Nutritional status of mechanically ventilated critically ill patients in a university-based hospital in Northern Thailand
Malnutrition in mechanically ventilated medical critical care unit patients
DOI:
https://doi.org/10.54205/ccc.v34.279855Keywords:
Critically ill medical patients, Malnutrition, Mechanical ventilation, NT 2013, Prevalence, Risk factorsAbstract
Background: Malnutrition is common in mechanically ventilated critically ill patients and contributes to poor outcomes. This study evaluated its prevalence and associated factors in a medical critical care unit (MCCU).
Method: A retrospective study of adult mechanically ventilated patients admitted between May 2021 and July 2024. Nutritional status was assessed using NT 2013, with day-7 status used for outcome analysis. Logistic regression identified factors associated with malnutrition.
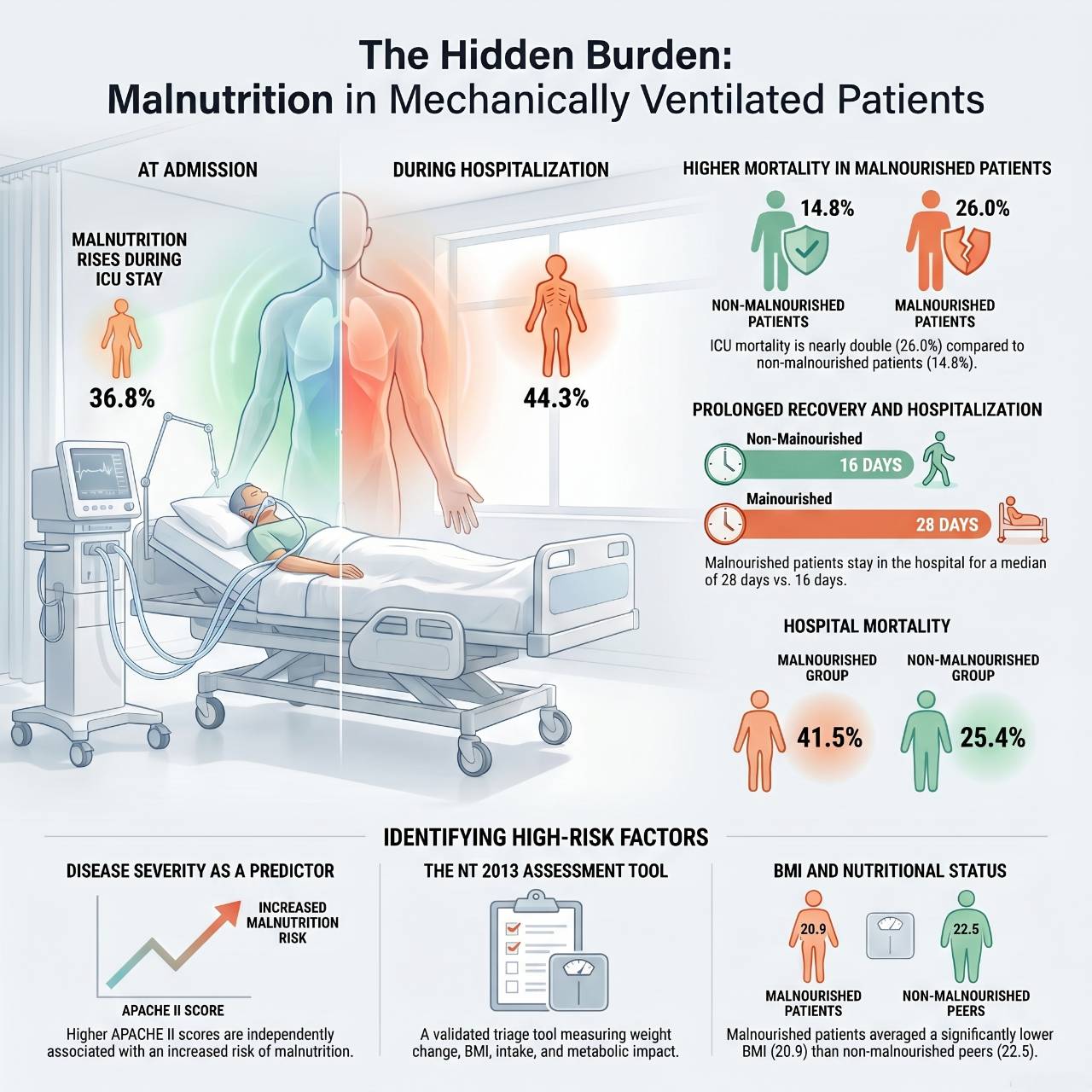
Result: Among 334 patients, malnutrition prevalence was 36.8% at admission and increased to 44.3% during hospitalization. Malnourished patients had lower BMI and higher severity scores (APACHE II, SAPS II, SOFA). They also experienced worse outcomes, including higher MCCU mortality (26.0% vs. 14.8%), higher in-hospital mortality (41.5% vs. 25.4%), longer mechanical ventilation, and longer hospital stays. These associations persisted in patients hospitalized ≥7 days. Independent factors associated with malnutrition were younger age (aOR 0.97) and higher APACHE II score (aOR 1.07).
