JOB STRESS AND EFFECT TO SLEEP QUALITY AMONG POLICE OFFICERS IN MUEANG DISTRICT, PHRAE PROVINCE, THAILAND
Main Article Content
Abstract
Purpose: The paper aims to: estimate the prevalence of poor sleep and determine the relationship among demographic characteristic data, characteristics of police, covariate factors or behavioral factors, job stress, and sleep quality.
Methods: This study was cross-sectional study which approached 244 Thai police in Mueang District, Phrae Province, Thailand. By systemic random sampling technique. Data were collected by self-administrative questionnaire to find demographic data, covariate factors, behavior factors, job characteristics, job stress, and sleep quality during working as a police officer.
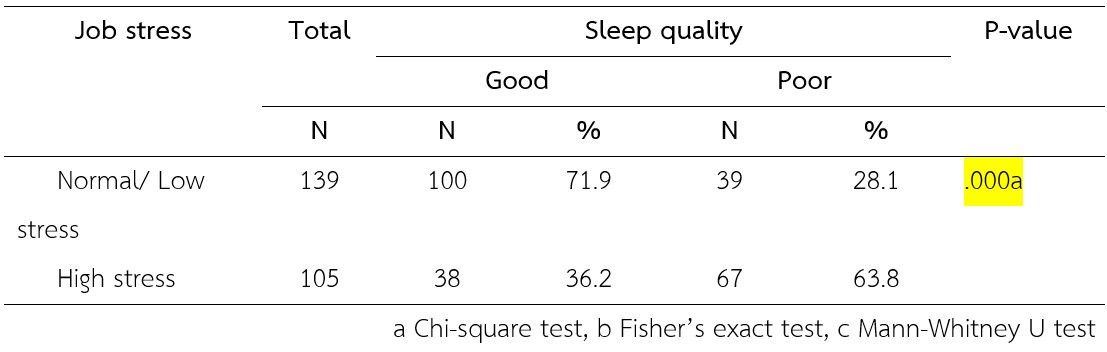
Findings: The findings highlight that mechanism of sleep, sleep quality, job stress, and police officer. Ever have an estimate 96.7% mentioned that they had a poor sleep quality and 3.3% had a good sleep quality. Police who have low stress or normal were assessed good sleep quality 100 people (71.9%) and poor sleep quality 39 people (28.1%). While who have high stress 38 (36.2%) were assessed good sleep quality and 67 police (63.8%) as poor sleep quality. Job stress was associated with sleep quality (p-value=0.000)
Originality/value: The paper presents general data, covariate factors, characteristics of police and police job stress among police officers in Mueang district, Phare province, Thailand. It also provides the associations of sleep quality.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Agency. (2008). Mobile phone radiation disrupts sleep, causes headaches. Retrieved from http://articles.econo mictimes.indiatimes.com/2008-01-21/news/27697646_1_mobile-phone-radiation-phones-from-exposure-sce narios-bengt-arnetz
Akololo, J. (2011). Kenya Police Demoralized. Kenya Broadcasting Corporation. Nairobi Kenya
Anshel, M. H. (2000). A conceptual model and implications for coping with stressful events inpolice work. Criminal Justice and Behavior, 27 (3), 375.
Atkinson, G., & Davenne, D. (2007). Relationships between sleep, physical activity and human health. Physiology & Behavior. 90(0), 229–235.
Better-Sleep-Guide.com. Benefit of Sleep. Retrieved from http://better-sleep-guide.com/benefits-of-sleep
Brough, J & Frane, R (2004). Predicting Police Job Satisfaction Work Well-Being And Turnover Intentions, the Role of Social Support and Police Organizational Variables. New Zealand journal of psychology 33:8-1
Brown (2007). From Cult of Masculinity to Smart Macho Gender Perspectives on Police Occupational Culture. In Neill M. O, Marks &Singh, A.M (Eds). Police Occupational Culture New Debates and Discussion Pp189-210.Oxford Elsevier
Buysse DJ, R. C. (1990). Insomnias. In: Thorpy MJ, ed. Handbook of Sleep Disorders. New York. Marcel Dekker Inc (375-433).
Buysse, D. J., Reynolds, C. F., Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry research, 28(2), 193-213.
Chaiarj S, Panya P. Insomnia and related factors. The Thai Journal of Nursing Council. 2005;20(2):1-12.
Chellappa SL, Steiner R, Blattner P, Oelhafen P, Gotz T, Cajochen C. Non-visual effects of light on melatonin, alertness and cognitive performance: can blue-enriched light keep us alert? PLoS One. 2011;6(1):e16429.
Danilov Y. Melatonin in chronic pain syndromes. Neuroscience and behavioral physiology. 2017;47(7):806-12.
Dariush D, Maryam M, Mohammad K. Happiness & health: The Biological Factors- Systematic Review Article. Iranian Journal Public Health. 2014;43(11):1468-77.
Demirci, K., Akgönül, M., & Akpinar, A. (2015). Relationship of smartphone use severity with sleep quality, depression, and anxiety in university students. Journal of Behavioral Addictions, 4(2), 85-92. doi:10.1556/2006.4.2015.010
Doi Y, Minowa M, Tango T. Impact and correlates of poor sleep quality in Japanese White-Collar employees. Sleep. 2003;26(4):467-71.
