Long-Term Refractive Outcomes Following Pediatric Cataract Surgery with Primary IOL Implantation
DOI:
https://doi.org/10.33192/smj.v78i5.280456Keywords:
Cataract, Pediatric ophthalmology, Myopic shiftAbstract
Objective: To evaluate long-term refractive outcomes following pediatric cataract surgery with primary intraocular lens (IOL) implantation.
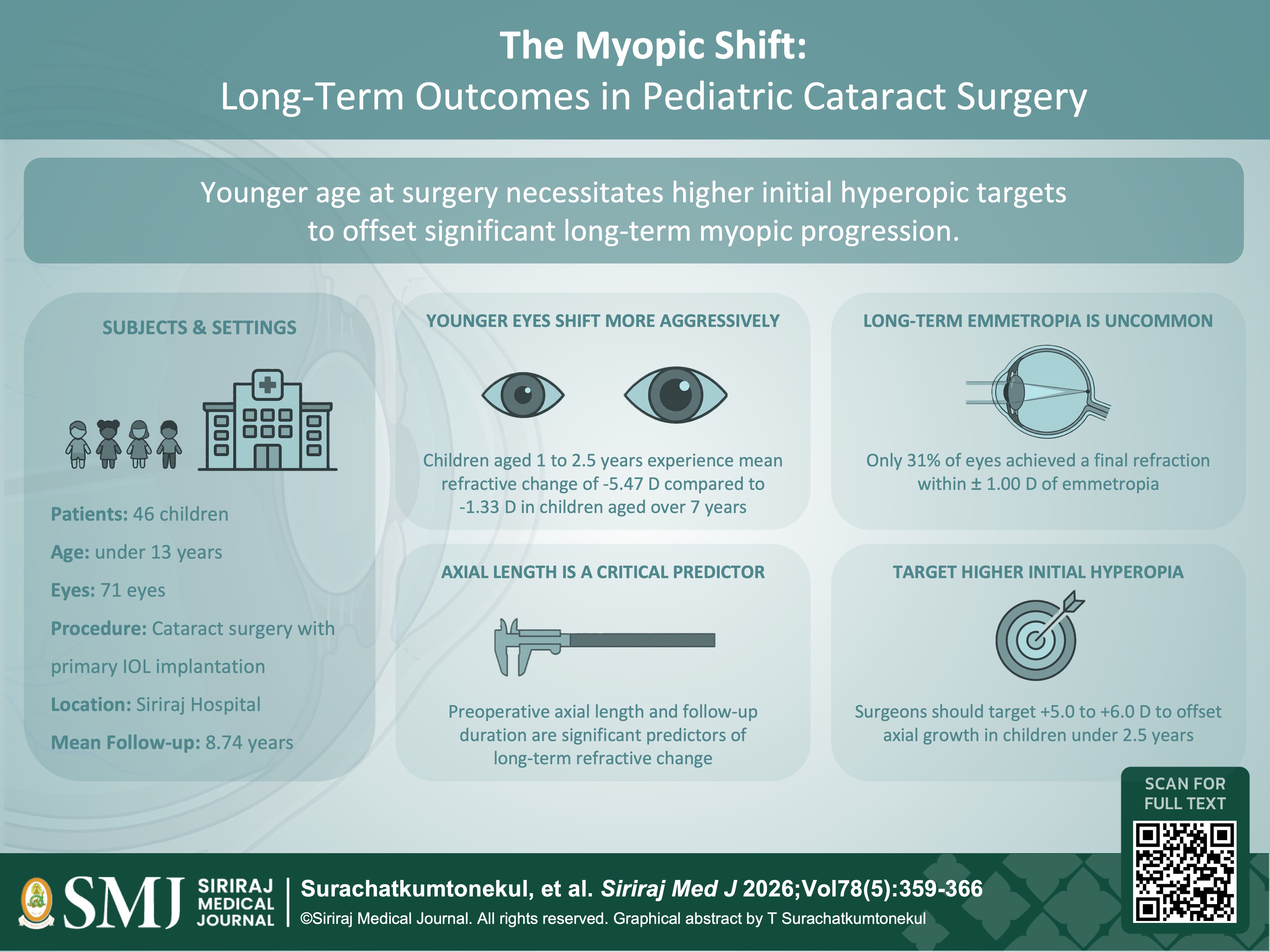
Materials and Methods: A retrospective review was conducted on children younger than 13 years who underwent cataract surgery with primary IOL implantation at Siriraj Hospital between 2000 and 2020, with a minimum follow-up of 5 years. Refractive data were converted to spherical equivalents. Linear mixed models were used to analyze refractive shifts across four age groups (1 to <2.5, 2.5 to <4, 4 to <7, and 7 to <13 years) and identify influencing factors.
Results: The study included 71 eyes of 46 children, with a mean follow-up of 8.74 ± 3.01 years. The mean final refractive change ranged from -5.47 D (95% CI: -7.93, -3.01) in children aged 1 to <2.5 years to -1.33 D (95% CI: -1.99, -0.67) in those aged 7 to <13 years. Overall, only 30.99% of eyes achieved a final refraction within ±1.00 D of emmetropia. Multivariate analysis identified preoperative axial length (P = 0.005) and follow-up duration (P = 0.003) as significant predictors of refractive change.
