Factors Related to Health-Related Quality of Life among Persons with Systemic Lupus Erythematosus in Wenzhou, China
คำสำคัญ:
Health-related quality of life, SLE symptoms, Depression, Social support, Self-careบทคัดย่อ
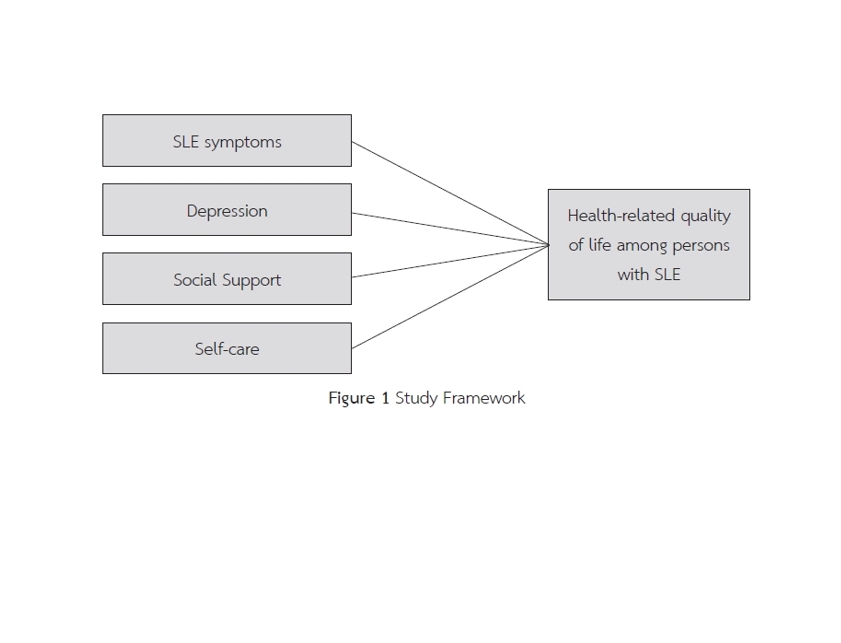
Systemic lupus erythematosus (SLE) is a major global health issue affecting patients' health-related quality of life (HRQOL). This research aimed to examine HRQOL in persons with SLE and to examine the relationships between SLE symptoms, depression, social support, self-care, and HRQOL in this population. Ninety-two persons with SLE were recruited by simple random sampling from one hospital in Wenzhou, Zhejiang Province, China. Instruments included the Demographic Information Questionnaire, the SLE Symptom Checklist (SSC), the Chinese version of the Patient Health Questionnaire (PHQ-9), the Chinese version of the Perceived Social Support Scale (PSSS), the Exercise of Self-Care Agency (ESCA), and the Chinese version of the Lupus Quality of Life (LupusQoL). Data were analyzed by using descriptive statistics and the Pearson correlation coefficient.
The results revealed that the mean score of HRQOL among persons with SLE was 62.8 out of 100 (SD = 19.49). Self-care and social support were positively correlated with HRQOL (r = .370, p < .01; r = .407, p < .01, respectively). At the same time, depression and SLE symptoms showed negative correlations with HRQOL (r = -.466, p < .01; r = -.436, p < .01, respectively).
The findings underscore the necessity and relevance of targeted interventions focused on improving the HRQOL of individuals with SLE. To improve the quality of life in this population, nurses should develop an intervention that focuses on controlling SLE symptoms, preventing depression, and promoting SLE self-care and social support.
เอกสารอ้างอิง
Askanase, A. D., & Furie, R. A. (2022). A narrative review of repository corticotropin injection for the treatment of systemic lupus erythematosus. Advances in Therapy, 39(7), 3088-3103. https://doi.org/10.1007/s12325-022-02160-y
Blumenthal, J. A., Burg, M. M., Barefoot, J., Williams, R. B., Haney, T., & Zimet, G. (1987). Social support, type A behavior, and coronary artery disease. Psychosomatic Medicine, 49(4), 331-340. https://journals.lww.com/psychosomaticmedicine/fulltext/1987/07000/social_support,_type_a_behavior,_and_coronary.2.aspx
Cao, L., Zhang, X., Wang, Y., & Zhao, B. (2023). Continuum of care intervention in adolescent systemic lupus erythematosus. Journal of Qilu Nursing, 29(11), 158-160.
