Incidence and Risk Factors of Neonatal Sepsis in Preterm Premature Rupture of Membranes before 34 Weeks of Gestation
DOI:
https://doi.org/10.33192/Smj.2022.21Keywords:
Early-onset neonatal sepsis, incidence, PPROM, risk factorsAbstract
Objective: Early-onset neonatal sepsis (EONS) is a leading cause of newborn morbidity and mortality, particularly in preterm premature rupture of membranes (PPROM) before 34 weeks of gestation, in which expectant management was performed until reaching 34 weeks of gestation, evidence of maternal chorioamnionitis, or unfavorable fetal conditions. The interval between membrane rupture and delivery has a positive correlation with neonatal sepsis. The purpose of this study was to investigate the incidence and risk factors of EONS in PPROM.
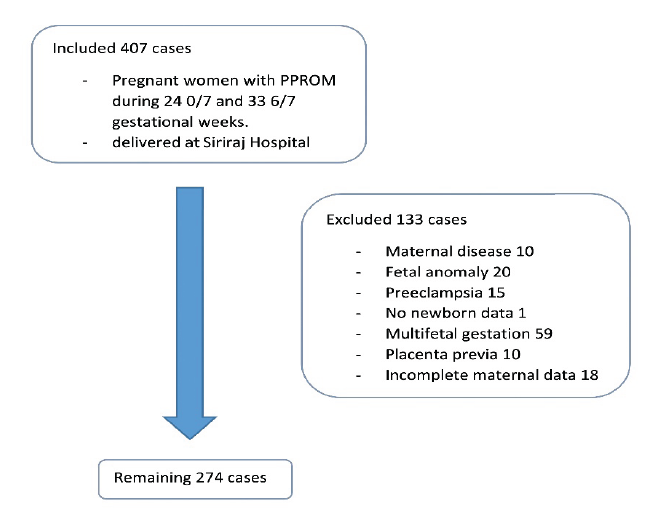
Materials and Methods: This was a retrospective cross-sectional study. The medical records of pregnant women who gave birth between 2005 and 2018 and their newborns were reviewed. The inclusion criterion was singleton pregnancies complicated by PPROM between 24 and 33+6 weeks of gestation. Multifetal pregnancies, fetal malformation, stillbirths, and records with incomplete data were excluded. PPROM was diagnosed by obstetricians while EONS was diagnosed by neonatologist.
Results: The incidence of EONS in with PPROM was 24%. Risk factors included excessive maternal weight gain based on IOM (OR = 2.40, 95% CI = 1.16-4.94), extremely preterm at admission (before 28 weeks of gestation) (OR = 3.38, 95% CI 1.12-10.21) and very low birth weight (≤ 1,500 g) (OR 3.68, 95% CI = 1.86-7.30). Maternal hematologic laboratory results were not associated with neonatal sepsis.
Conclusion: The incidence of EONS in PPROM was similar to data provided by other studies. Obstetricians and pediatricians should be cautious about neonatal sepsis, especially in cases of excessive maternal weight gain, extremely preterm admissions, and very low birth weight.
References
Chawanpaiboon S, Kanokpongsakdi S. Preterm birth at Siriraj Hospital: a 9-year period review (2002-2010). Siriraj Med J. 2020;63:143-6.
Prechapanich J, Tongtub E. Retrospective review of the relationship between parity and pregnancy outcomes at Siriraj Hospital. Siriraj Med J. 2020;62:14-7.
Cunnimgham FG, Leveno KJ, Bloom SL, Dashe JS, Hoffman BL, Casey BM, et al. Preterm birth. In: Cunningham FG, Leveno KJ, Bloom SL, Dashe JS, Hoffman BL, Casey BM, Spong CY, eds. Williams Obstetrics, 25th ed. New York:McGraw-Hill, 2018. p.803-34.
Sae-lin P, Wanitpongpan P. Incidence and risk factors of preterm premature rupture of membranes in singleton pregnancies at Siriraj Hospital. J Obstet Gynecol Res. 2019;45:573-7.
Martius JA, Roos T, Gora B, et al. Risk factors associated with early-onset sepsis in premature infants. Eur J Obstet Gynecol Reprod Biol. 1999;85:151-8.
Triniti A, Suthatvorawut S, O-Prasertsawat P. Epidermiologic study of cervical swab culture in preterm premature rupture of membrane (PPROM) at Ramathibodi Hospital. Thai J Obstet Gynaecol. 2008;16:173-8.
Ocviyanti D, Wahono WT. Risk factors for neonatal sepsis in pregnant women with premature rupture of the membrane. J Pregnancy. 2018;2018:4823404.
Simonsen KA, Anderson-Berry AL, Delair SF, Davies HD. Early-onset neonatal sepsis. Clin Microbiol Rev. 2014;27:21-47.
Prelabor rupture of membranes: ACOG Practice Bulletin, Number 217. Obstet Gynecol. 2020;135:e80-97.
Arora P, Bagga R, Kalra J, Kumar P, Radhika S, Gautam V. Mean gestation at delivery and histological chorioamnionitis correlates with early-onset neonatal sepsis following expectant management in pPROM. J Obstet Gynaecol. 2015;35:235-40.
Rasmussen KM, Yaktine AL, Institute of Medicine (US) and National Research Council (US) Committee to reexamine IOM pregnancy weight guidelines, eds. Weight gain during pregnancy: reexamining the guidelines. Washington (DC): National Academies Press (US); 2009.
