The Predictive Factors Associated with Longer Operative Time in Single-Incision Laparoscopic Cholecystectomy
DOI:
https://doi.org/10.33192/Smj.2021.86Keywords:
Laparoscopic cholecystectomy, single-incision laparoscopic cholecystectomy, predictive factors, difficult laparoscopic cholecystectomyAbstract
Objective: The difficult laparoscopic cholecystectomy (LC) is defined as the presence of one of the following
conditions including prolonged operative time, conversion to open cholecystectomy or significant blood loss. At
present, there is no evidence of predictive factors related to longer operative time in single-incision laparoscopic
cholecystectomy (SILC). The aim of this study is to determine predictive factors associated with longer operative
time in SILC procedure.
Materials and Methods: A retrospective study was conducted of patients with benign gallbladder disease who
underwent SILC in Thammasat University Hospital between October 2014 and December 2020. Patients’ records
were reviewed. Primary outcomes were preoperative predictive factors associated with DSLC. Secondary outcomes
were perioperative and 3-month postoperative adverse outcomes.
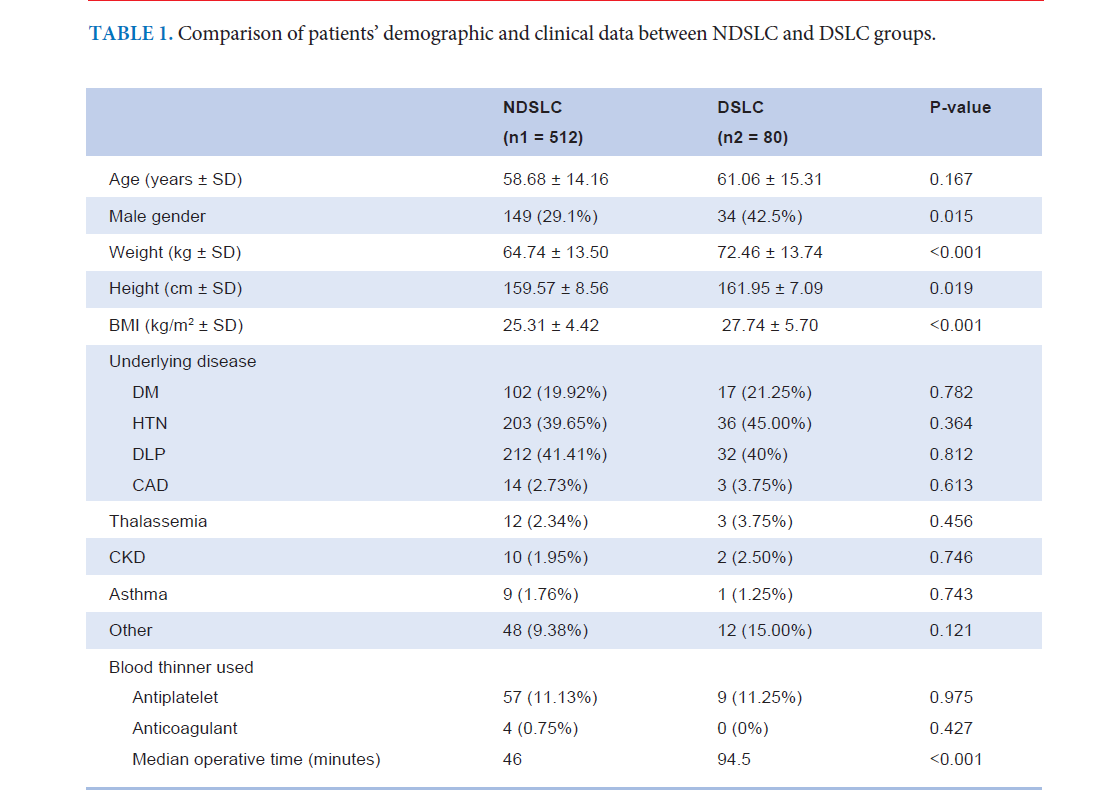
Results: 592 SILC procedures were categorized as 80 DSLC and 512 non-difficult SILC (NDSLC). The median
(interquartile range) of operative time in all SILC procedure is 48 (38, 62) minutes. The threshold of operative time
of difficult SILC was 72 minutes. The multivariate analysis indicated 5 significant predictive factors. Obesity (body
mass index > 25 kg/m2)) and abdominal pain reflected the difficulty of SILC procedures (p = 0.041 and p = 0.009).