Conclusion: Younger age at surgery correlates with greater magnitude and variability of myopic shift. Standard guidelines should be adapted to target higher residual hyperopia to achieve optimal long-term emmetropic refraction.
References
Rahi JS, Dezateux C, British Congenital Cataract Interest G. Measuring and interpreting the incidence of congenital ocular anomalies: lessons from a national study of congenital cataract in the UK. Invest Ophthalmol Vis Sci. 2001;42(7):1444–8.
Kim DG, Lee DY, Woo SJ, Park KH, Park SJ. Nationwide incidence of congenital and infantile cataract requiring surgery in Korea. Sci Rep. 2024;14(1):5251.
Weakley DR, Jr., Lynn MJ, Dubois L, Cotsonis G, Wilson ME, Buckley EG, et al. Myopic Shift 5 Years after Intraocular Lens Implantation in the Infant Aphakia Treatment Study. Ophthalmology. 2017;124(6):822–7.
Repka MX, Dean TW, Kraker RT, Li Z, Yen KG, de Alba Campomanes AG, et al. Visual Acuity and Ophthalmic Outcomes 5 Years After Cataract Surgery Among Children Younger Than 13 Years. JAMA Ophthalmol. 2022;140(3):269–76.
Enyedi LB, Peterseim MW, Freedman SF, Buckley EG. Refractive changes after pediatric intraocular lens implantation. Am J Ophthalmol. 1998;126(6):772–81.
Plager DA, Kipfer H, Sprunger DT, Sondhi N, Neely DE. Refractive change in pediatric pseudophakia: 6-year follow-up. J Cataract Refract Surg. 2002;28(5):810–5.
Crouch ER, Crouch ER, Jr., Pressman SH. Prospective analysis of pediatric pseudophakia: myopic shift and postoperative outcomes. J AAPOS. 2002;6(5):277–82.
Orazbekov L, Smagulova S, Ruslanuly K. Long-term Results of Congenital Cataract Surgery with Primary Intraocular Lens Implantation: A Case-Control Study of Three Age Groups. J Curr Ophthalmol. 2022;34(3):290–6.
VanderVeen DK, Oke I, Nihalani BR. Deviations From Age-Adjusted Normative Biometry Measures in Children Undergoing Cataract Surgery: Implications for Postoperative Target Refraction and IOL Power Selection. Am J Ophthalmol. 2022;239:190–201.
Pediatric Eye Disease Investigator G, de Alba Campomanes AG, Repka MX, Hatt SR, Sutherland DR, Leske DA, et al. Myopic Shift over 5 Years after Pediatric Lensectomy with Primary Intraocular Lens Implantation. Ophthalmology. 2025;132(3):290–8.
Lekskul A, Chuephanich P, Charoenkijkajorn C. Long-term outcomes of intended undercorrection intraocular lens implantation in pediatric cataract. Clin Ophthalmol. 2018;12:1905–11.
Wu PC, Huang HM, Yu HJ, Fang PC, Chen CT. Epidemiology of Myopia. Asia Pac J Ophthalmol (Phila). 2016;5(6):386–93.
Li Y, Jin G, Tan Y, Chen H, Jin J, Luo L, et al. Myopic shift after primary intraocular lens implantation in unilateral cataract children and its association with preoperative ocular parameters. J Cataract Refract Surg. 2025;51(1):53–9.
Troilo D, Wallman J. The regulation of eye growth and refractive state: an experimental study of emmetropization. Vision Res. 1991;31(7-8):1237–50.
Lambert SR, Archer SM, Wilson ME, Trivedi RH, del Monte MA, Lynn M. Long-term Outcomes of Undercorrection Versus Full Correction After Unilateral Intraocular Lens Implantation in Children. Am J Ophthalmol. 2012;153(4):602–8, 8 e1.
Valeina S, Heede S, Erts R, Sepetiene S, Skaistkalne E, Radecka L, et al. Factors influencing myopic shift in children after intraocular lens implantation. Eur J Ophthalmol. 2020;30(5):933–40.
Surachatkumtonekul T, Jaruniphakul P. Prevalence, Predictive Factors, and Surgical Outcomes of Strabismus in High Myopia. Siriraj Med J. 2026;78(3):175–84.
Trivedi RH, Barnwell E, Wolf B, Wilson ME. A Model to Predict Postoperative Axial Length in Children Undergoing Bilateral Cataract Surgery With Primary Intraocular Lens Implantation. Am J Ophthalmol. 2019;206:228–34.
Gouws P, Hussin HM, Markham RH. Long term results of primary posterior chamber intraocular lens implantation for congenital cataract in the first year of life. Br J Ophthalmol. 2006;90(8):975–8.
Hoevenaars NE, Polling JR, Wolfs RC. Prediction error and myopic shift after intraocular lens implantation in paediatric cataract patients. Br J Ophthalmol. 2011;95(8):1082–5.
Trivedi RH, Wilson ME, Jr. Changes in interocular axial length after pediatric cataract surgery. J AAPOS. 2007;11(3):225–9.
Infant Aphakia Treatment Study Group, Lambert SR, Lynn MJ, et al. Comparison of contact lens and intraocular lens correction of monocular aphakia during infancy: a randomized clinical trial of HOTV optotype acuity at age 4.5 years and clinical findings at age 5 years. JAMA Ophthalmol. 2014;132(6):676-82.
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














