A Case Report of Cellulitis Caused by Leclercia adecarboxylata in a Thai Boy: A Common Infection From a Rare Pathogen
DOI:
https://doi.org/10.33165/rmj.2024.47.3.268046Keywords:
Leclercia adecarboxylata, Soft tissue infection, Puncture woundAbstract
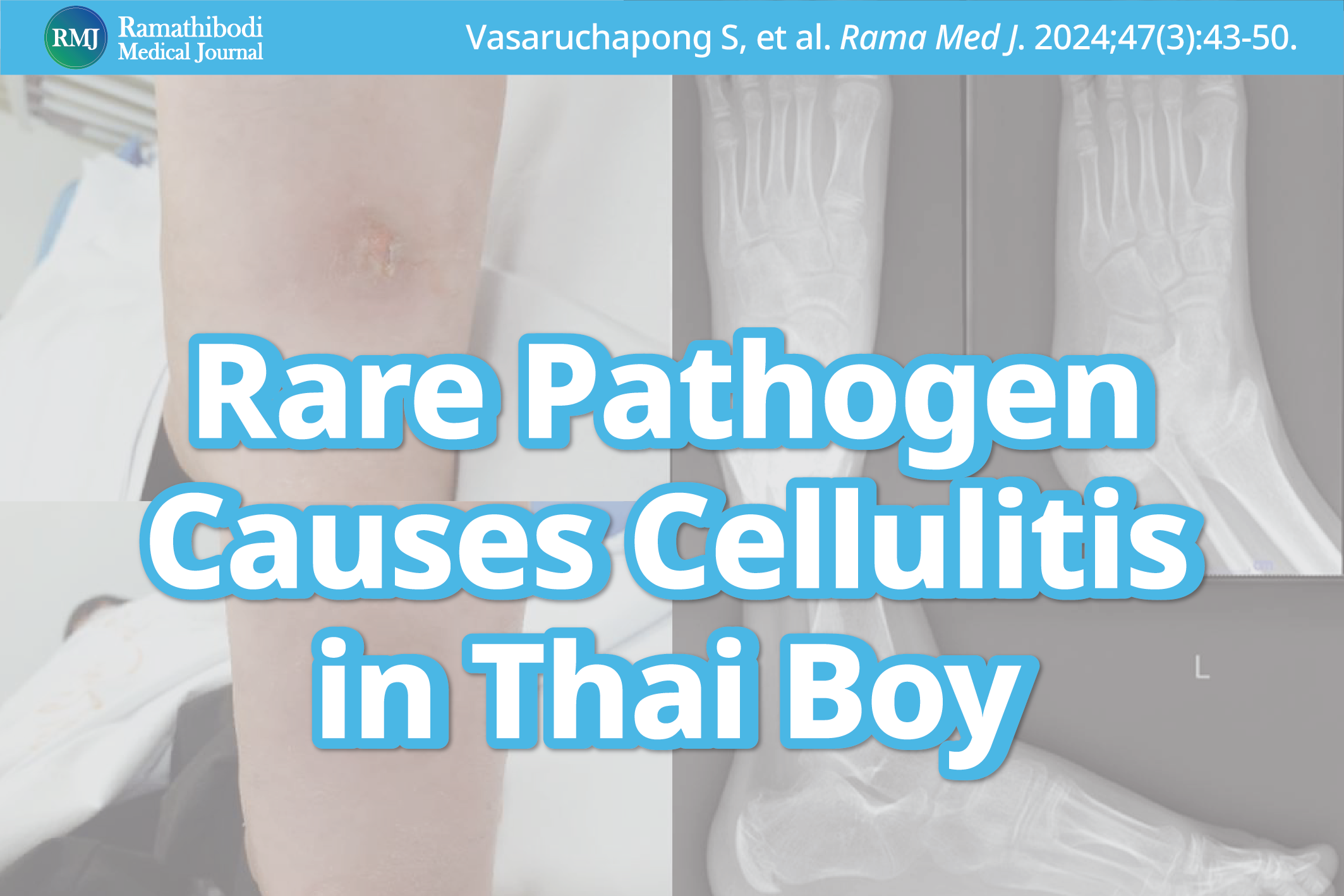
Leclercia adecarboxylata is a gram-negative bacillus that rarely causes infections in children, especially in Thailand. We report a case of a boy with a wound infection and cellulitis after a punctate injury caused by L. adecarboxylata. A previously healthy 12-year-old boy presented with a 2-month history of infected wound and cellulitis on his left sole after a punctate injury in the garden. He experienced recurrent swelling and purulent discharge despite an incision and drainage and a full course of appropriate antibiotics. Plain films of his left foot showed no radiopaque foreign body or evidence of osteomyelitis. L. adecarboxylata was isolated from the wound tissue culture. Incision and drainage followed by a 2-week course of oral amoxicillin/clavulanic acid was prescribed which resulted in a complete resolution of the lesion. This case emphasizes the significance of identifying L. adecarboxylata as a possible cause of soft tissue infections in Thai children, especially those with a history of puncture wounds. Unusual pathogens should be considered when standard treatments fail to eliminate the infection.