Garcia A, Ramirez C, Aguillon A, Tirado V, Paredes L, Ibarra A, et al. Smartphone use during sleep time in Mexican adolescents. Sleep Medicine. 2017;40:e106-e7.
Hall, K. (2013). How Mobile Phones Affect Sleep (INFOGRAPHIC). Retrieved from http://www.huffingtonpost.com/2013/02/15/phones-sleep-mobile-_n_2680805.html
Hirasawa, U., & Fujimoto, M. Age-Based Mobile Phone Usage Survey. Retrieved from http://www.hakuhodody-media.co.jp/english/newsrelease/reports/20070507_64.html
Kalhori, S. M., Mohammadi, M. R., Alavi, S. S., Jannatifard, F., Sepahbodi, G., Reisi, M. B., ... & Kasvaee, V. H. (2015). Validation and Psychometric Properties of Mobile Phone Problematic Use Scale (MPPUS) in University Students of Tehran. Iranian journal of psychiatry, 10(1), 25.
Kawasaki N, T. S., Ogata F, Burapadaja S, Loetkham C, Nakamura T, Tanada S. (2006). Survey on cellular phone usage on students in Thailand. Journal of Physiological Anthropology, 25(6), 377-382.
Leproult R, Colecchia EF, L'Hermite-Balériaux M, Van Cauter E. Transition from dim to bright light in the morning induces an immediate elevation of cortisol levels. The Journal of Clinical Endocrinology & Metabolism. 2000;86(1).
Lotrakul M, Sumrithe S, Saipanish R. Reliability and validity of the Thai version of the PHQ-9. BMC Psychiatry. 2008;8:46.
Lucia A, D. B., Hoyos J, Fernandez C, Villa G, Bandres F, et al... 2001; 35:424–30. (2001). Hormone levels of world Class
McCreary, D. R., & Thompson, M. M. (2006). Development of two reliable and validmeasures of stressors in policing: The operational and organizational police stressquestionnaires. International Journal of Stress Management, 13(4), 494-518.
Miller, L. (2007). Police families: Stresses, syndromes, and solutions. American Journal of Family Therapy, 35(1), 21-40. doi:10.1080/01926180600698541.
Mortazavi, M. J., Mortazavi, A., Habibzadeh, P., & Mortazavi, G. (2016). Is it Blue Light or Increased Electromagnetic Fields which Affects the Circadian Rhythm in People Who Use Smartphones at Night. Iran J Public Health, 45, 405-406.
National Institutes of Health, National Heart, Lung, and Blood Institute. (2011). Your guide to healthy sleep.
National Sleep Foundation. Smoking, head injury, esticide use may be risk factors for rare sleep disorder 2012; [update: 2012 Jun 27; cited 2018 May 25]. Available from: http://www.sleepfoundation.org/sleep-news/smoking-head-injury-pesticide-use-may-be-risk-factors-rare-sleep-disorder/page/0/1.
National Sleep Foundation. Melatonin and sleep 2015; [update: 2017 Jul 15; cited 2018 May 25]. Available from: https://sleepfoundation.org/sleep-topics/melatonin-and-sleep.
National Sleep Foundation. Asthma and sleep 2013 [update: 2017 Jul 1; cited 2018 May 25]. Available from: https://sleepfoundation.org/sleep-disorders-problems/asthma-and-sleep.
Peter L. Franzen DJ. Sleep disturbances and depression risk relationships for subsequent depression and therapeutic implications. Journal of Dialogues in Clinical Neuroscience 2008;10(4):473-81.
Pietrangelo A., W. S. (2014). Effects of Sleep Deprivation on the Body. Retrieved from http://www.healthline.com/health/sleep-deprivation/effects-on-body
Portas CM, Krakow K, Allen P, Josephs O, Armony JL, Frith CD. Auditory processing across the sleep-wake cycle: simultaneous EEG and fMRI monitoring in humans. Journal of Neuron 2000; 28: 991-9. 9
Sabanayagam C, Shankar A. The association between active smoking, smokeless tobacco, second-hand smoke exposure and insufficient sleep. Sleep Med. 2011;12(1):7-11.
Sanchez-Barcelo EJ, Rueda N, Mediavilla MD, Martinez-Cue C, Reiter RJ. Clinical Uses of Melatonin in Neurological Diseases and Mental and Behavioural Disorders. Current Medicinal Chemistry. 2017;24(35):3851-78
Shim J, Kang SW. Behavioral Factors Related to Sleep Quality and Duration in Adults. Journal of Lifestyle Medicine 2017;7(1):18-26.
Shimizu N, Nagai Y, Yamamoto Y, Minami T, Hayashi T, Tsuji H, et al. Survey on lower urinary tract symptoms and sleep disorders in patients treated at urology departments. Nat Sci Sleep. 2013;5:7-13.
Tel H. Sleep quality and quality of life among the elderly people. Neurology, Psychiatry and Brain Research. 2013;19(1):48-52.
Thai Health Promotion Foundation. nsomnia in Thai people Retrieved from http://www.thaihealth.or.th/Content/Washington, D. C. U. S. D. o. H. a. H. S.,
V. Lohsoonthorn, e. a. (2013). Sleep Quality and Sleep Patterns in Relation to Consumption of Energy Drinks, Caffeinated Beverages and Other Stimulants