Incidence of Adverse Perioperative Airway Complications in Obese Non-Pregnant and Pregnant Patients Undergoing General Anesthesia
DOI:
https://doi.org/10.33192/Smj.2022.22Keywords:
Airway, obesity, perioperative, complicationAbstract
Objective: Airway complications in obese patients are a major concern during surgical operation. This study aimed to determine the incidence of airway- and respiratory-related anesthetic complications for obese (including maternal) patients undergoing general anesthesia.
Materials and Methods: This multicenter, retrospective, observational study evaluated obese female patients (BMI≥ 30 kg/m2), both non-pregnant and pregnant, undergoing general anesthesia in 5 hospitals across Thailand during May 2013 - August 2016. The primary observation was anesthesia-related airway complications (difficult and failed intubations, aspiration, desaturation, and airway injuries) detected during anesthesia. An analysis was performed to compare the incidents of the adverse events and to determine the risk factors for airway-related adverse events in both groups.
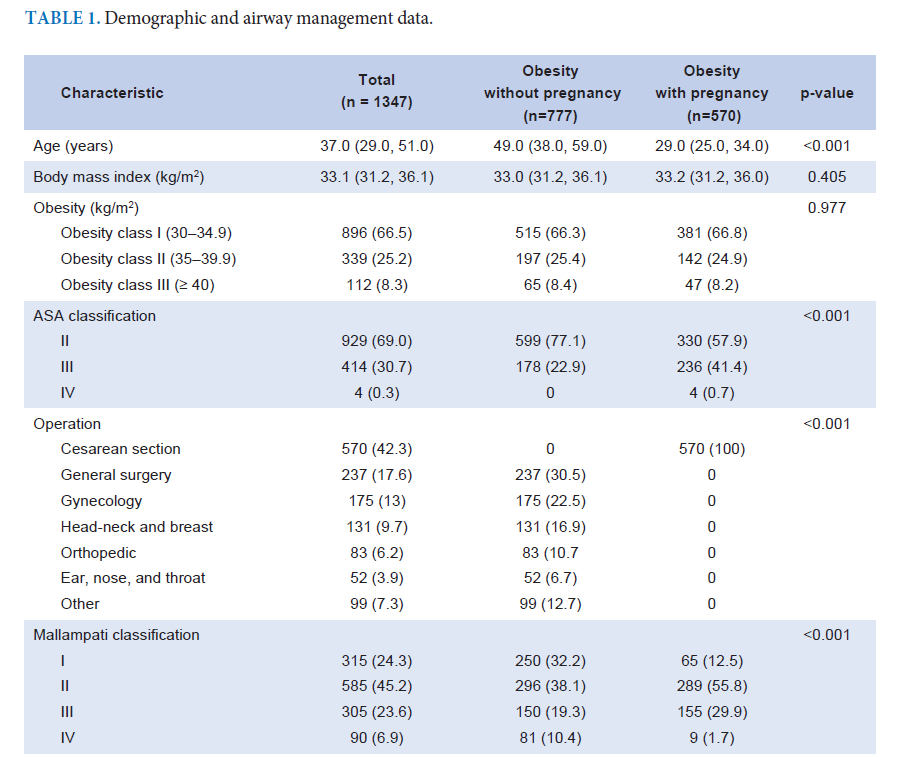
Results: There were 1,347 obese patients enrolled (777 non-pregnant and 570 pregnant). The overall incidence of airway and respiratory complications was observed in 129 patients (9.6%), with a higher rate in pregnant patients (12.5% vs. 7.5%; p<0.05). The most common complications were desaturation (5.6%) followed by airway injuries (3.6%) and difficult intubation (1.5%). The factors significantly associated with adverse airway-related events were obesity class II (OR=1.63 [1.05–2.54]), obesity class III (OR=2.25 [1.19–4.25]), pregnancy (OR=1.73 [1.18–2.54]), Mallampati classifications III–IV (OR=1.69 [1.16–2.48]), and neck circumference <43 cm (OR=3.33 [1.02-10.81]), p<0.05).
Conclusion: The incidence of the anesthesia-related airway and respiratory complications was 9.6%, with a higher rate in pregnant patients. The most common adverse airway event was desaturation. However, the frequency of serious airway events was low.