References
Leclerc H. Biochemical study of pigmented Enterobacteriaceae. Ann Inst Pasteur (Paris). 1962;102:726-741.
Tamura K, Sakazaki R, Kosako Y, Yoshizaki E. Leclercia adecarboxylata gen. nov., comb. nov., formerly known as Escherichia adecarboxylata. Curr Microbiol. 1986;13:179-184. doi:10.1007/BF01568943
Spiegelhauer MR, Andersen PF, Frandsen TH, Nordestgaard RLM, Andersen LP. Leclercia adecarboxylata: a case report and literature review of 74 cases demonstrating its pathogenicity in immunocompromised patients. Infect Dis (Lond). 2019;51(3):179-188. doi:10.1080/23744235.2018.1536830
Zayet S, Lang S, Garnier P, et al. Leclercia adecarboxylata as emerging pathogen in human infections: clinical features and antimicrobial susceptibility testing. Pathogens. 2021;10(11):1399. doi:10.3390/pathogens10111399
Keyes J, Johnson EP, Epelman M, Cadilla A, Ali S. Leclercia adecarboxylata: an emerging pathogen among pediatric infections. Cureus. 2020;12(5):e8049. doi:10.7759/cureus.8049
Stock I, Burak S, Wiedemann B. Natural antimicrobial susceptibility patterns and biochemical profiles of Leclercia adecarboxylata strains. Clin Microbiol Infect. 2004;10(8):724-733. doi:10.1111/j.1469-0691.2004.00892.x
Sarma PM, Bhattacharya D, Krishnan S, Lal B. Degradation of polycyclic aromatic hydrocarbons by a newly discovered enteric bacterium, Leclercia adecarboxylata. Appl Environ Microbiol. 2004;70(5):3163-3166. doi:10.1128/AEM.70.5.3163-3166.2004
Chotelersak K, Thamacharoensuk T, Tanasupawat S, Nantavisai K, Taweechotipatr M, Puttikamonkul S. Preliminary studies of lactic acid bacteria isolated from feces of Thai newborns. J Med Assoc Thai. 2016;99 Suppl 8:S90-S98.
