Effects of proton pump inhibitors for stress ulcer prophylaxis in critically ill patients: A randomized control trial
PPIs for stress ulcer prophylaxis
DOI:
https://doi.org/10.54205/ccc.v34.278040Keywords:
Stress ulcer prophylaxis, Critically ill patient, Hospital-acquired pneumoniaAbstract
Background: Critically ill patients are prone to gastrointestinal bleeding, leading to hemodynamic instability, transfusions, and prolonged hospitalization. Stress ulcer prophylaxis with proton pump inhibitors is commonly used in intensive care, but their benefit is uncertain and may increase hospital-acquired pneumonia risk. This study aimed to evaluate the efficacy and safety of proton pump inhibitors (PPIs) for stress ulcer prophylaxis, focusing on the occurrence of gastrointestinal bleeding and pneumonia.
Method: An open label, randomized controlled trial was conducted at Chiangrai Prachanukroh Hospital between January and October 2022. Critically ill patients were randomly assigned to receive a once-daily dose of omeprazole 40 mg intravenously or without prophylaxis; all received enteral nutrition. The primary outcome was the rate of gastrointestinal bleeding at 30 days, and hospital-acquired pneumonia was a safety outcome.
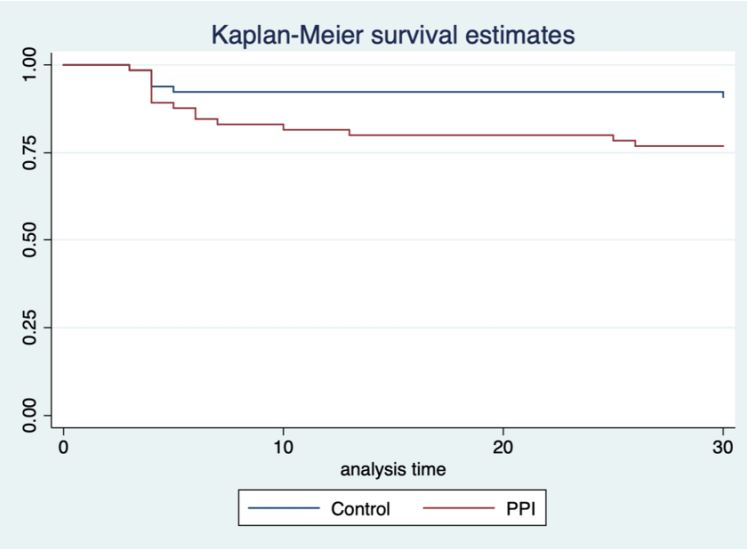
Results: One hundred thirty patients were enrolled (65 per group). Baseline characteristics, disease severity, laboratory values, and feeding parameters were comparable between groups. The duration of mechanical ventilation was longer in the PPI group, and all patients received enteral nutrition with similar feeding profiles. Gastrointestinal bleeding occurred in 6.15% of patients in the proton pump inhibitor group and 3.08% of controls, with no statistically significant difference. Hospital-acquired pneumonia occurred more frequently in the PPI group than in the control group (23.08% vs. 9.23%) in the crude analysis; however, PPI use was not independently associated with hospital-acquired pneumonia after multivariate adjustment. Mortality was higher in the PPI group (9.23% vs. 1.54%), but the difference was not statistically significant.
Conclusions: Critically ill patients on PPIs have comparable rates of gastrointestinal bleeding. Although the incidence of hospital-acquired pneumonia is higher in the PPI group, the multivariable analysis shows no statistically significant difference.
Trial registration: TCTR20260116007
Downloads
References
Cook DJ, Griffith LE, Walter SD, Guyatt GH, Meade MO, Heyland DK, et al. The attributable mortality and length of intensive care unit stay of clinically important gastrointestinal bleeding in critically ill patients. Critical Care. 2001;5(6):368-75.
Krag M, Perner A, Wetterslev J, Wise MP, Borthwick M, Bendel S, et al. Prevalence and outcome of gastrointestinal bleeding and use of acid suppressants in acutely ill adult intensive care patients. Intensive Care Medicine. 2015;41(5):833-45.