Calcified gallbladder showed the highest RR of 14.08 (p = 0.011). Contracted gallbladder and chronic cholecystitis
were also predictive factors with RR of 13.79 and 3.64, respectively (p < 0.001 and p = 0.007).
Conclusion: Obesity, abdominal pain, chronic cholecystitis, contracted gallbladder and calcified gallbladder were
preoperative predictive factors. Surgeons should perform the SILC procedure carefully when predictive factors are
identified.
References
conventional laparoscopic technique for cholecystectomy. World J Surg 2014;38:25-32.
2. Navarra G, Pozza E, Occhionorelli S, Carcoforo P, Donini I. One-wound laparoscopic cholecystectomy. Br J Surg 1997; 84:695.
3. Qu J-W, Xin C, Wang G-Y, Yuan Z-Q, Li K-W. Feasibility and safety of single-incision laparoscopic cholecystectomy versus conventional laparoscopic cholecystectomy in an ambulatory setting. Hepatobiliary & Pancreat Dis Int 2019;18: 273-7.
4. Arezzo A, Passera R, Forcignanò E, Rapetti L, Cirocchi R, Morino M. Single-incision laparoscopic cholecystectomy is responsible for increased adverse events: results of a metaanalysis of randomized controlled trials. Surg Endosc 2018; 32:3739-53.
5. Hoyuela C, Juvany M, Guillaumes S, Ardid J, Trias M, Bachero I, et al. Long-term incisional hernia rate after single-incision laparoscopic cholecystectomy is significantly higher than that after standard three-port laparoscopy: a cohort study. Hernia 2019;23:1205-13.
6. Bourgouin S, Mancini J, Monchal T, Calvary R, Bordes J, Balandraud P. How to predict difficult laparoscopic cholecystectomy? Proposal for a simple preoperative scoring system. Am J Surg 2016;212:873-81.
7. Wakabayashi G, Iwashita Y, Hibi T, Takada T, Strasberg SM, Asbun HJ, et al. Tokyo Guidelines 2018: surgical management of acute cholecystitis: safe steps in laparoscopic cholecystectomy for acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci 2018;25:73-86.
8. Wu T, Luo M, Guo Y, Bi J, Guo Y, Bao S. Role of procalcitonin as a predictor in difficult laparoscopic cholecystectomy for acute cholecystitis case: A retrospective study based on the TG18 criteria. Sci Rep 2019;9:10976.
9. Nidoni R, Udachan TV, Sasnur P, Baloorkar R, Sindgikar V, Narasangi B. Predicting difficult laparoscopic cholecystectomy based on linicoradiological assessment. J Clin Diagn Res 2015;9:PC09-PC12.
10. Chong JU, Lee JH, Yoon YC, Kwon KH, Cho JY, Kim SJ, et al. Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy. Korean J Hepatobiliary Pancreat Surg 2016;20:12-6.
11. Randhawa JS, Pujahari AK. Preoperative prediction of difficult lap chole: a scoring method. Indian J Surg 2009;71:198-201.
12. Hayama S, Ohtaka K, Shoji Y, Ichimura T, Fujita M, Senmaru N, et al. Risk factors for difficult laparoscopic cholecystectomy in acute cholecystitis. JSLS 2016;20:e2016.00065.
13. Stanisic V, Milicevic M, Kocev N, Stanisic B. A prospective cohort study for prediction of difficult laparoscopic cholecystectomy. Ann Med Surg (Lond) 2020;60:728-33.
14. Seehawong U, Sumritpradit P, Krutsri C, Singhatat P, Thampongsa T, P T. Risk factors of difficult laparoscopic cholecystectomy for acute cholecystitis in acute care surgery patients. J Med Assoc Thai 2019;102:56.
