Comparison of Local Versus General Anesthesia in Open Inguinal Hernioplasty: A Prospective Study on Postoperative Outcomes and Cost-Effectiveness
DOI:
https://doi.org/10.33192/smj.v78i4.280214Keywords:
Hernioplasty, Inguinal hernia, Local anesthesia, Day surgery, Cost-effectivenessAbstract
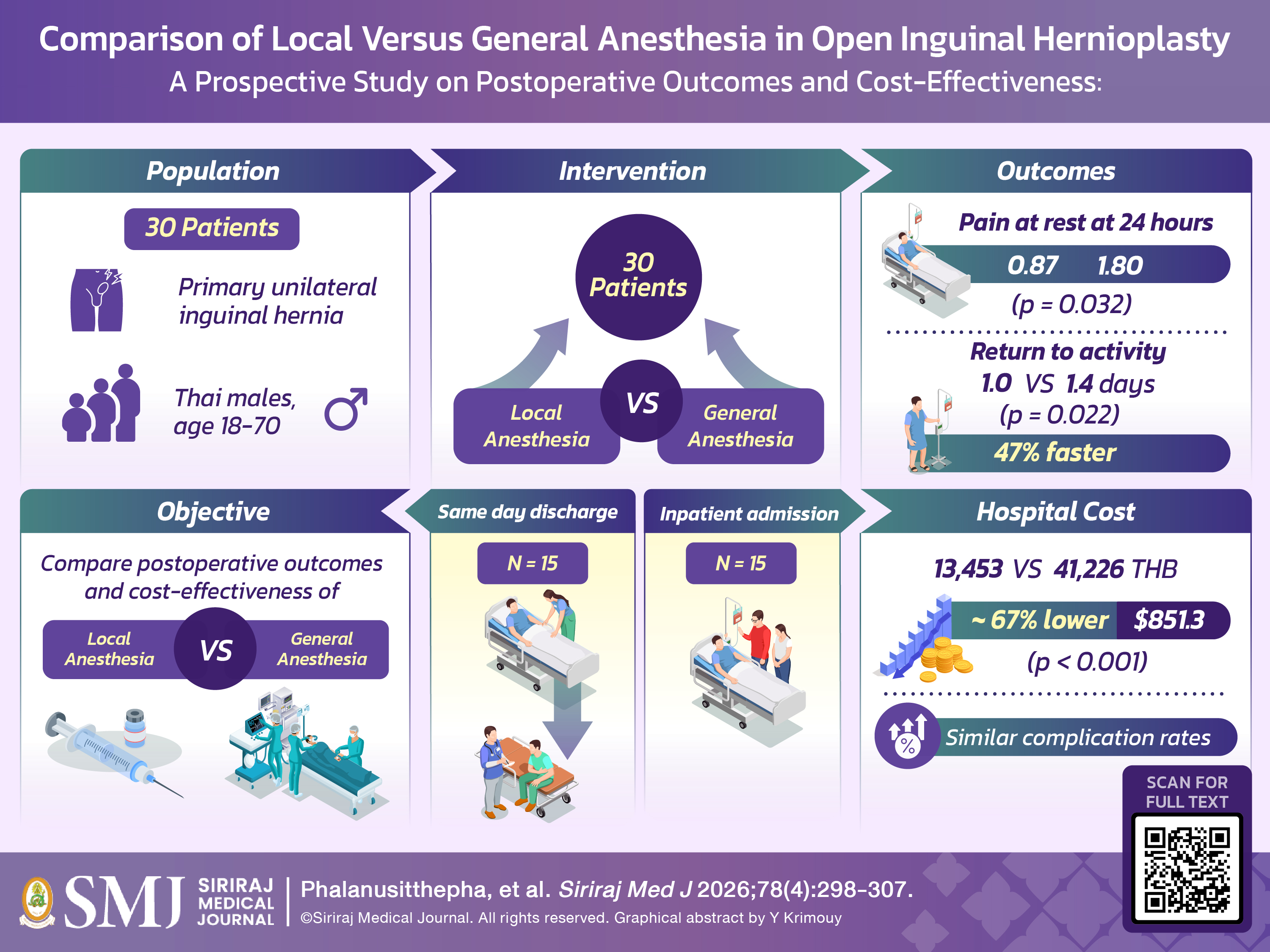
Objective: This study evaluates whether performing open inguinal hernia repair under local anesthesia with sameday discharge is comparable to general anesthesia with inpatient admission, with respect to postoperative outcomes, recovery time, and healthcare costs.
Materials and Methods: This prospective cohort study was conducted at Siriraj Hospital and included 30 adults undergoing unilateral open inguinal hernioplasty. Patients were allocated to either local anesthesia with same-day discharge (n=15) or general anesthesia with inpatient admission (n=15). Postoperative pain, recovery time, operative efficiency, complications, and total hospital costs were assessed.