Carter, E. E., Barr, S. G., & Clarke, A. E. (2016). The global burden of SLE: Prevalence, health disparities and socioeconomic impact. Nature Reviews Rheumatology, 12(10), 605-620. https://doi.org/10.1038/nrrheum.2016.137
Fernández-Llanio-Comella, N., San-Martín-Álvarez, A., Vivas-Consuelo, D., Jordán-Alfonso, A., Ivorra, J. R., Vela-Casasempere, P., & Saurí-Ferrer, M. (2016). Health-related quality of life in patients with systemic lupus erythematosus (SLE): A Spanish study based on patient reports. Value in Health, 19(7), A617. https://doi.org/10.1016/j.jval.2016.09.1555
Ferrans, C. E., Zerwic, J. J., Wilbur, J. E., & Larson, J. L. (2005). Conceptual model of health-related quality of life. Journal of Nursing Scholarship, 37(4), 336-342.
Figueiredo-Braga, M., Cornaby, C., Cortez, A., Bernardes, M., Terroso, G., Figueiredo, M., ... Poole, B. D. (2018). Depression and anxiety in systemic lupus erythematosus: The crosstalk between immunological, clinical, and psychosocial factors. Medicine (Baltimore), 97(28), e11376. https://doi.org/10.1097/MD.0000000000011376
Garcia, B. E. C., Pesantez, M. P. C., Carbaca, V. X. V., Alvarez, R. A. V., Betancourt, V. J. M., Barriga, J. P. G., Moreno, M. G. H., & Carchipulla, D. G. G. (2024). Systemic lupus erythematosus: Update on the diagnosis, prevalence, clinical management, inflammatory markers, new horizons in the pathogenesis, manifestations and progress in treatment. EPRA International Journal of Multidisciplinary Research (IJMR), 10(2), 317-325.
Gottlieb, B. H., & Bergen, A. E. (2010). Social support concepts and measures. Journal of Psychosomatic Research, 69(5), 511-520. https://doi.org/10.1016/j.jpsychores.2009.10.001
He, X., Lloyd, E., Cooper, S., Li, L., Chauhan, D., Juliao, P., ... Bao, C. (2023). Healthcare costs and utilization for patients with systemic lupus erythematosus in China: A national claims database study. Value in Health Regional Issues, 37, 88-96. https://doi.org/10.1016/j.vhri.2023.03.007
Huang, L., Jiang, Q., & Ren, W. (1996). The relationship between coping style, social support and psychosomatic symptoms of cancer patients. Chinese Mental Health Journal, 10(4), 160-161.
Janke, M. C., Son, J. S., Jones, J. J., Payne, L. L., & Anderson, S. K. (2015). Leisure patterns and their associations with arthritis-related self-management and health. Therapeutic Recreation Journal, 49(4), 281. https://doi.org/10.18666/TRJ-2015-V49-I4-6294
Jiang, H. Z., Lin, Z. G., Li, H. J., Du, Q., Tian, W., Wang, S. Y., ... Mei, Y. F. (2018). The Chinese version of the SLEQOL is a reliable assessment of health-related quality of life in Han Chinese patients with systemic lupus erythematosus. Clinical Rheumatology, 37(1), 151-160. https://doi.org/10.1007/s10067-017-3910-4
Jönsen, A., Hjalte, F., Willim, M., Carlsson, K. S., Sjöwall, C., Svenungsson, E., ... Pettersson, S. (2016). Direct and indirect costs for systemic lupus erythematosus in Sweden: A nationwide health economic study based on five defined cohorts. Seminars in Arthritis & Rheumatism, 45(6), 684-690. https://doi.org/10.1016/j.semarthrit.2015.11.013
Kaplan, R. M., & Hays, R. D. (2022). Health-related quality of life measurement in public health. Annual Review of Public Health, 43, 355-373. https://doi.org/10.1146/annurev-publhealth-052120-012811
Kearney, B. Y., & Fleischer, B. J. (1979). Development of an instrument to measure exercise of self-care agency. Research in Nursing & Health, 2(1), 25-34. https://doi.org/10.1002/nur.4770020105
Kusnanto, K., Sari, N. P. W. P., Harmayetty, H., Efendi, F., & Gunawan, J. (2018). Self-care model application to improve self-care agency, self-care activities, and quality of life in patients with systemic lupus erythematosus. Journal of Taibah University Medical Sciences, 13(5), 472-478. https://doi.org/10.1016/j.jtumed.2018.07.002
Li, M., Zhang, Z., Zhang, L., & Gu, Y. (2022). Mediating effects of navigating social support in patients with systemic lupus erythematosus between sense of hope and quality of life. Chinese Evidence-Based Nursing, 8(14), 1955-1960. https://doi.org/10.2478/rir-2020-0009
