Psychometric Properties of the Thai Mental Health Literacy Scale in Sixth-Year Medical Students
DOI:
https://doi.org/10.33192/Smj.2022.13Keywords:
assessment, experience, help-seeking, medical externs, professional, reliability, validityAbstract
Objective: To assess the psychometric properties of the Thai Mental Health Literacy Scale (TMHLS) in sixth-year medical students.
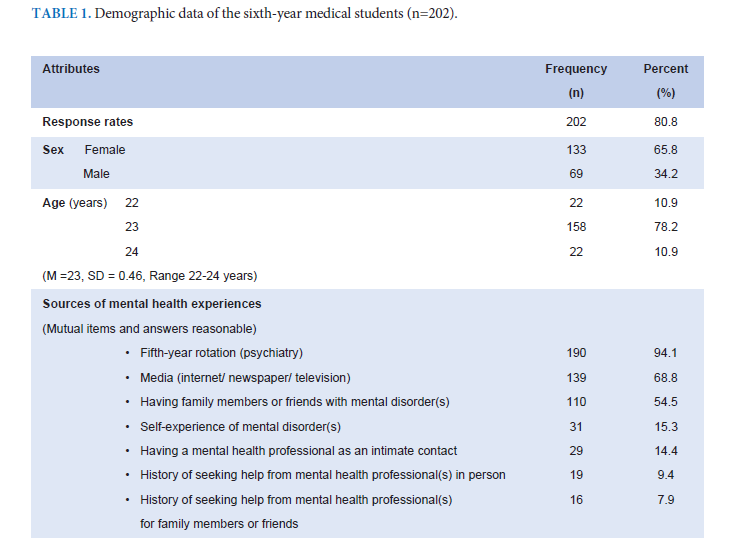
Materials and Methods: By using the purposive sampling method, we enrolled 202 participants in this study. Descriptive statistics were used to analyze demographic data. The index of item-objective congruence (IOC) was used to verify content validity. Exploratory factor analysis (EFA) was performed to establish the construct validity of the TMHLS. The internal consistency was estimated by computing Cronbach’s coefficient alpha.
Results: The TMHLS had good content validity (IOC=.85) and construct validity. The EFA resulted in five factors, which included 32 of the 35 items and accounted for 46.86% of the variance. The factors were the ability to recognize mental disorders; confidentiality of mental health practitioners; skills of mental health information seeking; beliefs about mental illnesses; and attitudes toward patients with mental illness. The reliability coefficient of the TMHLS total test was .851, and reliability coefficient in subdomains were range from .197 to .872. Individuals who had a mental health professional as an intimate contact and individuals who had a history of seeking help from mental health professional(s) in person showed significantly higher mental health literacy than those who did not.
Conclusions: The TMHLS has good psychometric properties. Dynamic knowledge transfer and exchange with a close mental health professional should be applied to promote mental health literacy in medical students.
References
GBD 2017 Disease and Injury Incidence and Prevalence
Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet. 2018;392:1789-1858. doi: https://doi.org/10.1016/S0140-6736(18)32279-7.
Lê-Scherban F, Brenner AB, Schoeni RF. Childhood family wealth and mental health in a national cohort of young adults. SSM - Population Health. 2016;2:798-806. doi: 10.1016/j.ssmph.2016.10.008.
Stallman MH. Psychological distress in university students: a comparison with general population data. Australian Psychologist. 2010;45(4):249-257. doi: https://doi.org/10.1080/00050067.2010.482109.
Smith LC, Shochet IM. The impact of mental health literacy on help-seeking Intentions: results of a pilot study with first year psychology students. International Journal of Mental Health Promotion. 2011;13(2): 14-20.
Gulliver A, Griffiths MK, Helen C. Perceived barriers and facilitators to mental health help-seeking in young people: a systematic review. BMC Psychiatry. 2010;10(113):1-9. doi: https://doi.org/10.1186/1471-244X-10-113.
Hom MA, Stanley IH, Joiner TE. Evaluating factors and
interventions that influence help-seeking and mental health service utilization amongsuicidal individuals: A review of the literature. Clinical Psychology Review. 2015;40:28-39. doi: 10.1016/j.cpr. 2015.05.006.
Rickwood JD, Deane PF, Coralie WJ. When and how do young people seek professional help for mental health problems? MJA. 2007;187(7):35-39. doi: 10.5694/j.1326-5377.2007.tb01334.x.
Wei Y, McGrath P, Hayden J, Kutcher S. Measurement properties of tools measuring mental health knowledge: a systematic review. BMC Psychiatry. 2016;16(297):2-16. doi:10.1186/s12888-016-1012-5.
