Effects of Forward Leaning Characteristics on Protective Steps when Performing Voluntary- induced Stepping Response in Young and Older Adults: A Cross-Sectional Study
DOI:
https://doi.org/10.33192/smj.v78i3.278066Keywords:
Postural balance, accidental falls, gait, health, motor activityAbstract
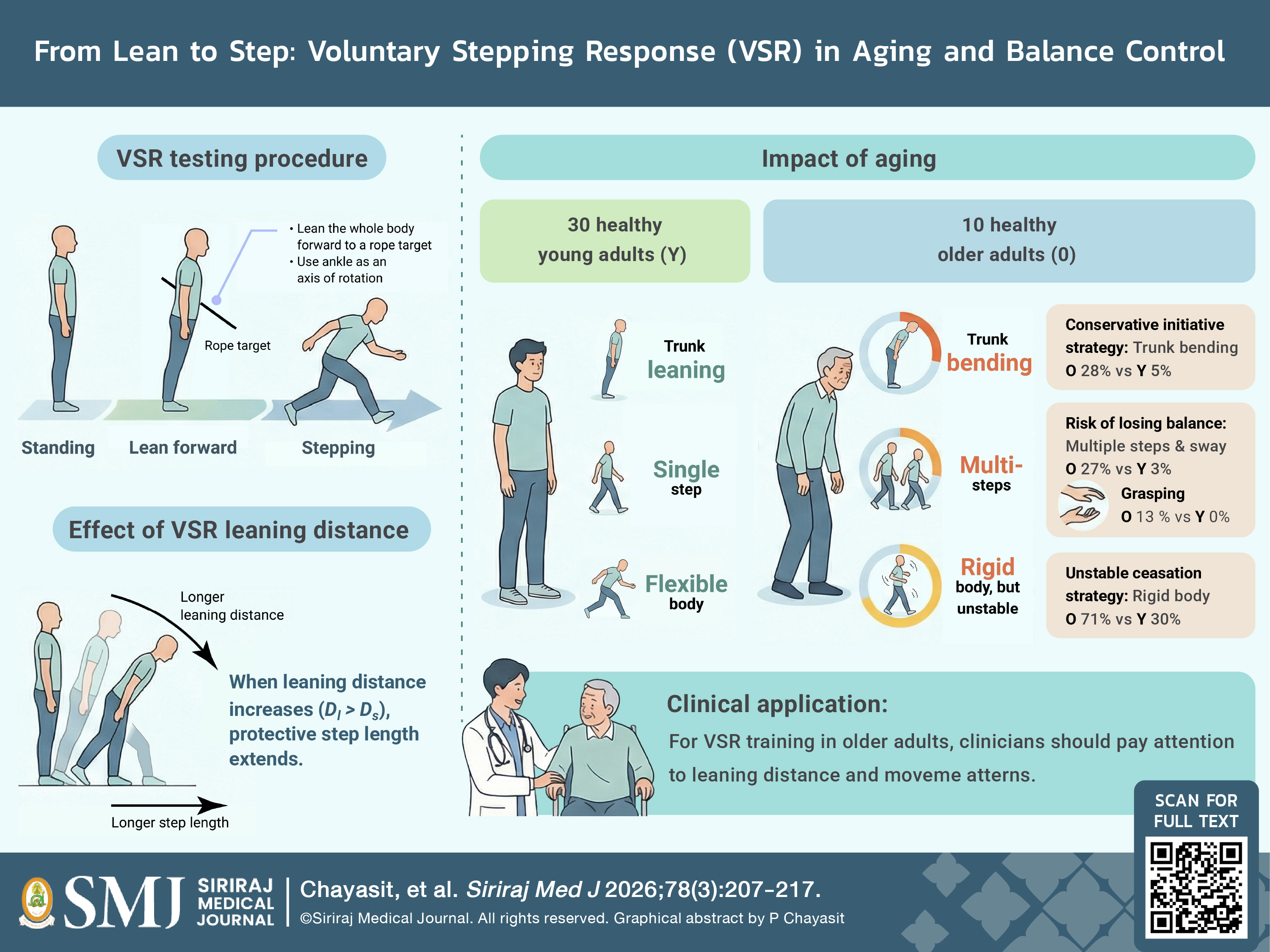
Objective: To examine the effect of forward leaning distance and aging on protective step length, movement strategies, and postural stability during voluntary-induced stepping response (VSR).
Materials and Methods: Thirty healthy young adults (19.5 ± 0.7 years) and ten healthy older adults (68.9 ± 4.4 years) participated in a cross-sectional study. Young adults performed VSR under two conditions: short-distance (Ds) and long-distance (Dl), based on pelvis displacement ratios. Older adults performed VSR at their preferred leaning distance (Dp) and were instructed to recover balance with a single step. Protective step length, movement initiation and cessation strategies, and postural stability were assessed using 2D video analysis. Statistical comparisons were conducted using paired t-tests and chi-square tests (α = 0.05).