Lou, K., Schlencker, A., Mertz, P., Martin, T., & Arnaud, L. (2021). Fatigue in systemic lupus erythematosus: An update on its impact, determinants, and therapeutic management. Journal of Clinical Medicine, 10(17), 3996. https://doi.org/10.3390/jcm10173996
Mazzoni, D., & Cicognani, E. (2016). Positive and problematic support, stress, and quality of life in patients with systemic lupus erythematosus. Anxiety, Stress, & Coping, 29(5), 542-551. https://doi.org/10.1080/10615806.2015.1134785
McElhone, K., Abbott, J., Shelmerdine, J., Bruce, I. N., Ahmad, Y., Gordon, C., ... Teh, L. S. (2007). Development and validation of a disease-specific health-related quality of life measure, the LupusQoL, for adults with systemic lupus erythematosus. Arthritis Care & Research, 57(6), 972-979. https://doi.org/10.1002/art.22881
Mizukami, A., Trinh, M. T., Hoang, T. P., Shibanuma, A., Ong, K. I. C., & Jimba, M. (2023). Determinants of health-related quality of life among patients with systemic lupus erythematosus in Hanoi, Vietnam. BMC Rheumatology, 7(1), 16. https://doi.org/10.1186/s41927-023-00339-6
Rees, F., Doherty, M., Grainge, M. J., Lanyon, P., & Zhang, W. (2017). The worldwide incidence and prevalence of systemic lupus erythematosus: A systematic review of epidemiological studies. Rheumatology, 56(11), 1945-1961. https://doi.org/10.1093/rheumatology/kex260
Spitzer, R. L., Kroenke, K., Williams, J. B. W., & Patient Health Questionnaire Primary Care Study Group. (1999). Validation and utility of a self-report version of PRIME-MD: The PHQ primary care study. JAMA, 282(18), 1737-1744. https://doi.org/10.1001/jama.282.18.1737
Tamayo, T., Fischer-Betz, R., Beer, S., Winkler-Rohlfing, B., & Schneider, M. (2010). Factors influencing the health-related quality of life in patients with systemic lupus erythematosus: Long-term results (2001–2005) of patients in the German Lupus Erythematosus Self-Help Organization (LULA Study). Lupus, 19(14), 1606-1613. https://doi.org/10.1177/0961203310377090
Tian, J., Zhang, D., Yao, X., Huang, Y., & Lu, Q. (2023). Global epidemiology of systemic lupus erythematosus: A comprehensive systematic analysis and modeling study. Annals of the Rheumatic Diseases, 82(3), 351-356. https://doi.org/10.1136/ard-2022-223035
Wang, H., & Laffrey, S. C. (2000). Preliminary development and testing of instruments to measure self-care agency and social support of women in Taiwan. The Kaohsiung Journal of Medical Sciences, 16(9), 459-467. https://doi.org/10.6452/KJMS.200009.0459
Wang, S., Wu, B., Leng, L., Bucala, R., & Lu, L.-J. (2013). Validity of LupusQoL-China for the assessment of health-related quality of life in Chinese patients with systemic lupus erythematosus. PLOS ONE, 8(5), e63795. https://doi.org/10.1371/journal.pone.0063795
Wang, W., Bian, Q., Zhao, Y., Li, X., Wang, W., Du, J., ... Zhao, M. (2014). Reliability and validity of the Chinese version of the Patient Health Questionnaire (PHQ-9) in the general population. General Hospital Psychiatry, 36(5), 539-544. https://doi.org/10.1016/j.genhosppsych.2014.05.021
Wu, C. Y., Li, C. F., Wu, Q. J., Xu, J. H., Jiang, L. D., Gong, L., ... Chinese Systemic Lupus Erythematosus Treatment and Research Group Registry IX. (2017). Clinical features and survival of childhood-onset systemic lupus erythematosus in China. Chinese Medical Journal, 130(11), 1276-1282. https://doi.org/10.4103/0366-6999.206346
Xu, Q., Liu, D., Zeng, F., Luo, H., & Li, Y. (2019). Social support and management strategies for chronic disease in patients with systemic lupus erythematosus. Journal of Central South University. Medical Sciences, 44(1), 67-73. https://doi.org/10.11817/j.issn.1672-7347.2019.01.011
Yan, P., Zhou, X., Deng, D., & Fu, P. (2012). Evaluation of quality of life in patients with systemic lupus erythematosus using the Systemic Lupus Erythematosus Symptom Specificity Scale. Guangdong Medical Journal, 33, 2822-2825. https://doi.org/10.13820/j.cnki.gdyx.2012.18.033
ดาวน์โหลด
เผยแพร่แล้ว
รูปแบบการอ้างอิง
ฉบับ
ประเภทบทความ
สัญญาอนุญาต

อนุญาตภายใต้เงื่อนไข Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.