Results: Postoperative pain at rest at 8 and 24 hours was lower in the LA group compared with the GA group (1.93±1.10 vs 2.53±1.55 p=0.233, 0.87±0.83 vs 1.80±1.65 p=0.032). Patients in the LA group resumed normal activities significantly earlier, and total hospital costs were significantly lower (1.00+0.54 vs 1.40+0.51 p = 0.022, 13,453 THB vs. 41,226 THB; p<0.001). Operative time, theater time, complications, and patient demographics (age, BMI, ASA classification) were comparable between groups.
Conclusions: Open inguinal hernioplasty under local anesthesia in a day-surgery setting demonstrated clinical outcomes comparable to those of general anesthesia with inpatient admission. Additionally, this approach was associated with faster functional recovery and significantly reduced hospital costs. Local anesthesia represents a safe, efficient, and cost-effective alternative for appropriately selected patients.
References
Fitzgibbons RJ, Jr., Forse RA. Clinical practice. Groin hernias in adults. N Engl J Med. 2015;372(8):756-63.
Primatesta P, Goldacre MJ. Inguinal hernia repair: incidence of elective and emergency surgery, readmission and mortality. Int J Epidemiol. 1996;25(4):835-9.
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, et al. European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2009;13(4):343-403.
Miserez M, Peeters E, Aufenacker T, Bouillot JL, Campanelli G, Conze J, et al. Update with level 1 studies of the European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2014;18(2):151-63.
Lomanto D, Cheah WK, Faylona JM, Huang CS, Lohsiriwat D, Maleachi A, et al. Inguinal hernia repair: toward Asian guidelines. Asian J Endosc Surg. 2015;8(1):16-23.
Burney RE, Prabhu MA, Greenfield ML, Shanks A, O'Reilly M. Comparison of spinal vs general anesthesia via laryngeal mask airway in inguinal hernia repair. Arch Surg. 2004;139(2):183-7.
Nordin P, Haapaniemi S, van der Linden W, Nilsson E. Choice of anesthesia and risk of reoperation for recurrence in groin hernia repair. Ann Surg. 2004;240(1):187-92.
Kehlet H, Aasvang E. Groin hernia repair: anesthesia. World J Surg. 2005;29(8):1058-61.
van Veen RN, Mahabier C, Dawson I, Hop WC, Kok NF, Lange JF, et al. Spinal or local anesthesia in lichtenstein hernia repair: a randomized controlled trial. Ann Surg. 2008;247(3):428-33.
Law LS, Tan M, Bai Y, Miller TE, Li YJ, Gan TJ. Paravertebral Block for Inguinal Herniorrhaphy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Anesth Analg. 2015;121(2):556-69.
Prakash D, Heskin L, Doherty S, Galvin R. Local anaesthesia versus spinal anaesthesia in inguinal hernia repair: A systematic review and meta-analysis. Surgeon. 2017;15(1):47-57.
Bakota B, Kopljar M, Baranovic S, Miletic M, Marinovic M, Vidovic D. Should we abandon regional anesthesia in open inguinal hernia repair in adults? Eur J Med Res. 2015;20(1):76.
Kazaure HS, Roman SA, Sosa JA. The resident as surgeon: an analysis of ACS-NSQIP. J Surg Res. 2012;178(1):126-32.
Lee SL, Sydorak RM, Applebaum H. Training general surgery residents in pediatric surgery: educational value vs time and cost. J Pediatr Surg. 2009;44(1):164-8.
Papandria D, Rhee D, Ortega G, Zhang Y, Gorgy A, Makary MA, et al. Assessing trainee impact on operative time for common general surgical procedures in ACS-NSQIP. J Surg Educ. 2012;69(2):149-55.
Sungurtekin H, Sungurtekin U, Erdem E. Local anesthesia and midazolam versus spinal anesthesia in ambulatory pilonidal surgery. J Clin Anesth. 2003;15(3):201-5.
Tverskoy M, Cozacov C, Ayache M, Bradley EL, Jr., Kissin I. Postoperative pain after inguinal herniorrhaphy with different types of anesthesia. Anesth Analg. 1990;70(1):29-35.
Haff RE, Stoltzfus J, Lucente VR, Murphy M. The Surgical Satisfaction Questionnaire (SSQ-8): A Validated Tool for Assessment of Patient Satisfaction Following Surgery To Correct Prolapse and/or Incontinence. J Minim Invasive Gynecol. 2011;18(6):S49-S50.
Li R, Atahar J, Noureldin A, Kartiko S. Favorable 30-day outcomes of initial open inguinal hernia repair with local anesthesia among frail patients. J Visc Surg. 2025;162(3):178-84.
Nordin P, Zetterström H, Gunnarsson U, Nilsson E. Local, regional, or general anaesthesia in groin hernia repair: multicentre randomised trial. The Lancet. 2003;362:853-8.
Balentine CJ, Meier J, Berger M, Reisch J, Cullum M, Lee SC, et al. Using Local Anesthesia for Inguinal Hernia Repair Reduces Complications in Older Patients. J Surg Res. 2021;258:64-72.
Argo M, Favela J, Phung T, Huerta S. Local VS. other forms of anesthesia for open inguinal hernia repair: A meta-analysis of randomized controlled trials. Am J Surg. 2019;218(5):1008-15.
Published
How to Cite
License
Copyright (c) 2026 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