Conclusion: Malnutrition is frequent and worsens during MCCU stay, and is linked to poorer clinical outcomes. Early assessment, close monitoring, and timely individualized nutritional support are essential.
Downloads
References
Muangin W, Akarawanasakun B, Phromrin M, Uangnakhon M, Mongkhonittivech N. Development of a nursing care model for critically-ill patients based on the FAST HUG concept in a Medical and Surgical Intensive Care Unit at Chiang Rai Prachanukroh Hospital. Nursing Journal CMU. 2021;48:308–23.
Manrique S, Ruiz-Botella M, Murillo N, Canelles S, Victoria ID, Samper MA, et al. Impact of mechanical power on ICU mortality in ventilated critically ill patients: a retrospective study with continuous real-life data. Eur J Med Res. 2024;29:491.
Oami T, Yamamoto A, Ishida S, Kondo K, Hata N, Oshima T. Critical care nutrition from a metabolic point of view: A narrative review. Nutrients. 2025;17.
Lew CCH, Wong GJY, Cheung KP, Chua AP, Chong MFF, Miller M. Association between malnutrition and 28-day mortality and intensive care length-of-stay in the critically ill: A prospective cohort study. Nutrients. 2018;10:10.
Benyapad P, Kongsaman P. Nutritional support in critically ill patients: the challenges of nurses role. Vajira Medical Journal : Journal of Urban Medicine. 2019;63:219–30.
Kulnitichai W. Nursing care for continuous monitoring of the malnutrition in critical patients. Thai Journal of Cardio-Thoracic Nursing. 2019;30:2–16.
Doganay M, Halil MG, Uyar M, Kocatakan P, Dikmeer A, Kelleci Cakir B, et al. Prevalence of malnutrition risk in hospitalized patients: a large nationwide study. Journal of Health, Population and Nutrition. 2025;44:137.
Kalaiselvan MS, Arunkumar AS, Renuka MK, Sivakumar RL. Nutritional adequacy in mechanically ventilated patient: are we doing enough? Indian J Crit Care Med. 2021;25:166–71.
Wełna M, Adamik B, Kübler A, Goździk W. The NUTRIC score as a tool to predict mortality and increased resource utilization in intensive care patients with sepsis. Nutrients. 2023;15:1648.
Majumdar A, Saraf S, Sahu C, Verma K, Vishwakarma P. Current perspectives on malnutrition and immunomodulators bridging nutritional deficiencies and immune health. Future Journal of Pharmaceutical Sciences. 2025;11.
Litchford MD, Dorner B, Posthauer ME. Malnutrition as a Precursor of Pressure Ulcers. Adv Wound Care (New Rochelle). 2014;3:54–63.
Osooli F, Abbas S, Farsaei S, Adibi P. Identifying critically ill patients at risk of malnutrition and underfeeding: a prospective study at an academic hospital. Adv Pharm Bull. 2019;9:314–20.
Verheul EAH, Dijkink S, Krijnen P, Hoogendoorn JM, Arbous S, Peters R, et al. Prevalence, incidence, and complications of malnutrition in severely injured patients. Eur J Trauma Emerg Surg. 2025;51:72.
Rezaeian M, Monfared-Parizi S, Mousavi Shirazifard Z, Sayadi A, Khodadadi H, Ghaseminasab-Parizi M. Evaluation of nutritional intake and malnutrition in critically ill patients and its relationship with 28-day death. Sci Rep. 2025;15:15677.
Díaz Chavarro BC, Romero-Saldaña M, Assis Reveiz JK, Molina-Recio G. Impact of nutritional screening on mortality and intensive care unit length of stay. Front Nutr. 2025;12:1474039.