References
Expert Panel on the Identification, Evaluation, and Treatment of Overweight in Adults. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults: executive summary. Am J Clin Nutr. 1998;68(4):899-917.
Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of Obesity Among Adults and Youth: United States, 2015–2016. NCHS data brief, no 288. Hyattsville, MD: National Center for Health Statistics. 2017.
Fryar CD, Carroll MD, Ogden CL. Prevalence of Overweight, Obesity, and Extreme Obesity Among Adults Aged 20 and Over: United States, 1960–1962 Through 2013–2014. National health statistics reports Hyattsville, MD: National Center for Health Statistics. 2016.
Rodanant O, Chau-in W, Charuluxananan S, Morakul S, Pongruekdee S, Tanyong U, Chanthawong S, et al. The perioperative and anesthetic adverse events in Thailand (PAAd Thai) study: 58 case reports of obesity patients. J Med Assoc Thai. 2019;102:320-6.
Wang T, Sun S, Huang S. The association of body mass index with difficult tracheal intubation management by direct laryngoscopy: a meta-analysis. BMC Anesthesiol. 2018;18(1):79.
Kim WH, Ahn HJ, Lee CJ, Shin BS, Ko JS, Choi SJ, et al. Neck circumference to thyromental distance ratio: a new predictor of difficult intubation in obese patients. Br J Anaesth. 2011;106(5): 743-8.
Robinson M, Davidson A. Aspiration under anaesthesia: risk assessment and decision-making. Cont Educ Anaesth Crit Care Pain. 2013;14(4):171-5.
Visalyaputra, S. Maternal Mortality Related to Anesthesia: Can It be Prevented? Siriraj Med J. 2002;54(9):533-9.
Adnet F, Borron SW, Racine SX, Clemessy JL, Fournier JL, Plaisance P, et al. The intubation difficulty scale (IDS): proposal and evaluation of a new score characterizing the complexity of endotracheal intubation. Anesthesiology. 1997;87(6):1290-7.
Uakritdathikarn T, Chongsuvivatwong V, Geater AF, Vasinanukorn M, Thinchana S, Klayna S. Perioperative desaturation and risk
factors in general anesthesia. J Med Assoc Thai. 2008;91(7):1020-9.
Nason KS. Acute Intraoperative Pulmonary Aspiration. Thorac Surg Clin. 2015;25(3):301-7.
Charuluxananan S, Punjasawadwong Y, Suraseranivongse S, Srisawasdi S, Kyokong O, Chinachoti T, et al. The Thai Anesthesia Incidents Study (THAI Study) of anesthetic outcomes: II. Anesthetic profiles and adverse events. J Med Assoc Thai. 2005;88:S14-29.
Lotia S, Bellamy MC. Anaesthesia and morbid obesity. BJA Education. 2008;8(5):151-6.
Bedson R, Riccoboni A. Physiology of pregnancy: clinical anaesthetic implications. Cont Educ Anaesth Crit Care Pain. 2013;14(8):69-72.
Gupta A, Faber P. Obesity in pregnancy. Cont Educ Anaesth Crit Care Pain. 2011;11:143–6.
Chau-in W, Hintong T, Rodanant O, Lekprasert V, Punjasawadwong Y, Charuluxananan S, et al. Anesthesia-related complications of caesarean delivery in Thailand: 16,697 cases from the Thai Anaesthesia Incidents Study. J Med Assoc Thai. 2010;93(11)1274-83.
Chau-In W, Rodanant O, Chanthawong S, Punjasawadwong Y, Charuluxananan S, Lekprasert V, et al. Perioperative anesthetic Adverse Events in Thailand (PAAd Thai): Incident reporting study: an analysis of 69 perioperative adverse events in patients undergoing cesarean section. J Med Assoc Thai. 2018;101(6):821-8.
Minville V, Gonzalez H, Fourcade O. Neck Circumference and Difficult Intubation. Anesthesia & Analgesia. 2008;107(5):1757.
De Jong A, Molinari N, Pouzeratte Y, Verzilli D, Chanques G, Jung B, et al. Difficult intubation in obese patients: incidence, risk factors, and complications in the operating theatre and in intensive care units. Br J Anaesth. 2014;114(2):297-306.
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














