Factors Associated with Sexual Dysfunction among Men with Type 2 Diabetes Mellitus in Botswana
คำสำคัญ:
Sexual dysfunction, Men with type 2 diabetes mellitus, Couple satisfaction, Botswanaบทคัดย่อ
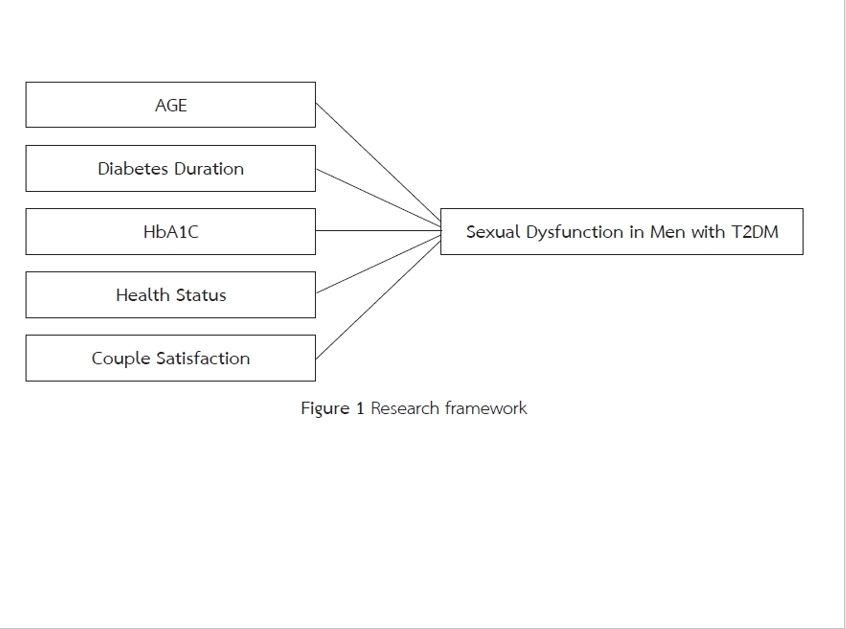
This descriptive correlational study aimed to examine the prevalence of sexual dysfunction and its associated factors, including age, health status, diabetes duration, HbA1C, and couple satisfaction with sexual dysfunction among men with T2DM in Botswana. Engel’s Biopsychosocial Model served as the conceptual framework (Engel, 2012). Simple random sampling was used to recruit 200 men with T2DM attending an outpatient diabetes clinic in Botswana. The tools used included a demographic questionnaire, the Short Form-12 (SF-12), the Couples Satisfaction Questionnaire (CSQ-4), and the Changes in Sexual Functioning Questionnaire (CSFQ-14). Data were analyzed using descriptive statistics and Pearson correlation.
Results revealed that 64.5% of participants had HbA1C levels ≥8%, indicating poor glycemic control (HbA1C ≥ 8%). 70 % (n = 140) of participants reported sexual dysfunction. Strong positive correlations were found with age (r = .547, p < .001), and moderate correlations were observed for diabetic duration (r = .375, p < .001). Weak positive correlations were observed with couple satisfaction (r = .189, p = .007), while negative correlations were observed with health status (r = - .235, p < .001). However, no significant correlation was found between sexual dysfunction and HbA1c levels.
Sexual dysfunction is highly prevalent among men with type 2 diabetes mellitus. Age, health status, diabetes duration, and couple satisfaction were significantly associated with sexual dysfunction. Healthcare interventions should focus on promoting overall health status, improving diabetes control, and providing couples counselling to enhance relationship quality, thereby improving sexual health outcomes in men with type 2 diabetes mellitus.