Alhazzani W, Guyatt G, Alshahrani M, Deane AM, Marshall JC, Hall R, et al. Withholding pantoprazole for stress ulcer prophylaxis in critically ill patients: a pilot randomized clinical trial and meta-analysis. Crit Care Med. 2017;45(7):1121–29.
El-Kersh K, Jalil B, McClave SA, Cavallazzi R, Guardiola J, Guilkey K, et al. Enteral nutrition as stress ulcer prophylaxis in critically ill patients: a randomized controlled exploratory study. J Crit Care. 2017(1);43:108–13.
Selvanderan SP, Summers MJ, Finnis ME, Plummer MP, Ali Abdelhamid Y, Anderson MB, et al. Pantoprazole or placebo for stress ulcer prophylaxis (POP-UP): randomized double-blind exploratory study. Crit Care Med. 2016;44(10):1842–50.
Lin CC, Hsu YL, Chung CS, Lee TH. Stress ulcer prophylaxis in patients being weaned from the ventilator in a respiratory care center: a randomized control trial. J Formos Med Assoc. 2016;115(1):19–24.
Cook D, Guyatt G. Prophylaxis against Upper Gastrointestinal Bleeding in Hospitalized Patients. New England Journal of Medicine. 2018;378(26):2506-16.
MacLaren R, Reynolds PM, Allen RR. Histamine-2 Receptor Antagonists vs Proton Pump Inhibitors on Gastrointestinal Tract Hemorrhage and Infectious Complications in the Intensive Care Unit. JAMA Internal Medicine. 2014;174(4):564-74.
Krag M, Perner A, Wetterslev J, Wise MP, Hylander M. Stress ulcer prophylaxis versus placebo or no prophylaxis in critically ill patients: a systematic review of randomized clinical trials with meta-analysis and trial sequential analysis. Intensive Care Med. 2014;40(1):11-22.
Krag M, Marker S, Perner A, Wetterslev J, Wise MP, Schefold JC, et al. Pantoprazole in Patients at Risk for Gastrointestinal Bleeding in the ICU. New England Journal of Medicine. 2018;379(23):2199-208.
Herzig SJ, Doughty C, Lahoti S, Marchina S, Sanan N, Feng W, et al. Acid-Suppressive Medication Use in Acute Stroke and Hospital-Acquired Pneumonia. Annals of Neurology. 2014;76(5):712-718.
Bateman BT, Bykov K, Choudhry NK, Schneeweiss S, Gagne JJ, Polinski JM, et al. Type of stress ulcer prophylaxis and risk of nosocomial pneumonia in cardiac surgical patients: cohort study. BMJ. 2013;347:f5416.
El-Kersh K, Jalil B, McClave SA, Cavallazzi R, Guardiola J, Guilkey K, et al. Enteral nutrition as stress ulcer prophylaxis in critically ill patients: A randomized controlled exploratory study. Journal of Critical Care. 2018(1);43:108-113.
Thorens J, Froehlich F, Schwizer W, Saraga E, Bille J, Gyr K, et al. Bacterial overgrowth during treatment with omeprazole compared with cimetidine: a prospective randomized double-blind study. Gut. 1996;39(1):54-9.
Zedtwitz-Liebenstein K, Wenisch C, Patruta S, Parschalk B, Daxböck F, Graninger W. Omeprazole treatment diminishes intra- and extracellular neutrophil reactive oxygen production and bacterial activity. Critical Care Medicine. 2002;30(5):1118-22.
Huang HB, Jiang W, Wang CY, Qin HY, Du B. Stress ulcer prophylaxis in intensive care unit patients receiving nutrition: a systematic review and meta-analysis. Crit Care. 2018;22(1):20.
Papazian L, Klompas M, Luyt CE. Ventilator-associated pneumonia in adults: a narrative review. Intensive Care Med. 2020;46(5):888-906.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 The Thai Society of Critical Care Medicine

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.