Results: Step length was significantly greater in Dl than Ds (p < 0.001). Older adults in Dp showed no significant difference in step length compared to young adults in Dl. However, older adults more frequently used trunk bending (28% versus 5% of trials), rigid body strategies (71% versus 30%), grasping (13% versus 0%), body sway, and multi-step responses (27% versus 3%) (p < 0.001).
Conclusion: Forward-leaning distance influences step length during VSR. Aging is linked to altered movement strategies and reduced postural control. These findings suggest that VSR may serve as a targeted intervention to enhance dynamic stability in older adults, supporting broader goals of health promotion and overall well-being.
References
World Health Organization. Falls [Internet]. 2021. Available from: https://www.who.int/news-room/fact-sheets/detail/falls/.
James SL, Lucchesi LR, Bisignano C, Castle CD, Dingels ZV, Fox JT, et al. The global burden of falls: global, regional and national estimates of morbidity and mortality from the Global Burden of Disease Study 2017. Inj Prev. 2020;26(Suppl 1):i3-i11.
Gambaro E, Gramaglia C, Azzolina D, Campani D, Molin AD, Zeppegno P. The complex associations between late life depression, fear of falling and risk of falls. A systematic review and meta-analysis. Ageing Research Reviews. 2022;73:101532.
Monteiro YCM, Vieira MAdS, Vitorino PVdO, Queiroz SJd, Policena GM, Souza ACSE. Trend of fall-related mortality among the elderly. Rev Esc Enferm USP. 2021;55:e20200069.
Montero-Odasso M, van der Velde N, Martin FC, Petrovic M, Tan MP, Ryg J, et al. World guidelines for falls prevention and management for older adults: a global initiative. Age and Ageing. 2022;51(9):afac205.
Dajpratham P, Thitisakulchai P, Pongratanakul R, Prapavanond R, Haridravedh S, Muangpaisan W. Effectiveness of Personalized Multifactorial Fall Risk Assessment and Intervention in Reducing Fall Rates Among Older Adults: A Retrospective Study. Siriraj Medical Journal. 2025;77(1):64-72.
Bhatt T, Wang Y, Wang S, Kannan L. Perturbation Training for Fall-Risk Reduction in Healthy Older Adults: Interference and Generalization to Opposing Novel Perturbations Post Intervention. Front Sports Act Living. 2021;3:697169.
Chayasit P, Hollands K, Hollands M, Boonsinsukh R. Immediate effect of voluntary-induced stepping response training on protective stepping in persons with chronic stroke: a randomized controlled trial. Disabil Rehabil. 2022;44(3):420-7.
Chayasit P, Hollands K, Hollands M, Boonsinsukh R. Characteristics of Voluntary-induced Stepping Response in Persons with Stroke compared with those of healthy Young and Older Adults. Gait Posture. 2020;82:75-82.
Jensen JL, Brown LA, and Woollacott MH. Compensatory Stepping: The Biomechanics of a Preferred Response Among Older Adults. Experimental Aging Research. 2001;27(4):361-76.
Folstein MF, Folstein SE, McHugh PR. "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189-98.
Powell LE, Myers AM. The Activities-specific Balance Confidence (ABC) Scale. J Gerontol A Biol Sci Med Sci. 1995;50A(1):M28-M34.
Bohannon R, Shove M, Barreca S, Masters L, Sigouin C. Five-repetition sit-to-stand test performance by community-dwelling adults: A preliminary investigation of times, determinants, and relationship with self-reported physical performance. Isokinet Exerc Sci. 2007;15:77-81.
Lord SR, Murray SM, Chapman K, Munro B, Tiedemann A. Sit-to-stand performance depends on sensation, speed, balance, and psychological status in addition to strength in older people. J Gerontol A Biol Sci Med Sci. 2002;57(8):M539-43.
Shumway-Cook A, Baldwin M, Polissar NL, Gruber W. Predicting the probability for falls in community-dwelling older adults. Phys Ther. 1997;77(8):812-9.
Horak FB, Wrisley DM, Frank J. The Balance Evaluation Systems Test (BESTest) to differentiate balance deficits. Phys Ther. 2009;89(5):484-98.
Puig-Diví A, Escalona-Marfil C, Padullés-Riu JM, Busquets A, Padullés-Chando X, Marcos-Ruiz D. Validity and reliability of the Kinovea program in obtaining angles and distances using coordinates in 4 perspectives. PLoS One. 2019;14(6):e0216448.