เอกสารอ้างอิง
Anderson, D., Laforge, J., Ross, M. M., Vanlangendonck, R., Hasoon, J., Viswanath, O., Kaye, A. D., & Urits, I. (2022). Male sexual dysfunction. Health Psychology Research, 10(3), 37533. doi:10.52965/001c.37533
Asadi, M., Ghasemzadeh, N., Nazarifar, M., & Niroumand Sarvandani, M. (2020). The effectiveness of emotion-focused couple therapy on marital satisfaction and positive feelings towards the spouse. Shahroud Journal of Medical Sciences, 6(4), 36–40. doi:10.22100/ijhs.v6i4.804
Asefa, A., Nigussie, T., Henok, A., & Mamo, Y. (2019). Prevalence of sexual dysfunction and related factors among diabetes mellitus patients in Southwest Ethiopia. BMC Endocrine Disorders, 19(1), 141. doi:10.1186/s12902-019-0473-1
Banday, M. Z., Sameer, A. S., & Nissar, S. (2020). Pathophysiology of diabetes: An overview. Avicenna Journal of Medicine, 10(4), 174–188. doi:10.4103/ajm.ajm_53_20
Centers for Disease Control and Prevention. (2024). Diabetes and men. Retrieved from https://www.cdc.gov/diabetes/risk-factors/diabetes-and-men.html
Chen, L., Shi, G. R., Huang, D. D., Li, Y., Ma, C. C., Shi, M., Su, B. X., & Shi, G. J. (2019). Male sexual dysfunction: A review of literature on its pathological mechanisms, potential risk factors, and herbal drug intervention. Biomed Pharmacother, 112, 108585. doi:10.1016/j.biopha.2019.01.046
Chung, E. (2019). Sexuality in ageing male: Review of pathophysiology and treatment strategies for various male sexual dysfunctions. Med Sci (Basel), 7(98). 1-7 doi:10.3390/medsci7100098
Clayton, A. H., Pradko, J. F., Croft, H. A., Montano, C. B., Leadbetter, R. A., Bolden-Watson, C., . . . Metz, A. (2002). Prevalence of sexual dysfunction among newer antidepressants. Journal of Clinical Psychiatry, 63(4), 357-366. https://doi.org/10.4088/jcp.v63n0414
Cooper, S., Leon, N., Namadingo, H., Bobrow, K., & Farmer, A. J. (2018). My wife's mistrust. That's the saddest part of being a diabetic: A qualitative study of sexual well-being in men with Type 2 diabetes in sub-Saharan Africa. PLoS ONE, 13(9), e0202413. https://doi.org/10.1371/journal.pone.0202413
Corona, G., Isidori, A. M., Aversa, A., Bonomi, M., Ferlin, A., Foresta, C., . . . Lombardo, F. (2020). Male and female sexual dysfunction in diabetic subjects: Focus on new antihyperglycemic drugs. Reviews in Endocrine and Metabolic Disorders, 21(1), 57-65. https://doi.org/10.1007/s11154-019-09535-7
Das, M., Angeli, F., Krumeich, A. J. S. M., & van Schayck, O. C. P. (2018). The gendered experience with respect to health-seeking behaviour in an urban slum of Kolkata, India. International Journal for Equity in Health, 17(24), 1 - 14. https://doi.org/10.1186/s12939-018-0738-8
Defeudis, G., Mazzilli, R., Tenuta, M., Rossini, G., Zamponi, V., Olana, S., . . . Gianfrilli, D. (2022). Erectile dysfunction and diabetes: A melting pot of circumstances and treatments. Diabetes/Metabolism Research and Reviews, 38(2), e3494. https://doi.org/10.1002/dmrr.3494
Elterman, D. S., Bhattacharyya, S. K., Mafilios, M., Woodward, E., Nitschelm, K., & Burnett, A. L. (2021). The quality of life and economic burden of erectile dysfunction. Research and Reports in Urology, 13, 79-86. https://doi.org/10.2147/rru.S283097
Engel, G. L. (2012). The need for a new medical model: A challenge for biomedicine. Psychodynamic Psychiatry, 40(3), 377-396. https://doi.org/10.1521/pdps.2012.40.3.377
Faselis, C., Katsimardou, A., Imprialos, K., Deligkaris, P., Kallistratos, M., & Dimitriadis, K. (2020). Microvascular complications of Type 2 diabetes mellitus. Current Vascular Pharmacology, 18(2), 117-124. https://doi.org/10.2174/1570161117666190502103733
Funk, J. L., & Rogge, R. D. (2007). Testing the ruler with item response theory: Increasing precision of measurement for relationship satisfaction with the Couples Satisfaction Index. Journal of Family Psychology, 21(4), 572-583. https://doi.org/10.1037/0893-3200.21.4.572