De Mauri A, Chiarinotti D, Andreoni S, Molinari GL, Conti N, De Leo M. Leclercia adecarboxylata and catheter-related bacteraemia: review of the literature and outcome with regard to catheters and patients. J Med Microbiol. 2013;62(Pt 10):1620-1623. doi:10.1099/jmm.0.059535-0
Mayfield CK, Haglin JM, Konda SR, Tejwani NC, Egol KA. Post-operative orthopedic infection with monomicrobial Leclercia adecarboxylata: a case report and review of the literature. JBJS Case Connect. 2019;9(3):e0297. doi:10.2106/JBJS.CC.18.00297
Fattal O, Deville JG. Leclercia adecarboxylata peritonitis in a child receiving chronic peritoneal dialysis. Pediatr Nephrol. 2000;15(3-4):186-187. doi:10.1007/s004670000436
Longhurst CA, West DC. Isolation of Leclercia adecarboxylata from an infant with acute lymphoblastic leukemia. Clin Infect Dis. 2001;32(11):1659. doi:10.1086/320539
Myers KA, Jeffery RM, Lodha A. Late-onset Leclercia adecarboxylata bacteraemia in a premature infant in the NICU. Acta Paediatr. 2012;101(1):e37-e39. doi:10.1111/j.1651-2227.2011.02431.x
Shah A, Nguyen J, Sullivan LM, Chikwava KR, Yan AC, Treat JR. Leclercia adecarboxylata cellulitis in a child with acute lymphoblastic leukemia. Pediatr Dermatol. 2011;28(2):162-164. doi:10.1111/j.1525-1470.2011.01348.x
Sethi K, Barker EM, Metlay LA, Caserta MT, Daugherty LE. Leclercia adecarboxylata sepsis and cerebral herniation. J Pediatric Infect Dis Soc. 2014;3(1):e1-e3. doi:10.1093/jpids/pis131
Nelson MU, Maksimova Y, Schulz V, Bizzarro MJ, Gallagher PG. Late-onset Leclercia adecarboxylata sepsis in a premature neonate. J Perinatol. 2013;33(9):740-742. doi:10.1038/jp.2013.34
Hurley EH, Cohen E, Katarincic JA, Ohnmacht RK. Leclercia adecarboxylata infection in an immunocompetent child. R I Med J. 2015;98(9):41-44.
Grantham WJ, Funk SS, Schoenecker JG. Leclercia adecarboxylata musculoskeletal infection in an immune competent pediatric patient: an emerging pathogen? Case Rep Orthop. 2015;2015:160473. doi:10.1155/2015/160473
Capretta N, Pearl J, Lawrence J, Gagliardo C. 716: An immunocompetent pediatric patient with rare Leclercia adecarboxylata wound infection. Critical Care Medicine. 2018;46(1):344. doi:10.1097/01.ccm.0000528730.92625.17
Broderick A, Lowe E, Xiao A, Ross R, Miller R. Leclercia adecarboxylata folliculitis in a healthy swimmer-an emerging aquatic pathogen? JAAD Case Rep. 2019;5(8):706-708. doi:10.1016/j.jdcr.2019.06.007
Sánchez-Códez M, Lubián-Gutiérrez M, Blanca-García JA, Pérez Aragón C. Leclercia adecarboxylata and Raoultella ornithinolytica catheter-related infection in a child with mitochondrial disease. Arch Argent Pediatr. 2019;117(2):e147-e149. doi:10.5546/aap.2019.e147
Hassan I, Gupta P, Ray P, Tiewsoh K. Leclercia adecarboxylata causing spontaneous bacterial peritonitis in a child with nephrotic syndrome: a case report and review of literature. J Lab Physicians. 2020;12(3):222-224. doi:10.1055/s-0040-1721162
Courtois MF, Hernando A, Jokanovich MV, Paruelo F, Plata F. Catheter colonization by Leclercia adecarboxylata: a pediatric case report. Arch Argent Pediatr. 2020;118(4):e418-e420. doi:10.5546/aap.2020.e418
Arasu R, Ewe YH, Sundaram A, et al. Two cases of Leclercia adecarboxylata septic arthritis in immunocompetent paediatric patients. Access Microbiol. 2022; 4(2):000325. doi:10.1099/acmi.0.000325
Aarab A, Saddari A, Noussaiba B, et al. Leclercia adecarboxylata invasive infection in a patient with Hirschsprung disease: a case report. Ann Med Surg (Lond). 2021;71:102927. doi:10.1016/j.amsu.2021.102927
Bronte Anaut M, Arredondo Montero J, García Abellás P, de Uribe Viloria M, Regojo Zapata RM. Fulminant sepsis caused by Leclercia adecarboxylata in a premature neonate: case report and review of the literature. Pediatr Infect Dis J. 2022;41(5):e220-e222. doi:10.1097/INF.0000000000003472
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 by the Authors. Licensee Ramathibodi Medical Journal.

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
















