Burnout among Mental Health Professionals in a Tertiary University Hospital
DOI:
https://doi.org/10.33192/Smj.2022.23Keywords:
Burnout, coping strategies, health care professionals, personality traitsAbstract
Objective: To examine the level of burnout syndrome, and to investigate the relationship between burnout, personality traits, coping strategies, and other related personal factors among mental health professionals working in a tertiary hospital.
Materials and Methods: Online questionnaires were sent to 160 mental health professionals at Siriraj Hospital. The questionnaire comprised questions collecting demographic data, the Copenhagen Burnout Inventory (Thai version), the Big Five Inventory, and the Coping Scale. The data were analyzed through descriptive statistics, analysis of variance, Pearson correlation, and stepwise multiple regression.
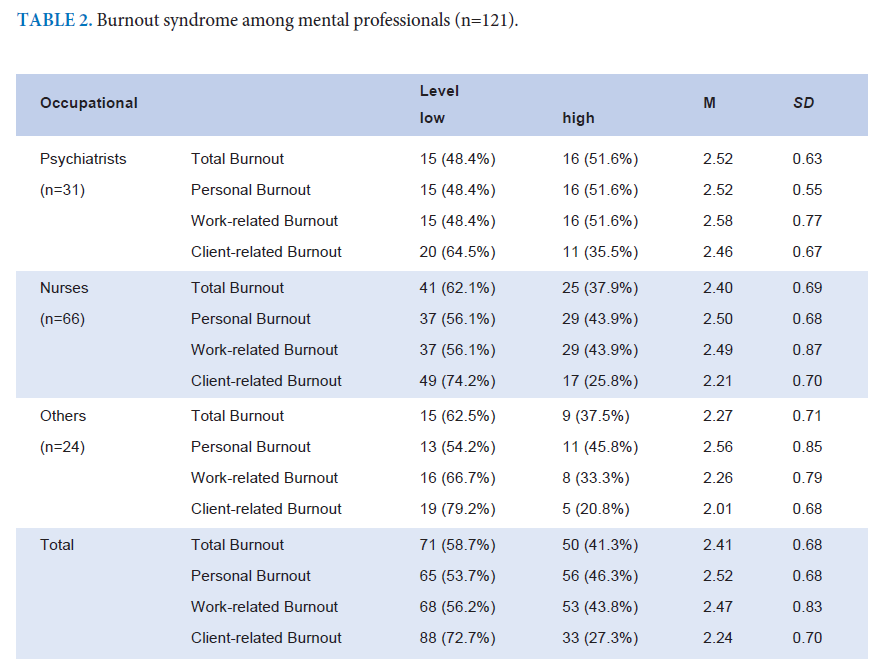
Results: A total of 121 (75.6%) responses were collected. Of the 121 participants, 41.3% reported high total burnout levels. However, no difference in total burnout was found between the different mental health professions. The group aged between 20-29 years demonstrated higher burnout than the others. Individuals with bachelor’s and master’s degrees showed greater burnout than those with lower than undergraduate degrees. Moreover, individuals who worked for less than five years had higher burnout than those in other groups. Furthermore, neuroticism and avoidance significantly predicted the burnout syndrome.
Conclusion: In contrast to previous studies in Thailand, the results highlighted the risk factors for burnout syndrome in terms of personal, work-related, and client-related burnout. These results can strengthen awareness surrounding mental health conditions, for the effective provision of psychoeducation and psychological interventions.
References
World Health Organization. Burnout-out an “occupational phenomenon” 2019 [18 Oct 2019]. Available from: https://www.who.int/mental_health/evidence/burn-out/en/.
Maslach C, Jackson SE. The measurement of experienced burnout. Journal of Occupational Behaviour. 1981;2:99-103.
Magnavita N, Heponiemi T, Chirico F. Workplace Violence Is Associated With Impaired Work Functioning in Nurses: An Italian Cross-Sectional Study. J Nurs Scholarsh. 2020;52(3):281-91.
Chirico F, Ferrari G, Nucera G, Szarpak Ł, Crescenzo P, Ilesanmi O. Prevalence of anxiety, depression, burnout syndrome, and mental health disorders among healthcare workers during the COVID-19 pandemic: A rapid umbrella review of systematic reviews. Journal of Health and Social Sciences. 2021;6:209-20.
Borritz M, Rugulies R, Bjorner JB, Villadsen E, Mikkelsen OA, Kristensen TS. Burnout among employees in human service work: design and baseline findings of the PUMA study. Scan J Public Health. 2006;34(1):49-58.
Bahrer-Kohler S. Burnout for Experts: Prevention in the Context of Living and Working. Basel, Switzerland: Springer, Boston, MA; 2013.
Pejuskovic B, Lecic-Tosevski D, Priebe S, Toskovic O. Burnout syndrome among physicians - the role of personality dimensions and coping strategies. Psychiatr Danub. 2011;23(4):389-95.