Hospital MNCM. Nutrition Assessment Tool (NT 2013). Chiang Mai, Thailand, Maharaj Nakorn Chiang Mai Hospital. 2013.
Chittawatanarat K, Chaiwat O, Morakul S, Kongsayreepong S. Outcomes of nutrition status assessment by Bhumibol Nutrition Triage/Nutrition Triage (BNT/NT) in multicenter THAI-SICU study. J Med Assoc Thai. 2016;99 Suppl 6:S184–s92.
Komindrg S, Tangsermwong T, Janepanish P. Simplified malnutrition tool for Thai patients. Asia Pac J Clin Nutr. 2013;22:516–21.
Knaus WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II: a severity of disease classification system. Crit Care Med. 1985;13:818–29.
Le Gall JR, Lemeshow S, Saulnier F. A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. Jama. 1993;270:2957–63.
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonça A, Bruining H, et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med. 1996;22:707–10.
Prammanasudh B, Trakulhoon V. NT 2013: A Recommended nutrition screening and nutrition format for practical clinical use in hospitalized patients in Thailand. The Thai Journal of Surgery. 2019;40:107–16.
Heyland DK, Dhaliwal R, Jiang X, Day AG. Identifying critically ill patients who benefit the most from nutrition therapy: the development and initial validation of a novel risk assessment tool. Crit Care. 2011;15:R268.
Detsky AS, McLaughlin JR, Baker JP, Johnston N, Whittaker S, Mendelson RA, et al. What is subjective global assessment of nutritional status? JPEN J Parenter Enteral Nutr. 1987;11:8–13.
Gongmuang L, Bannaasan B, Kitsripisarn S. The effects of an educative supportive program on the nutrition self-care behavior and nutritional status among colorectal cancer patients receiving chemotherapy. Journal of The Royal Thai Army Nurses. 2022;23:361–70.
Burns N, Grove S. The practice of nursing research: Appraisal, synthesis and generation of evidence. 6th ed. Saunders Elsevier: St. Louis.; 2009.
Cronbach, L.J. Essentials of psychological testing. 5th ed. Harper & Row: New York; 1990.
Bursac Z, Gauss CH, Williams DK, Hosmer DW. Purposeful selection of variables in logistic regression. Source Code Biol Med. 2008;3:17.
Regression methods in biostatistics: Linear, logistic, survival, and repeated measures models. In: Regression methods in biostatistics: Linear, logistic, survival, and repeated measures models.: New York, NY, US, Springer Publishing Company. 2005, pp xv, 340–xv, .
Singer P, Blaser AR, Berger MM, Calder PC, Casaer M, Hiesmayr M, et al. ESPEN practical and partially revised guideline: Clinical nutrition in the intensive care unit. Clinical Nutrition. 2023;42:1671–89.
Silva-García J, García-Grimaldo A, Rodríguez-Moguel NC, Gómez-Rodriguez AL, Rios-Ayala MA, Hernández-Cardenas CM, et al. Malnutrition is associated with clinical outcomes in mechanically ventilated patients with pneumonia and other lung manifestations: A retrospective cohort study. Nutr Clin Pract. 2025;40:870–9.
Shah S, Ullah K, Bibi A, Ullah L, Khan BA, Ullah S, et al. Prevalence and severity of malnutrition among intensive care patients in a government tertiary care hospital in Swat: malnutrition in intensive care unit patients. NURSEARCHER (Journal of Nursing & Midwifery Sciences). 2025;5:55–60.
Compher C, Higashiguchi T, Yu J, Jensen GL. Does low body mass index predict the hospital mortality of adult western or asian patients? JPEN J Parenter Enteral Nutr. 2018;42:467–72.
Wang S, He Y, Yi J, Sha L. Risk factors for enteral feeding intolerance in critically ill patients: an updated systematic review and meta-analysis. BMC Gastroenterol. 2025;25:233.
Menchamo M, Debebe Z, Abebe Z. Nutritional status and clinical outcomes of adult intensive care unit (ICU) patients -- a systematic review and Meta-analysis; 2025.
Pontzer H, Yamada Y, Sagayama H, Ainslie PN, Andersen LF, Anderson LJ, et al. Daily energy expenditure through the human life course. Science. 2021;373:808–12.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 The Thai Society of Critical Care Medicine

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.