Marcus M, Westra H. Mental Health Literacy in Canadian
Young Adults: Results of a National Survey. Canadian Journal of Community Mental Health. 2012;1(1-15). doi: https://doi.org/10.7870/cjcmh-2012-0002.
Gentile JP, Roman B. Medical student mental health services: psychiatrists treating medical students. Psychiatry (Edgmont). 2009;6(5):38-45. PMID: 19724734.
Jafari N, Loghmani A, Montazeri A. Mental health of medical students in different levels of training. International Journal of Preventive Medicine. 2012;3(1):S107–S112. PMID: 22826751.
Cheslock PA. Assessing mental health literacy of first- and thirdyear medical students: knowledge and beliefs about mental disorders. Doctoral dissertation. Philadelphia College; 2005.
Marwood MR, Hearn JH. Evaluating mental health literacy in medical students in the United Kingdom. The Journal of Mental Health Training Education and Practice. 2019;14(5):339-347. doi: https://doi.org/10.1108/JMHTEP-01-2019-0001.
Cochran WG.Sampling techniques, 3rd ed. New York: John Wiley & Sons; 1977.
O’Connor M, Casey L. The Mental Health Literacy Scale (MHLS): A new scale-based measure of mental health literacy. Psychiatry Research. 2015;229 (1-2):511-516. doi: 10.1016/j.psychres. 2015.05.064.
SPSS Inc. PASW Statistics for Windows, Version 18.0. Chicago: SPSS Inc; 2009.
Kaiser, H. F. The application of electronic computers to factor analysis. Educational and Psychological Measurement, 1960;20: 141-151.
Floyd, F. J., & Widaman, K. F. . Factor analysis in the development and refinement of clinical assessment instruments. Psychological Assessment, 1995;7(3):286-299.
Kass, R. A. & Tinsley, H. E. A. Factor analysis. Journal of Leisure Research, 1979;11:120-138.
Comrey, A. L. & Lee, H. B. A first course in factor analysis (2nd edition). Hillsdale, NJ: Erlbaum, 1992.
Boomsma A. (1982). The robustness of LISREL against small sample sizes in factor analysis models. In H. Wold & K. Jöreskog (Eds.), Systems under indirect observations (pp. 147-173). New York: Elsevier North-Holland, 1982.
McMillan, J.H. Classroom assessment: principles and practice for effective standards-based instruction (4th ed.). Boston: Pearson, 2007.
Ketumarn P, Sitdhiraksa N, Sittironnarit G, Limsricharoen K, Pukrittayakamee P, Wannarit K. Mental health problems of medical students retired from the Faculty of Medicine, Siriraj Hospital, 1982-2007. J Psychiatr Assoc Thailand. 2013;58(3):271-282.
Saravanan C, Wilks R. Medical students’ experience of and reaction to stress: the role of depression and anxiety. The Scientific World Journal. 2014;1-8. doi: http://dx.doi.org/10.1155/2014/737382
Zeng W, Chen R, Wang X, Zhang Q, Deng W. Prevalence of mental health problems among medical students in China. Medicine. 2019;98:18. doi: 10.1097/MD.0000000000015337.
Heizomi H, Kouzekanani K, Jafarabadi MA, Allahverdipour H. Psychometric properties of the Persian version of Mental Health Literacy Scale. Int J Womens Health. 2020;12: 513-520. doi: https://doi.org/10.2147/IJWH.S252348.
Shaw SJ, Huebner C, Armin, J, Orzech K, Vivian J. The role of culture in health literacy and chronic disease screening and management. J Immigrant Minority Health. 2009;11: 460–467. doi: https://doi.org/10.1007/s10903-008-9135-5.
Kaewprom C, Yuthavisut S, Pratoom L, Boontum A. Mental health literacy among village health workers: a case study of two sub-districts in Kloong, Chantaburi. Journal of health science research. 2014;8(1):10-16.
Ganasen KA, Parker S, Hugo CJ, Stein DJ, Emsley RA, Seedat S. Mental health literacy: focus on developing countries. Afr J Psychiatry (Johannesbg). 2008;11(1):23-28. doi: 10.4314/ajpsy. v11i1.30251.
Kermode M, Bowen K, Arole S, Pathare S, Jorm AF. Attitudes to people with mental disorders: a mental health literacy survey in a rural area of Maharashtra, India. Soc Psychiat Epidemiol. 2009;44:1087–1096. doi: 10.1007/s00127-009-0031-7.
Letonja M, Duh M. Knowledge transfer in family businesses and its effects on the innovativeness of the next family generation. Knowledge Management Research & Practice. 2016;
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