Lue B-H, Chen H-J, Wang C-W, Cheng Y, Chen M-C. Stress, personal characteristics and burnout among first postgraduate year residents: a nationwide study in Taiwan. Medical Teacher. 2010;32(5):400-7.
Afshar H, Roohafza HR, Keshteli AH, Mazaheri M, Feizi A, Adibi P. The association of personality traits and coping styles according to stress level. J Res Med Sci. 2015;20(4):353-8.
Pitanupong J, Jatchavala C. A Study on the Comparison of Burnout Syndrome, Among Medical Doctors in the Restive Areas and Non-Restive Areas of the South Thailand Insurgency. J Health Sci Med Res. 2018;36(4):277-89.
Chatlaong T, Pitanupong J, Wiwattanaworaset P. Sleep Quality and Burnout Syndrome among Residents in Training at the Faculty of Medicine, Prince of Songkla University. Siriraj Med J. 2020;72(4):307-14.
Felton JS. Burnout as a clinical entity—its importance in health care workers. Occupational Medicine. 1998;48(4):237-50.
Chirico F, Capitanelli I, Bollo M, Ferrari G, Acquadro Maran D Association between workplace violence and burnout syndrome among schoolteachers: A systematic review. Journal of Health and Social Sciences. 2021;6:187-208.
Chirico F, Crescenzo P, Sacco A, Riccò M, Ripa S, Nucera G, et al. Prevalence of burnout syndrome among Italian volunteers of the Red Cross: a cross-sectional study. Industrial Health. 2021;59:117-27.
Morse G, Salyers MP, Rollins AL, Monroe-DeVita M, Pfahler C. Burnout in mental health services: a review of the problem and its remediation. Adm Policy Ment Health. 2012;39(5):341-52.
Maslach C, Schaufeli W, Leiter M. Job burnout. Annu Rev Psychol. 2001;52:397.
Phuekphan P, Aungsuroch Y, Yunibhand J, Chan SW-C. Psychometric properties of the Thai version of copenhagen burnout inventory (T-CBI) in Thai nurses. Journal of Health Research. 2016;30(2):135-42.
Banlue K. Narcissism and five-factor personality as predictors of leader emergence in an unacquainted group. Chulalongkorn University: Chulalongkorn University; 2010.
Benet-Matinez V, John O. Los Cinco Grandes Across Cultures and Ethnic Groups: Multitrait Multimethod Analyses of the Big Five in Spanish and English. J Pers Soc Psychol. 1998;75:729-50.
Leksomboon P. Job stress, coping, and burnout among helping practitioners in public welfare centers: a mixed methods research: Chulalongkorn University; 2011.
Ndetei DM, Pizzo M, Maru H, Ongecha FA, Khasakhala LI, Mutiso V, et al. Burnout in staff working at the Mathari psychiatric hospital. Afr J Psychiatry (Johannesbg). 2008;11(3):199-203.
Ogresta J, Rusac S, Zorec L. Relation between burnout syndrome and job satisfaction among mental health workers. Croat Med J. 2008;49(3):364-74.
Nimmawitt N, Wannarit K, Pariwatcharakul P. Thai psychiatrists and burnout: A national survey. PLoS One. 2020;15(4):e0230204.
Creedy DK, Sidebotham M, Gamble J, Pallant J, Fenwick J. Prevalence of burnout, depression, anxiety and stress in Australian midwives: a cross-sectional survey. BMC Pregnancy Childbirth. 2017;17(1):13.
Žutautienė R, Radišauskas R, Kaliniene G, Ustinaviciene R. The Prevalence of Burnout and Its Associations with Psychosocial Work Environment among Kaunas Region (Lithuania) Hospitals’ Physicians. Int J Environ Res Public Health. 2020;17(10):3739.
Chou L-P, Li C-Y, Hu SC. Job stress and burnout in hospital employees: comparisons of different medical professions in a regional hospital in Taiwan. BMJ Open. 2014;4(2):e004185.
Binub K. Burnout among health professionals in a tertiary medical college of northern Kerala, India. International Journal of Community Medicine And Public Health. 2018;6:229.
Oyefeso A, Clancy C, Farmer R. Prevalence and associated factors in burnout and psychological morbidity among substance misuse professionals. BMC Health Serv Res. 2008;8:39.
Kumar S, Officer IAFM, Vijai M, Anaesthesiologist IAF. Mental stress, and burnout among COVID warriors - A new healthcare crisis. JMR. 2020;6(5):193-6.
Chakraborty R, Chatterjee A, Chaudhury S. Internal predictors of burnout in psychiatric nurses: An Indian study. Ind Psychiatry J. 2012;21(2):119-24.
Green AE, Albanese BJ, Shapiro NM, Aarons GA. The roles of individual and organizational factors in burnout among community-based mental health service providers. Psychol Serv. 2014;11(1):41-9.
Shimizutani M, Odagiri Y, Ohya Y, Shimomitsu T, Kristensen TS, Maruta T, et al. Relationship of Nurse Burnout with Personality Characteristics and Coping Behaviors. Ind Health. 2008;46(4):326-35.
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














