A Comparative Study Using CT Imaging and Cadaveric Dissection in the Evaluation of the Posterior Auricular Vein as an Alternative Recipient Vein for Facial and Scalp Reconstructions
DOI:
https://doi.org/10.33192/smj.v77i9.276227Keywords:
Posterior Auricular Vein, Superficial Temporal Vein, Microvascular Surgery, Cranial Computed Tomography, Cadaveric DissectionAbstract
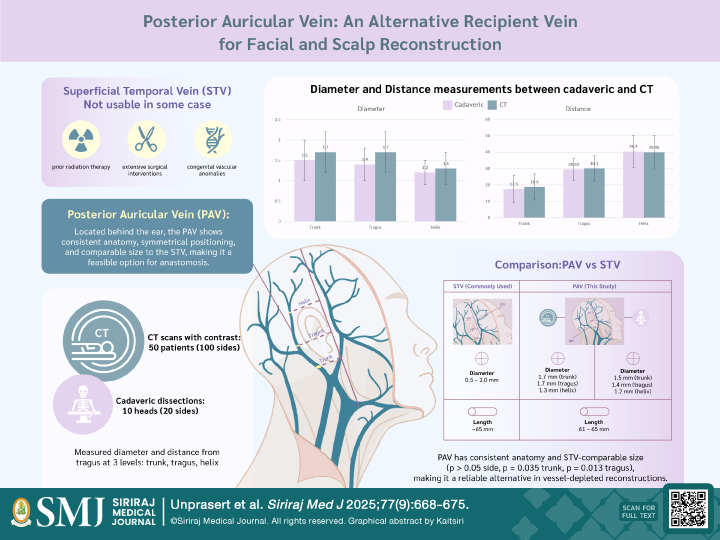
Objective: To determine the diameter and anatomical location of the posterior auricular vein (PAV) and evaluate its suitability as an alternative recipient vein to the superficial temporal vein in microvascular facial and scalp reconstruction.
Materials and Methods: A retrospective study was conducted using 50 contrast-enhanced cranial CT scans (100 sides) and anatomical dissections on 10 fresh cadaveric heads (20 sides) between 2015 and 2019 at Siriraj Hospital, Mahidol University. Measurements of PAV diameter and its distance from the vertical tragus line were recorded at the trunk, tragus, and helix levels. Descriptive statistics and side-to-side comparisons were analyzed using appropriate analytical tools.
Results: CT scans showed mean PAV diameters of 1.74 mm (trunk), 1.67 mm (tragus), and 1.33 mm (helix). Corresponding measurements from cadaveric dissections were 1.47 mm, 1.39 mm, and 1.16 mm, respectively. The 95% confidence intervals confirmed anatomical consistency and bilateral symmetry. The harvestable length of the PAV reached up to 65 mm on CT) and 61 mm on cadaveric dissection, comparable to the superficial temporal vein. No significant differences in positional measurements (distance from the tragus) were found between methods or sides (p > 0.05).
Conclusion: The posterior auricular vein demonstrates consistent anatomical parameters and a diameter comparable to the superficial temporal vein. These findings support its feasibility as a reliable alternative for venous anastomosis in facial and scalp microvascular reconstruction, especially in vessel-depleted cases.
References
Hansen SL, Foster RD, Dosanjh AS, Mathes SJ, Hoffman WY, Leon P. Superficial temporal artery and vein as recipient vessels for facial and scalp microsurgical reconstruction. Plast Reconstr Surg. 2007;120(7):1879–84.
Delgove L, Lebeau J, Raphaël B, Champetier J. Drainage of the scalp by the superficial temporal vein: surgical implications. Surg Radiol Anat. 1991;13(4):277–82.
Kushida-Contreras BH, Manrique OJ, Gaxiola-García MA. Head and neck reconstruction of the vessel-depleted neck: a systematic review of the literature. Ann Surg Oncol. 2021;28(5):2882–95.
Fichter AM, Wolff KD. Reconstructive options in the vessel-depleted neck: past, present and future strategies. Innovations and New Developments in Craniomaxillofacial Reconstruction. 2021;211–26.
Prince AD, Broderick MT, Neal MEH, Spector ME. Head and neck reconstruction in the vessel depleted neck. Front Oral Maxillofac Med. 2020;2:13.
Chopra K, Williams N, van Zyl A. Adjunctive application of Integra® in free-flap surgery for scalp defects. Int Med Case Rep J. 2022;15:483–91. doi:10.2147/IMCRJ.S509768.
Bechmann S, Rahman S, Kashyap V. Anatomy, head and neck, external jugular veins. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019.
Kim DJ, Park H. Use of the frontal branch of the superficial temporal artery and the postauricular vein to overcome anatomic variations of superficial temporal vessels in scalp reconstruction with free tissue transfer: a case report. Arch Craniofac Surg. 2024;25(2):145–9. doi:10.7181/acfs.2024.00073.
Lassus P, Lindford A. The temporal artery posterior auricular skin flap for head and neck reconstruction. Head Neck. 2017;39(12):2434–41. doi:10.1002/hed.24894.
Leedy JE, Janis JE, Rohrich RJ. Reconstruction of acquired scalp defects: an algorithmic approach. Plast Reconstr Surg. 2005;116(7):54e–72e. doi:10.1097/01.prs.0000179188.25019.6c.
Nokovitch L, Devauchelle B, Peyrachon B, Vacher C, Deneuve S. Caractéristiques anatomiques du système veineux temporal superficiel et implications en microchirurgie. Ann Chir Plast Esthet. 2021;66(3):250–6.
Chen JT, Sanchez R, Garg R, Poore S, Siebert JW. Helpful hints for the superficial temporal artery and vein as recipient vessels. Plast Reconstr Surg. 2017;139(3):818e–20e.
Paech D, Klopries K, Nawrotzki R, Schlemmer HP, Giesel FL, Kirsch J, et al. Strengths and weaknesses of non-enhanced and contrast-enhanced cadaver computed tomography scans in the teaching of gross anatomy in an integrated curriculum. Anat Sci Educ. 2022;15(1):143–54.
Schramek GGR, Stoevesandt D, Reising A, Kielstein JT, Hiss M, Kielstein H. Imaging in anatomy: a comparison of imaging techniques in embalmed human cadavers. BMC Med Educ. 2013;13:1–7.
Imanishi N, Nakajima H, Minabe T, Chang H, Aiso S. Venous drainage architecture of the temporal and parietal regions: anatomy of the superficial temporal artery and vein. Plast Reconstr Surg. 2002;109(6):2197–203.
Onishi S, Imanishi N, Yoshimura Y, Inoue Y, Sakamoto Y, Chang H, et al. Venous drainage of the face. J Plast Reconstr Aesthet Surg. 2017;70(3):433–40.
Published
How to Cite
License
Copyright (c) 2025 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














