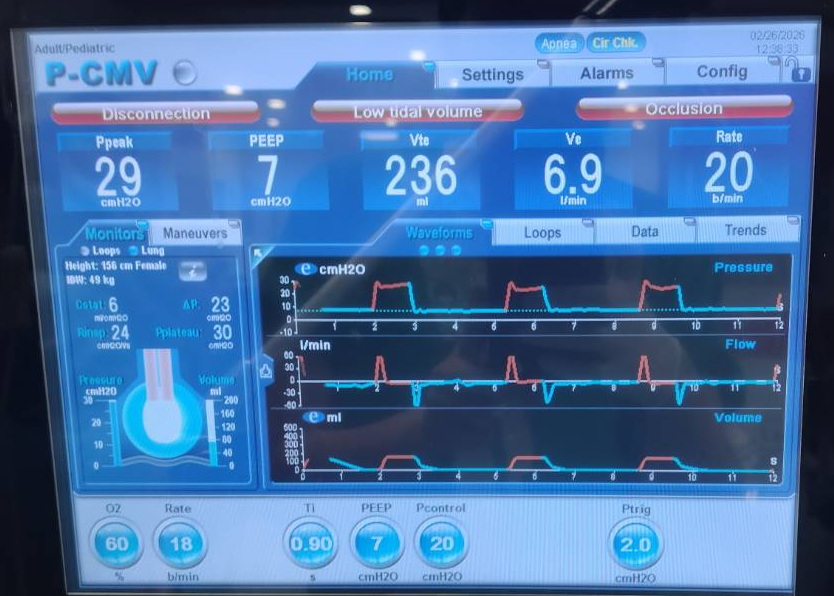
Case presentation: A 73-year-old Thai female with hepatitis C-related cirrhosis was admitted to the intensive care unit with septic shock and acute respiratory failure due to community-acquired multilobar pneumonia. She was intubated and mechanically ventilated in pressure-controlled mode. After receiving a fentanyl bolus of 50 mcg followed by a continuous infusion of 50 mcg/hour, she developed progressive patient-ventilator dyssynchrony with low tidal volume and worsening hypercapnia despite ventilator adjustments. Physical examination revealed a diffuse rigid abdominal wall. Ventilator flow-time waveforms suggested markedly reduced respiratory compliance. FIRCS was suspected. After discontinuation of fentanyl, incremental intravenous naloxone was administered. A total dose of 0.2 mg resulted in rapid improvement in tidal volume, minute ventilation, and ventilator waveform patterns within one minute. Recurrent symptoms occurred one hour later and resolved after an additional naloxone dose.
Conclusions: FIRCS can occur even with relatively low-dose fentanyl infusion. Recognition of characteristic ventilator waveform patterns is helpful in early diagnosis and prompt treatment.
Downloads
References
Tammen AJ, Brescia D, Jonas D, Hodges JL, Keith P. Fentanyl-induced rigid chest syndrome in critically ill patients. J Intensive Care Med. 2023;38:196-201.
Devarashetty S, Arty F, Vangala A, Abu Shanab A, Du D. The silent threat of wooden chest syndrome: Prompt management of fentanyl-induced muscle rigidity in the intensive care unit. Eur J Case Rep Intern Med. 2025;12:5363.
Marini JJ, Dries DJ. Analgesia, sedation, neuromuscular blockade, and delirium. In: Marini JJ, Dries DJ, eds. Critical Care Medicine: The Essentials and More. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2019: p.357.
McElrath C, Chew I, Lam T. The diagnosis of fentanyl-induced chest wall rigidity: A case report. Pain Med Case Rep. 2024;8:209-11.
Hill SA. Pharmacokinetics of drug infusions. Contin Educ Anaesth Crit Care Pain. 2004;4:76-80.
Flynn BC, Miranda HG, Mittel AM, Moitra VK. Stepwise ventilator waveform assessment to diagnose pulmonary pathophysiology. Anesthesiology. 2022;137:85-92.
Williamson J, Kermanizadeh A. A review of toxicological profile of fentanyl—A 2024 update. Toxics. 2024;12:690.
Cavallo D, Kelly E, Henderson G, Abdala Sheikh AP. Comparison of the effects of fentanyls and other μ opioid receptor agonists on the electrical activity of respiratory muscles in the rat. Front Pharmacol. 2023;14:1277248.
Marini JJ, Dries DJ. Thermal disorders. In: Marini JJ, Dries DJ, eds. Critical Care Medicine: The Essentials and More. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2019: p.602-608.
Devarashetty S, Arty F, Vangala A, Abu Shanab A, Du D. The silent threat of wooden chest syndrome: prompt management of fentanyl-induced muscle rigidity in the intensive care unit. Eur J Case Rep Intern Med. 2024;12:5363.
Ramathibodi Poison Center. Naloxone [Internet]: Ramathibodi Poison Center, Faculty of Medicine Ramathibodi Hospital, Mahidol University, 2020. [cited 2026 Apr 20]. Available from: https://www.rama.mahidol.ac.th/poisoncenter/sites/default/files/public/pdf/books/Antidote_book5-04_Naloxone.pdf.
Drägerwerk AG & Co. KGaA. Vista 120 S patient monitoring solution (PI 100918) [Internet]. Lübeck (Germany): Drägerwerk AG & Co. KGaA; 2024 [cited 2026 Apr 20]. Available from: https://www.draeger.com/Content/Documents/Products/Vista-120-S-pi-100918-en-MASTER.pdf.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 The Thai Society of Critical Care Medicine

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.




