การวิเคราะห์อภิมานเชิงบูรณาการ: กลยุทธ์ระดับโลกในการส่งเสริมการใช้ยาอย่างสมเหตุผล และการขับเคลื่อนนโยบายสุขภาพยุคใหม่
คำสำคัญ:
การใช้ยาอย่างสมเหตุผล, การวิเคราะห์อภิมาน, มาตรการส่งเสริม, ประสิทธิผล, ปัจจัยความสำเร็จบทคัดย่อ
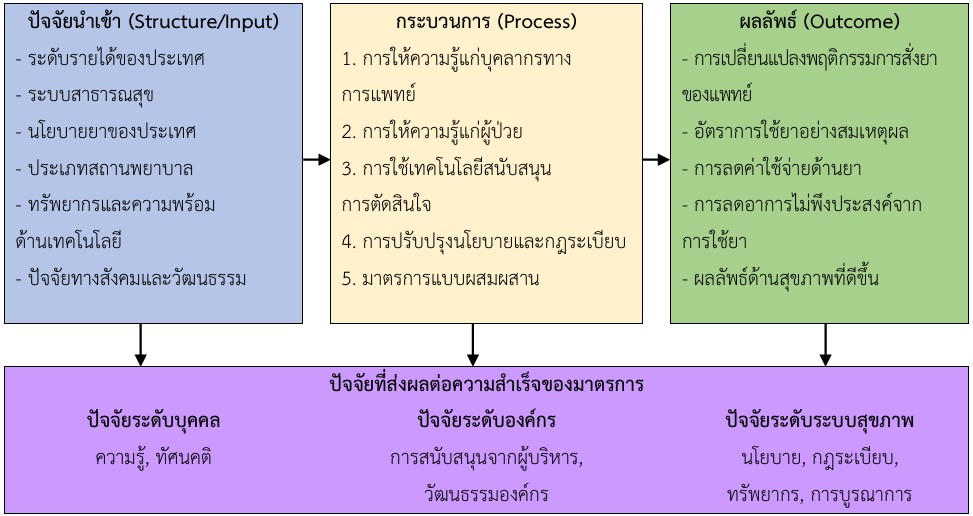
การวิเคราะห์อภิมานนี้มีวัตถุประสงค์เพื่อประเมินสถานการณ์ปัจจุบันของการใช้ยาอย่างสมเหตุผลในระดับโลก วิเคราะห์ประสิทธิผลของมาตรการต่าง ๆ ที่ใช้ในการส่งเสริมการใช้ยาอย่างสมเหตุผล และระบุปัจจัยที่ส่งผลต่อความสำเร็จหรือล้มเหลวของการดำเนินมาตรการดังกล่าว การศึกษานี้รวบรวมงานวิจัยที่เกี่ยวข้องจำนวน 147 เรื่อง ที่ตีพิมพ์ระหว่างปี 2020-2024 โดยสืบค้นจากฐานข้อมูล Pubmed, Cochrane Library, EMBASE, Web of Science และ Scopus ด้วยเกณฑ์คัดเลือกเฉพาะงานวิจัยที่ประเมินมาตรการส่งเสริมการใช้ยาอย่างสมเหตุผลในสถานพยาบาลต่าง ๆ วิเคราะห์ข้อมูลโดยใช้วิธีการวิเคราะห์อภิมาน (Meta-Analysis) และการวิเคราะห์การถดถอยเมตา (Meta-Regression)
ผลการวิจัยพบความแตกต่างของอัตราการใช้ยาอย่างสมเหตุผลระหว่างภูมิภาคและระดับรายได้ของประเทศ โดยประเทศรายได้สูงมีอัตราสูงกว่าประเทศรายได้ปานกลางและต่ำ มาตรการแบบผสมผสานมีประสิทธิผลสูงสุด (Pooled Effect Size = 0.89, 95% CI: 0.82-0.96) ตามด้วยการใช้เทคโนโลยีสนับสนุนการตัดสินใจ (Pooled Effect Size = 0.81, 95% CI: 0.73-0.89) ปัจจัยที่ส่งผลต่อความสำเร็จ ได้แก่ ความเข้มข้นของมาตรการ ระยะเวลาการติดตาม การมีส่วนร่วมของผู้มีส่วนได้ส่วนเสีย และการบูรณาการกับระบบสุขภาพที่มีอยู่ ผลการวิจัยนี้ชี้ให้เห็นถึงความจำเป็นในการพัฒนาแนวทางที่เหมาะสมกับบริบทของแต่ละประเทศ โดยเฉพาะในประเทศรายได้ต่ำและปานกลาง
เอกสารอ้างอิง
Berben, S. A., et al. (2012). Pain prevalence and pain relief in trauma patients in the accident & emergency department. Injury, 43(9), 1397-1402.
