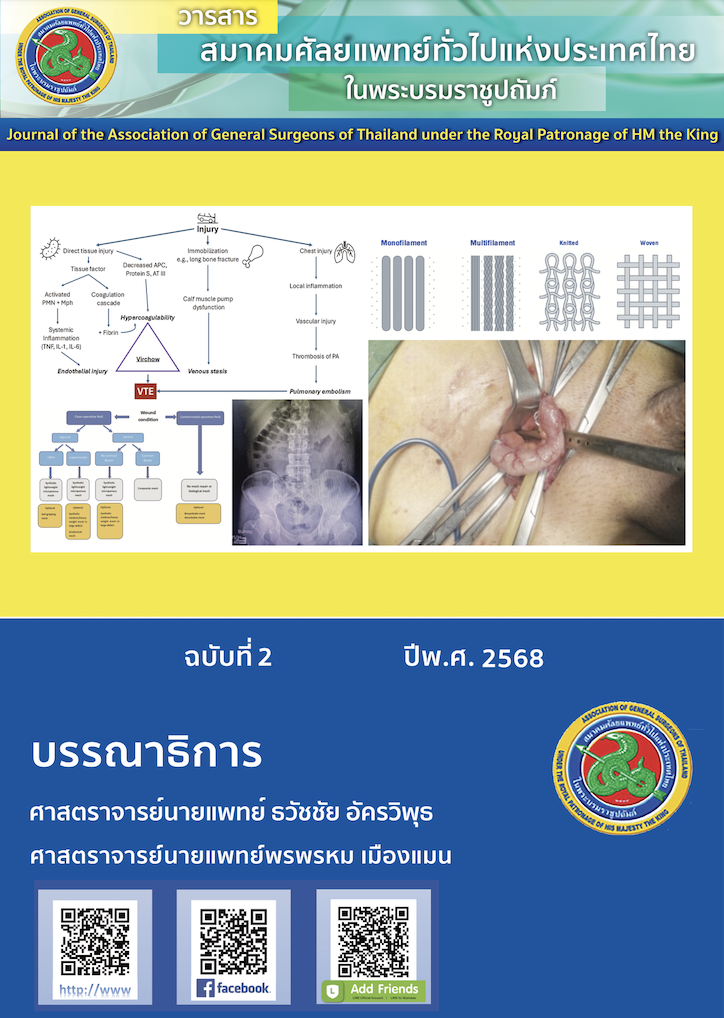
Hernia Mesh: Understanding the Properties and Selection of Materials for Hernia Repair
Keywords:
Hernia, Mesh, Mesh selectionAbstract
Hernia repair remains one of the most common procedures in general surgery, and mesh reinforcement has become the standard of care to reduce recurrence rates. A wide variety of mesh types and materials have been developed to address specific surgical needs and patient risk factors. This review provides an updated overview of synthetic and biological meshes, highlighting their properties, advantages, and limitations. Non-absorbable synthetic meshes, such as polypropylene and polyester, offer durable strength but may induce significant inflammatory responses, while ePTFE minimises adhesions at the cost of poor tissue integration. Absorbable synthetic meshes provide temporary support in contaminated fields but risk early degradation. Biological meshes derived from human or animal tissue offer high biocompatibility and suitability for infected settings but are expensive and mechanically weaker. Composite meshes combine different materials to balance tissue integration with anti-adhesive barriers for safe intraperitoneal use. Key factors in mesh selection include placement location (extra- vs intra-peritoneal), wound condition (clean vs contaminated), desired properties (lightweight, macroporous, monofilament structure), and appropriate sizing with sufficient overlap to prevent recurrence. Understanding these considerations is essential for optimising patient outcomes, reducing complications such as chronic pain or infection, and ensuring long-term hernia repair durability.
References
Köckerling F, Simons MP. Current Concepts of Inguinal Hernia Repair. Visc Med. 2018;34(2):145-50.
Grebić D, Havidić K. Historical review of surgical technique for operative treatment of inguinal hernia. Acta Med Hist Adriat. 2025;22(2):251-9.
Saiding Q, Chen Y, Wang J, Pereira CL, Sarmento B, Cui W, et al. Abdominal wall hernia repair: from prosthetic meshes to smart materials. Mater Today Bio. 2023;21:100691.
Salgaonkar H, Lomanto D. Mesh technology. Ann Laparosc Endosc Surg. 2017;2.
Amid PK. Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia. 2004;8(1):1-7.
International guidelines for groin hernia management. Hernia. 2018;22(1):1-165.
Cobb WS, Burns JM, Peindl RD, Carbonell AM, Matthews BD, Kercher KW, et al. Textile analysis of heavy weight, mid-weight, and light weight polypropylene mesh in a porcine ventral hernia model. J Surg Res. 2006;136(1):1-7.
Klinge U, Klosterhalfen B, Conze J, Limberg W, Obolenski B, Öttinger A, et al. Modified mesh for hernia repair that is adapted to the physiology of the abdominal wall. Eur J Surg. 1998;164(12):951-60.
Alfieri S, Amid PK, Campanelli G, Izard G, Kehlet H, Wijsmuller AR, et al. International guidelines for prevention and management of post-operative chronic pain following inguinal hernia surgery. Hernia. 2011;15(3):239-49.
LeBlanc KA, Elieson MJ, Corder JM, 3rd. Enterotomy and mortality rates of laparoscopic incisional and ventral hernia repair: a review of the literature. JSLS. 2007;11(4):408-14.
Wu JF, Chen J, Hong F. Intestinal erosion caused by meshoma displacement: A case report. World J Gastrointest Surg. 2023;15(1):114-20.