Getie Mekonnen, E., Yeshita, H. Y., & Bishaw Geremew, A. (2021). Sexual dysfunction among men with diabetes mellitus attending chronic out-patient department at the three hospitals of Northwest Amhara region, Ethiopia: Prevalence and associated factors. PLoS ONE, 16(8), e0256015. https://doi.org/10.1371/journal.pone.0256015
Heidari, M., Ghodusi, M., Rezaei, P., Kabirian Abyaneh, S., Sureshjani, E. H., & Sheikhi, R. A. (2019). Sexual function and factors affecting menopause: A systematic review. Journal of Menopausal Medicine, 25(1), 15-27. https://doi.org/10.6118/jmm.2019.25.1.15
Hurisa, A., & Negera, G. (2020). Erectile dysfunction among diabetic patients in a tertiary hospital of Southwest Ethiopia. The Open Public Health Journal, 13(1), 240-245. https://doi.org/10.2174/1874944502013010240
Ibrahim, A. A., Akindele, M. O., Ganiyu, S. O., Kaka, B., Abdullahi, B. B., Sulaiman, S. K., & Fatoye, F. (2020). The Hausa 12-item short-form health survey (SF-12): Translation, cross-cultural adaptation and validation in mixed urban and rural Nigerian populations with chronic low back pain. PLoS ONE, 15(5), e0232223. https://doi.org/10.1371/journal.pone.0232223
Lugg, W. (2022). The biopsychosocial model – history, controversy and Engel. Australasian Psychiatry, 30(1), 55-59. https://doi.org/10.1177/10398562211037333
Olivier, B. (2017). Introductory chapter: Sexual dysfunction - introduction and perspective. In B. Olivier (Ed.), Sexual dysfunction (pp. 3-10). London, United Kingdom: IntechOpen. https://doi.org/10.5772/intechopen.69092
Omani-Samani, R., Maroufizadeh, S., Ghaheri, A., Amini, P., & Navid, B. (2018). Reliability and validity of the Kansas Marital Satisfaction Scale (KMSS) in infertile people. Middle East Fertility Society Journal, 23(2), 154-157. https://doi.org/10.1016/j.mefs.2017.10.005
Rwegerera, G. M., Moshomo, T., Gaenamong, M., Oyewo, T. A., Gollakota, S., Rivera, Y. P., . . . Habte, D. (2018). Health-related quality of life and associated factors among patients with diabetes mellitus in Botswana. Alexandria Journal of Medicine, 54(2), 111-118. https://doi.org/10.1016/j.ajme.2017.05.010
Selvin, E. (2021). Hemoglobin A1c—Using epidemiology to guide medical practice: Kelly West Award Lecture 2020. Diabetes Care, 44(10), 2197-2204. https://doi.org/10.2337/dci21-0035
Shiferaw, W. S., Akalu, T. Y., & Aynalem, Y. A. (2020). Prevalence of erectile dysfunction in patients with diabetes mellitus and its association with body mass index and glycated hemoglobin in Africa: A systematic review and meta-analysis. International Journal of Endocrinology, 2020, 5148370. https://doi.org/10.1155/2020/5148370
Thongtang, P., & Seesawang, J. (2020). Erectile Dysfunction and Quality of Life among Diabetic Men: A Systematic Review of Quantitative Studies. Nursing Science Journal of Thailand, 38(1), 4-18.
United Nations. (2017). Principles and recommendations for population and housing censuses (Rev. 3). New York, NY: Author. Retrieved from https://unstats.un.org/unsd/demographic-social/Standards-and-Methods/files/Principles_and_Recommendations/Population-and-Housing-Censuses/Revision_3/P&R_Symbol-E.pdf
Ware, J., Jr., Kosinski, M., & Keller, S. D. (1996). A 12-item short-form health survey: Construction of scales and preliminary tests of reliability and validity. Medical Care, 34(3), 220-233. https://doi.org/10.1097/00005650-199603000-00003
World Health Organization. (2022). International statistical classification of diseases and related health problems. Retrieved from https://www.who.int/standards/classifications/classification-of-diseases
World Health Organization. (2024). Diabetes. Retrieved from https://www.who.int/news-room/fact-sheets/detail/diabetes
Zarif Golbar Yazdi, H., Aghamohammadian Sharbaf, H., Kareshki, H., & Amirian, M. (2020). Infertility and psychological and social health of Iranian infertile women: A systematic review. Iranian Journal of Psychiatry, 15(1), 67–79. https://doi.org/10.18502/ijps.v15i1.2441
ดาวน์โหลด
เผยแพร่แล้ว
รูปแบบการอ้างอิง
ฉบับ
ประเภทบทความ
สัญญาอนุญาต

อนุญาตภายใต้เงื่อนไข Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.