15. Poonkeaw T. Predicting Factors of the difficult laparoscopic cholecystectomy in Phatthalung Hospital. Region 11 Medical Journal 2019;30:251-60.
16. Inoue K, Ueno T, Douchi D, Shima K, Goto S, Takahashi M, et al. Risk factors for difficulty of laparoscopic cholecystectomy in grade II acute cholecystitis according to the Tokyo guidelines 2013. BMC Surgery 2017;17:114.
17. Elgammal AS, Elmeligi MH, Koura MMA. Evaluation of preoperative predictive factors for difficult laparoscopic cholecystectomy. Int Surg J 2019;6:3052-6.13
18. Yassein T, Iyoab I, Sallam A, Gomaa M, Sadek A, Osman M, et al. Predicting the risk factors of difficult laparoscopic cholecystectomy step by step. Egypt J Surg 2020;39:515-22.
19. Di Buono G, Romano G, Galia M, Amato G, Maienza E, Vernuccio F, et al. Difficult laparoscopic cholecystectomy and preoperative predictive factors. Sci Rep 2021;11:2559.
20. Saleem A-E-A, Abdallah H. Evaluation of preoperative predictive factors for difficult laparoscopic cholecystectomy in comparison with intraoperative parameters. Egypt J Surg 2018;37:504-11.
21. Ferrarese A, Gentile V, Bindi M, Rivelli M, Cumbo J, Solej M, et al. The learning curve of laparoscopic cholecystectomy in general surgery resident training: old age of the patient may be a risk factor? Open Med (Wars) 2016;11:489-96.
22. Joong Choi C, Roh YH, Kim MC, Choi HJ, Kim YH, Jung GJ. Single-Port Laparoscopic Cholecystectomy for Gall Bladder Polyps. JSLS 2015;19:e2014.00183.
23. Tomioka T, Inoue K, Onizuka S, Ikematsu Y, Kanematsu T. Laparoscopic cholecystectomy is a safe procedure for the Thowprasert et al.
https://he02.tci-thaijo.org/index.php/sirirajmedj/index Volume 73, No.10: 2021 Siriraj Medical Journal 679 Original Article SMJ
treatment of porcelain gallbladder. Endoscopy 1997;29:225.
24. Toouli J. Biliary Dyskinesia. Curr Treat Options Gastroenterol 2002;5:285-91.
25. Chow SC, Shao J, Wang H. Sample size calculations in clinical research, 2 ed. New York: John Wiley & Sons, 2008.
26. Von Elm E, Dg. A, Egger M, Pocock S, Gøtzsche P, Vandenbroucke JP. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 2008;61:344-9.
27. Tiong L, Oh J. Safety and efficacy of a laparoscopic cholecystectomy in the morbid and super obese patients. HPB (Oxford) 2015;
17:600-4.
28. Lyu Y, Cheng Y, Wang B, Zhao S, Chen L. Single-incision versus conventional multiport laparoscopic cholecystectomy: a
current meta-analysis of randomized controlled trials. Surg Endosc 2020;34:4315-29.
29. Bat O. The analysis of 146 patients with difficult laparoscopic cholecystectomy. Int J Clin Exp Med 2015;8:16127-31.
30. Gupta N, Ranjan G, Arora MP, Goswami B, Chaudhary P, Kapur A, et al. Validation of a scoring system to predict difficult
laparoscopic cholecystectomy. International Journal of Surgery 2013;11:1002-6.
31. Lal P, Agarwal PN, Malik VK, Chakravarti AL. A difficult laparoscopic cholecystectomy that requires conversion to open
procedure can be predicted by preoperative ultrasonography. JSLS 2002;6:59-63.
32. Vivek MAKM, Augustine AJ, Rao R. A comprehensive predictive scoring method for difficult laparoscopic cholecystectomy. J
Minim Access Surg 2014;10:62-7.1
Published
How to Cite
Issue
Section
License
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