Zhu RT, Lyu PZ, Li S, Tong CY, Ling YT, Ma CZ. How Does Lower Limb Respond to Unexpected Balance Perturbations? New Insights from Synchronized Human Kinetics, Kinematics, Muscle Electromyography (EMG) and Mechanomyography (MMG) Data. Biosensors (Basel). 2022;12(6).
Bair WN, Prettyman MG, Beamer BA, Rogers MW. Kinematic and behavioral analyses of protective stepping strategies and risk for falls among community living older adults. Clin Biomech (Bristol). 2016;36:74-82.
Lugade V, Lin V, Chou L-S. Center of mass and base of support interaction during gait. Gait & Posture. 2011;33(3):406-11.
Mille ML, Rogers MW, Martinez K, Hedman LD, Johnson ME, Lord SR, et al. Thresholds for Inducing Protective Stepping Responses to External Perturbations of Human Standing. Journal of Neurophysiology. 2003;90(2):666-74.
Zadravec M, Olenšek A, Rudolf M, Bizovičar N, Goljar N, Matjačić Z. Assessment of dynamic balancing responses following perturbations during slow walking in relation to clinical outcome measures for high-functioning post-stroke subjects. Journal of NeuroEngineering and Rehabilitation. 2020;17(1):85.
Horak FB, Nashner LM. Central programming of postural movements: adaptation to altered support-surface configurations. J Neurophysiol. 1986;55(6):1369-81.
Ren X, Lutter C, Kebbach M, Bruhn S, Bader R, Tischer T. Lower extremity joint compensatory effects during the first recovery step following slipping and stumbling perturbations in young and older subjects. BMC Geriatrics. 2022;22(1):656.
Payne AM, Ting LH. Worse balance is associated with larger perturbation-evoked cortical responses in healthy young adults. Gait & Posture. 2020;80:324-30.
Richard A, Van Hamme A, Drevelle X, Golmard J-L, Meunier S, Welter M-L. Contribution of the supplementary motor area and the cerebellum to the anticipatory postural adjustments and execution phases of human gait initiation. Neuroscience. 2017;358:181-9.
Radhakrishnan V, Gallea C, Valabregue R, Krishnan S, Kesavadas C, Thomas B, et al. Cerebellar and basal ganglia structural connections in humans: Effect of aging and relation with memory and learning. Frontiers in Aging Neuroscience. 2023;Volume 15 - 2023.
Zapparoli L, Mariano M, Paulesu E. How the motor system copes with aging: a quantitative meta-analysis of the effect of aging on motor function control. Communications Biology. 2022;5(1):79.
King GW, Akula CK, Luchies CW. Age-related differences in kinetic measures of landing phase lateral stability during a balance-restoring forward step. Gait & Posture. 2012;35(3):440-5.
Carty CP, Cronin NJ, Nicholson D, Lichtwark GA, Mills PM, Kerr G, et al. Reactive stepping behaviour in response to forward loss of balance predicts future falls in community-dwelling older adults. Age Ageing. 2015;44(1):109-15.
Singer JC, Prentice SD, McIlroy WE. Age-related challenges in reactive control of mediolateral stability during compensatory stepping: A focus on the dynamics of restabilisation. Journal of Biomechanics. 2016;49(5):749-55.
Tisserand R, Robert T, Chabaud P, Livet P, Bonnefoy M, Cheze L. Comparison between investigations of induced stepping postural responses and voluntary steps to better detect community-dwelling elderly fallers. Neurophysiol Clin. 2015;45(4-5):269-84.
Hof AL. Scaling gait data to body size. Gait Posture [Internet]. 1996;4:222-3 [cited 2026 Feb 4].
Pierrynowski MR, Galea V. Enhancing the ability of gait analyses to differentiate between groups: scaling gait data to body size. Gait Posture. 2001;13(3):193-201.
Rygelová M, Uchytil J, Torres IE, Janura M. Comparison of spatiotemporal gait parameters and their variability in typically developing children aged 2, 3, and 6 years. PLoS One. 2023;18(5):e0285558.
Mobbs L, Fernando V, Fonseka RD, Natarajan P, Maharaj M, Mobbs RJ. Normative Database of Spatiotemporal Gait Metrics Across Age Groups: An Observational Case–Control Study. Sensors [Internet]. 2025;25(2):581.
Eom GM, Kwon YR, Kim DY, Ko J, Kim JW. The influence of height on test-retest reliability of postural balance measures in healthy young adults. J Mech Med Biol. 2022;22(9).
Unluer N, Taş S. Effects of anthropometric factors, age, gender, and foot posture on single leg balance performance in asymptomatic subjects. Fizyoterapi Rehabilitasyon. 2019;30:154-60.
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2026 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