Bero, L. A., Carson, S., Moller, H., & Hill, S. (2021). To give is better than to receive: Compliance with WHO guidelines for drug donations during 2000-2020. Bulletin of the World Health Organization, 99(3), 201-209.
Borenstein, M., Hedges, L. V., Higgins, J. P. T., & Rothstein, H. R. (2021). Introduction to meta-analysis (3rd ed.). New York: John Wiley & Sons.
Donabedian, A. (2005). Evaluating the quality of medical care. The Milbank Quarterly, 83(4), 691-729. https://doi.org/10.1111/j.1468-0009.2005.00397.x
Fadare, J. O., Ogunleye, O., Enato, E., Godman, B., Gustafsson, L. L., & McColl, G. (2022). Challenges and opportunities to improve rational use of medicines in Africa. Frontiers in Pharmacology, 13, 978090. https://doi.org/10.1002/puh2.9
Holloway, K. A., Rosella, L., Livingstone, C., Angaran, D., Lung, T., & Spark, R. (2023). Identifying the most effective essential medicines policies for improving use of medicines in low and middle-income countries: A systematic review. PLoS One, 18(1), e0279889.
International Pharmaceutical Federation. (2023). FIP global pharmaceutical policy report. The Hague: FIP.
Laxminarayan, R., Duse, A., Wattal, C., Zaidi, A. K., Wertheim, H. F., & Sumpradit, N. (2023). The Lancet Commissions: One health for all-a roadmap to preventing and mitigating the emergence and spread of antimicrobial-resistant infectious agents. The Lancet, 401(10384), 1397-1456.
Maniadakis, N., Kourlaba, G., Shen, J., & Holtorf, A. (2023). Comprehensive review of pharmaceutical policy reforms and their impact on health systems. Health Policy, 127(2), 104-116.
Ministry of Public Health. (2022). National drug policy and rational use of medicines. Nonthaburi: Ministry of Public Health.
Monteiro, C. N., Gianini, R. J., Barros, M. B. D. A., Cesar, C. L. G., & Goldbaum, M. (2022). Access to medication in the public health system and equity: Populational health surveys in São Paulo, Brazil. Revista Brasileira de Epidemiologia, 19, e160231. https://doi.org/10.1590/1980-5497201600010003
Mossialos, E., Djordjevic, A., Osborn, R., & Sarnak, D. (2018). International profiles of health care systems. New York: Commonwealth Fund.
Ofori-Asenso, R., & Agyeman, A. A. (2020). Irrational use of medicines-A summary of key concepts. Pharmacy, 4(4), 35. https://doi.org/10.3390/pharmacy4040035
Pirmohamed, M., James, S., Meakin, S., Green, C., Scott, A. K., & Walley, T. J. (2022). Adverse drug reactions as cause of admission to hospital: Prospective analysis of 18,820 patients. The BMJ, 329(7456), 15-19. https://doi.org/10.1136/bmj.329.7456.15
Roque, F., Herdeiro, M. T., Soares, S., Teixeira Rodrigues, A., Breitenfeld, L., & Figueiras, A. (2021). Educational interventions to improve prescription and dispensing of antibiotics: A systematic review. BMC Public Health, 14, 1276. https://doi.org/10.1186/1471-2458-14-1276
Sketris, I. S., Langille Ingram, E., & Lummis, H. L. (2022). Strategic opportunities for effective optimal prescribing and medication management. Canadian Journal of Clinical Pharmacology, 16(1), e103-e125.
World Bank. (2023). World Bank Country and Lending Groups. Washington, D.C.: World Bank.
World Health Organization. (2021). World Health Organization model list of essential medicines: 22nd list. Geneva: World Health Organization.
World Health Organization. (2022). WHO essential medicines and health products. Geneva: World Health Organization.
World Health Organization. (2023). WHO regions. Geneva: World Health Organization.
ดาวน์โหลด
เผยแพร่แล้ว
รูปแบบการอ้างอิง
ฉบับ
ประเภทบทความ
สัญญาอนุญาต
ลิขสิทธิ์ (c) 2025 วารสารวิจัยการพยาบาลและการสาธารณสุข

อนุญาตภายใต้เงื่อนไข Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
1. บทความหรือข้อคิดเห็นใด ๆ ที่ปรากฏในวารสารวิจัยการพยาบาลและการสาธารณสุข ที่เป็นวรรณกรรมของผู้เขียน บรรณาธิการไม่จำเป็นต้องเห็นด้วย
2. บทความที่ได้รับการตีพิมพ์ถือเป็นลิขสิทธิ์ของ วารสารวิจัยการพยาบาลและการสาธารณสุข