Deeken CR, Lake SP. Mechanical properties of the abdominal wall and biomaterials utilized for hernia repair. J Mech Behav Biomed Mater. 2017;74:411-27.
Campanelli G, Catena F, Ansaloni L. Prosthetic abdominal wall hernia repair in emergency surgery: from polypropylene to biological meshes. World J Emerg Surg. 2008;3:33.
Sanders DL, Kingsnorth AN. Prosthetic mesh materials used in hernia surgery. Expert Rev Med Devices. 2012;9(2):159-79.
Klinge U, Klosterhalfen B. Mesh implants for hernia repair: an update. Expert Rev Med Devices. 2018;15(10):735-46.
Köckerling F, Sheen AJ, Berrevoet F, Campanelli G, Cuccurullo D, Fortelny R, et al. The reality of general surgery training and increased complexity of abdominal wall hernia surgery. Hernia. 2019;23(6):1081-91.
Gönüllü D, Köksoy FN. The Prosthetic Materials in Hernia Repair. J Acad Res Med. 2015;5(1):1-5.
Zhu L-M, Schuster P, Klinge U. Mesh implants: An overview of crucial mesh parameters. World J Gastrointerest Surg. 2015;7(10):226-236.
Brown CN, Finch JG. Which mesh for hernia repair? Ann R Coll Surg Engl. 2010;92(4):272-8.
Rodríguez M, Gómez-Gil V, Pérez-Köhler B, Pascual G, Bellón JM. Polymer Hernia Repair Materials: Adapting to Patient Needs and Surgical Techniques. Materials (Basel). 2021;14(11).
Trippoli S, Caccese E, Tulli G, Ipponi P, Marinai C, Messori A. Biological meshes for abdominal hernia: Lack of evidence-based recommendations for clinical use. Int J Surg. 2018;52:278-84.
Novitsky YW. Biology of biological meshes used in hernia repair. Surg Clin North Am. 2013;93(5):1211-5.
Sanders DL, Pawlak MM, Simons MP, Aufenacker T, Balla A, Berger C, et al. Midline incisional hernia guidelines: the European Hernia Society. Br J Surg. 2023;110(12):1732-68.
Henriksen N, Montgomery A, Kaufmann R, Berrevoet F, East B, Fischer J, et al. Guidelines for treatment of umbilical and epigastric hernias from the European Hernia Society and Americas Hernia Society. Br J Surg. 2020;107(3):171-90.
Köckerling F, Alam NN, Antoniou SA, Daniels IR, Famiglietti F, Fortelny RH, et al. What is the evidence for the use of biologic or biosynthetic meshes in abdominal wall reconstruction? Hernia. 2018;22(2):249-69.
Al-Bustami IS, Clements T, Ferguson D, Harmouch A, Olavarria OA, Holihan JL. Biosynthetic mesh in hernia repair: A systematic review and meta-analysis. Int J Abdom Wall Hernima Surg. 2024;7(2):55-66.
Bilsel Y, Abci I. The search for ideal hernia repair; mesh materials and types. Int J Surg. 2012;10(6):317-21.
Wang See C, Kim T, Zhu D. Hernia Mesh and Hernia Repair: A Review. Eng Regen. 2020;1:19-33.
Sanbhal N, Miao L, Xu R, Khatri A, Wang L. Physical structure and mechanical properties of knitted hernia mesh materials: A review. J Ind Text. 2018;48(1):333-60.
Deveci CD, Öberg S, Rosenberg J. Definition of Mesh Weight and Pore Size in Groin Hernia Repair: A Systematic Scoping Review of Randomised Controlled Trials. J Abdom Wall Surg. 2023;2:11179.
Krpata DM, Petro CC, Prabhu AS, Tastaldi L, Zolin S, Fafaj A, et al. Effect of Hernia Mesh Weights on Postoperative Patient-Related and Clinical Outcomes After Open Ventral Hernia Repair: A Randomized Clinical Trial. JAMA Surg. 2021;156(12):1085-92.
Özant A, Arslan K. Synthetic Meshes in Hernia Surgery. Cyprus J Med Sci. 2023.
Pott PP, Schwarz ML, Gundling R, Nowak K, Hohenberger P, Roessner ED. Mechanical properties of mesh materials used for hernia repair and soft tissue augmentation. PLoS ONE. 2012;7(10):e46978.
Klinge U, Klosterhalfen B, Müller M, Ottinger AP, Schumpelick V. Shrinking of polypropylene mesh in vivo: an experimental study in dogs. Eur J Surg. 1998;164(12):965-9.
Yewande A, Chamilka M, Michael S, Marielle M, Parag B. Mesh and plane selection: a summary of options and outcomes. Plast Aesthet Res. 2020;7:5.
Keric N, Campbell A. Meshing around: high-risk hernias and infected mesh. Trauma Surg Acute Care Open. 2024;9(Suppl 2):e001379.
Ellis R, Miller BT. Mesh Selection in Abdominal Wall Reconstruction: An Update on Biomaterials. Surg Clin North Am. 2023;103(5):1019-28.
Tansawet A, Rodsakan T, Kasetsermwiriya W, Lerdsirisopon S, Techapongsatorn S. The Myopectineal Orifice: A Study of Thai Cadavers. Front Surg. 2022;9:843344.
Howard R, Ehlers A, O'Neill S, Shao J, Englesbe M, Dimick JB, et al. Mesh overlap for ventral hernia repair in current practice. Surg Endosc. 2023;37(12):9476-82.