Titapant V, Lertbunnaphong T, Pimsen S. Is the U.S. Institute of Medicine recommendation for gestational weight gain suitable for Thai singleton pregnant Women? J Med Assoc Thai. 2013;96:1-6.
Puopolo KM, Benitz WE, Zaoutis TE; Committee on Fetus and Newborn; Committee on Infectious Diseases. Management of neonates born at ≥35 0/7 weeks’ gestation with suspected or proven early-onset bacterial sepsis. Pediatrics. 2018;142(6):e20182894.
Armstrong C. ACOG guidelines on premature rupture of membranes. Am Fam Physician. 2008;77:245-6.
Alam MM, Saleem AF, Shaikh AS, Munir O, Qadir M. Neonatal sepsis following prolonged rupture of membranes in a tertiary care hospital in Karachi, Pakistan. J Infect Dev Ctries. 2014;8:67‐73.
Asindi AA, Archibong EI, Mannan NB. Mother-infant colonization and neonatal sepsis in prelabor rupture of membranes. Saudi Med J. 2002;23:1270-4.
Stotland NE, Cheng YW, Hopkins LM, Caughey AB. Gestational weight gain and adverse neonatal outcome among term infants. Obstet Gynecol 2006;108:635-43.
Rastogi S, Rojas M, Rastogi D, Haberman S. Neonatal morbidities among full-term infants born to obese mothers. J Matern Fetal Neonatal Med. 2015;28:829-35.
Villamor E, Norman M, Johansson S, Cnattingius S. Maternal obesity and risk of early-onset neonatal bacterial sepsis: nationwide cohort and sibling-controlled studies. Clin Infect Dis. 2020;ciaa783.
Ferrante AW. Obesity-induced inflammation: a metabolic dialogue in the language of inflammation. J Intern Med. 2007;262:408–14.
Misra VK, Straughen JK, Trudeau S. Maternal serum leptin during pregnancy and infant birth weight: the influence of maternal overweight and obesity. Obesity. 2013;21:1064–9.
Belachew A, Tewabe T. Neonatal sepsis and its association with birth weight and gestational age among admitted neonates in Ethiopia: systematic review and meta-analysis. BMC Pediatr. 2020;20:55.
Thavarajah H, Flatley C, Kumar S. The relationship between the five minute Apgar score, mode of birth and neonatal outcomes. J Matern Fetal Neonatal Med. 2018;31:1335‐41.
Softic I, Tahirovic H, Di Ciommo V, Auriti C. Bacterial sepsis in neonates: single centre study in a neonatal intensive care unit in Bosnia and Herzegovina. Acta Med Acad. 2017;46:7-15.
Xie A, Zhang W, Chen M, et al. Related factors and adverse neonatal outcomes in women with preterm premature rupture of membranes complicated by histologic chorioamnionitis. Med Sci Monit. 2015;21:390-5.
Mamopoulos A, Petousis S, Tsimpanakos J, et al. Birth weight independently affects morbidity and mortality of extremely preterm neonates. J Clin Med Res. 2015;7:511-6.
Berggren E, Hickey K. 805: Clinical relevance of leukocytosis in preterm premature rupture of membranes. Am J Obstet Gynecol. 2008;199:S227.
Amirabi A, Naji S, Yekta Z, Sadeghi Y. Chorioamnionitis and diagnostic value of C-reactive protein, erythrocyte sedimentation rate and white blood cell count in its diagnosis among pregnant women with premature rupture of membranes. Pak J Biol Sci. 2012;15:454-8.
Perrone G, Anceschi MM, Capri O, et al. Maternal C-reactive protein at hospital admission is a simple predictor of funisitis in preterm premature rupture of membranes. Gynecol Obstet Invest. 2012;74:95-9.
Cho HY, Jung I, Kwon JY, Kim SJ, Park YW, Kim YH. The Delta Neutrophil Index as a predictive marker of histological chorioamnionitis in patients with preterm premature rupture of membranes: A retrospective study. PLoS One. 2017;12:e0173382.
Popowski T, Goffinet F, Batteux F, Maillard F, Kayem G. Prediction of maternofetal infection in preterm premature rupture of membranes: serum maternal markers. Gynecol Obstet Fertil. 2011;39:302-8.
Panwar C, Kaushik SL, Kaushik R, Sood A. Correlation of neonatal and maternal clinico-hematological parameters as predictors of early onset neonatal sepsis. Int J Contemp Pediatr. 2017;4:36-42.
Mayuga WAB, Isleta PFD. Clinical correlation of neonatal and maternal hematological parameters as predictors of neonatal sepsis. PIDSP Journal. 2005;9:36-43.
Diebel ND, Parsons MT, Spellacy WN. The effects of betamethasone on white blood cells during pregnancy with PPROM. J Perinat Med. 1998;26:204-7.
Ozel A, Davutoglu AE, Yurtkal A, Madazli R. How do plateletto-lymphocyte ratio and neutrophil-to-lymphocyte ratio change in women with preterm premature rupture of membranes, and threaten preterm labour? J Obstet Gynaecol. 2020;40:195-9.
Chayawongrungreung T, Luengmettakul J, Srilar A. Relationship between antenatal maternal neutrophil-to-lymphocyte ratio and early onset neonatal sepsis in preterm neonates. Thai J Obstet Gynaecol. 2020;28:94-102.
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














