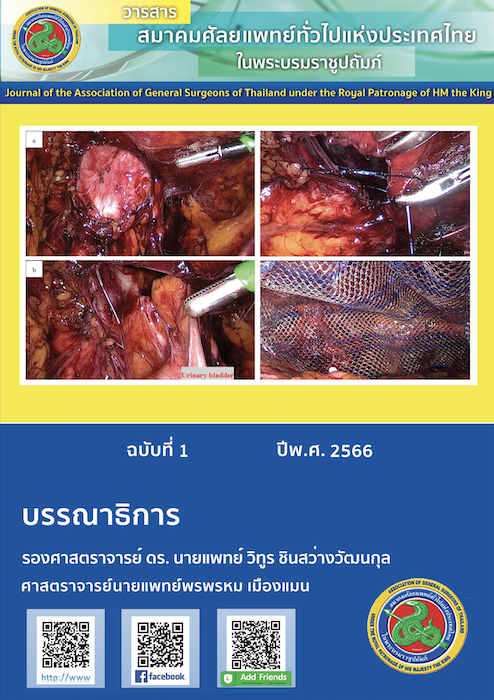
Massive inguinoscrotal hernia successfully repaired with laparoscopic total extraperitoneal hernia repair (T.E.P.): case report
Abstract
Inguinal hernia is a common surgical condition. It accounts for 75% of all abdominal wall hernias with a life-time risk of 27-43% in men and 3-6% in women. Even though extensive inguinoscrotal herniation of bladder is extremely rare, the bladder may be involved in up to 4% of all inguinal hernia cases. Majority of the patients presented with classical hernia symptoms with seldom complaints of urinary symptoms such as voiding related scrotal swelling, two-stage micturition (a first spontaneous voiding followed by a second requiring manual compression of the inguinoscrotal region), urinary tract infections, or irritative lower urinary tract symptoms (LUTS) such as urgency, frequency, and nocturia. Since the presentation is near identical to classic inguinal hernia, most of the cases were diagnosed intraoperatively and increasing the risk of accidental bladder injury. Only 10% of this condition can be diagnosed preoperatively. Surgical repair of hernia is the mainstay of the treatment which open techniques are the majority. We report the successfully laparoscopic total extraperitoneal hernia repair (T.E.P) for an extensive inguinoscrotal bladder hernia.
References
The HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018;22(1):1–165
Balamaddaiah G, et al. Prevalence and risk factors of inguinal hernia: a study in a semi-urban area in Rayalaseema, Andhra Pradesh, India. Int Surg J. 2016;3(3):1310-1313
Branchu B, Renard Y, et al. Diagnosis and treatment of inguinal hernia of the bladder: a systematic review of the past 10 years. Turk J Urol. 2018;44(5):384–388.
Levine B. Scrotal cystosele. J Am Med Assoc. 1951;147:1439–1441.
Kim KH, Kim MU, Jeong WJ. Incidentally detected inguinoscrotal bladder hernia. Korean J Urol. 2011;52:71–73.
Felipe WL, et al. Incidentally detected massive scrotal cystocele. Radiol Bras. 2018; 51(2):129–130.
Karanikas M, Kofina K, et al. Urinary bladder-containing incarcerated inguinoscrotal hernia: a case report. J. Surg. Case Rep., 2020;(11): rjaa092.
Hamidi Madani A, Mohammadi Nikouei H, et al. Scrotal herniation of bladder: a case report. Iran J Med Sci. 2013;38(1):62-4.
Hao-Han C, Shen-Chen W. Extraperitoneal laparoscopic repair of huge inguinoscrotal bladder hernia: A case report and literature review. Urology Case Reports.2021;(38):101735
Schmedt CG, Sauerland S, Bittner R. Comparison of endoscopic procedures vs Lichtenstein and other open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Surg Endosc. 2005;19(2):188-99.
Lyu Y, Cheng Y, et al. Comparison of endoscopic surgery and Lichtenstein repair for treatment of inguinal hernias. Medicine (Baltimore). 2020;99(6):e19134.
Shinichiro H, et al. Clinical characteristics of inguinal bladder hernias and total extraperitoneal repair. Asian J Endosc Surg. 2020;1–7.
Lee JY, et al. Laparoscopic Repair of Large Bladder Herniation Presenting as an Inguinal Hernia. Korean J Urol. 2013;54(2):139–142.
Yokoi R, Yamada S, Hatanaka Y, Kato H. Laparoscopic repair of femoral hernia involving the bladder with coexisting indirect inguinal hernia in a young man: a case report. Surg Case Rep. 2021;7(1):252.
Chow PM, Su YR, Chen YS. A rare complication from total extraperitoneal (TEP) laparoscopic inguinal hernia repair: bladder rupture associated with a balloon dissector. Case Reports Hernia. 2013;17(6):797-9
Ng AY, Lin J, Ching SS, Lee J, Wong ASY. Does primary closure of direct inguinal hernia defect during laparoscopic mesh repair reduce the risk of early recurrence? Hernia. 2020;24(5):1093-1098.
Usmani F, Wijerathne S, Malik S, Yeo C, Rao J, Lomanto D. Effect of direct defect closure during laparoscopic inguinal hernia repair ("TEP/TAPP plus" technique) on post-operative outcomes. Hernia. 2020;24(1):167-171.
Zhu Y, Liu M, Li J, Wang M. Closure of Direct Inguinal Hernia Defect in Laparoscopic Hernioplasty to Prevent Seroma Formation: A Prospective Double-blind Randomized Controlled Trial. Surg Laparosc Endosc Percutan Tech. 2019;29(1):18-21.