The Outcomes of Siriraj’s Classification for Giant Inguinal Hernia: A Literature Review and Metaanalysis
DOI:
https://doi.org/10.33192/smj.v78i5.280511Keywords:
Giant inguinal hernia, hernia repair, surgical outcomes, postoperative complications, classification, meta-analysisAbstract
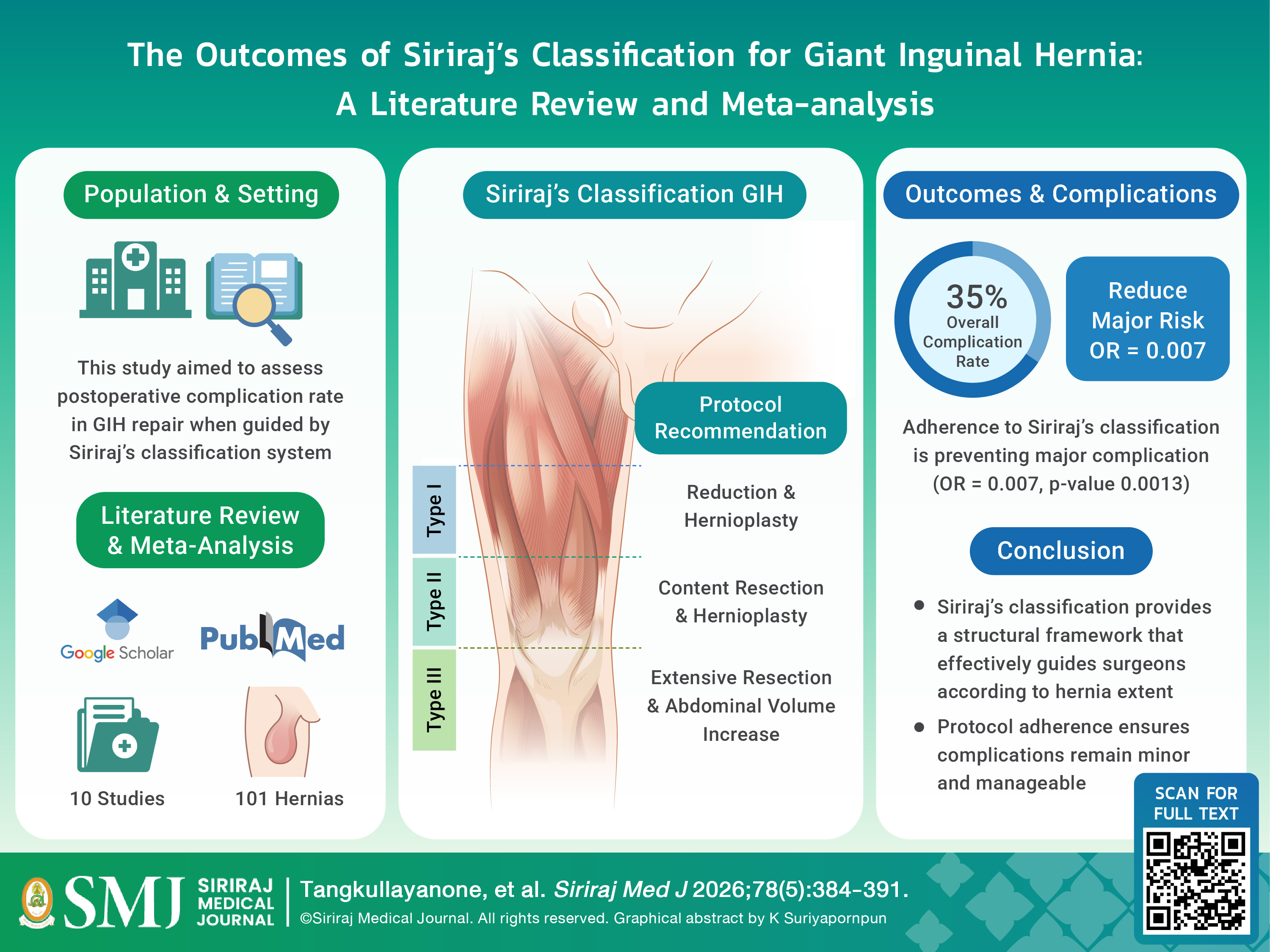
Objective: Giant inguinal hernia is a rare condition associated with high perioperative morbidity. Siriraj’s classification was developed to guide surgical management according to hernia extent; however, clinical outcome data remain limited. This study aimed to evaluate postoperative complications associated with giant inguinal hernia repair according to Siriraj’s classification.
Materials and Methods: A literature review and proportion meta-analysis were conducted to assess the surgical outcomes of giant inguinal hernia repair. PubMed and Google Scholar were systematically searched for studies reporting surgical management and complications of giant inguinal hernia. Studies were included if the hernia type could be classified according to Siriraj’s classification or sufficient clinical information was available. The primary outcome was postoperative complications. Pooled complication rates with 95% confidence intervals (CI) were calculated using fixed- or random-effects models based on heterogeneity.
Results: Ten studies involving 101 giant inguinal hernias were included in the meta analysis. The overall postoperative complication rate was 35% (95% CI: 0.17–0.59). Type I giant inguinal hernia showed a complication rate of 43%, while non-Type I hernias demonstrated a complication rate of 37%. Although overall complication rates were comparable, major complications were predominantly observed in cases not adhering to Siriraj’s classification. Protocol adherence was significantly associated with reduced risk of major complications (odds ratio 0.007, 95% CI: 0.0003–0.142; p=0.0013).
Conclusion: Siriraj’s classification provides a practical framework for guiding surgical management of giant inguinal hernia and may reduce major postoperative complications. Further large-scale studies are required to validate these findings.
References
Abebe MS, Tareke AA, Alem A, Debebe W, Beyene A. Worldwide magnitude of inguinal hernia: Systematic review and meta-analysis of population-based studies. SAGE Open Med. 2022;10:20503121221139150.
Menenakos C, Albrecht HC, Gretschel S. Bilateral giant inguinoscrotal hernia. Presentation of a novel combined two-stage repair approach. J Surg Case Rep. 2020;2020(3):rjaa012.
Trakarnsagna A, Chinswangwatanakul V, Methasate A, Swangsri J, Phalanusitthepha C, Parakonthun T, et al. Giant inguinal hernia: Report of a case and reviews of surgical techniques. Int J Surg Case Rep. 2014;5(11):868-72.
Cavalli M, Biondi A, Bruni PG, Campanelli G. Giant inguinal hernia: the challenging hug technique. Hernia. 2015;19(5):775-83.
Anand M, Hajong R, Naku N, Hajong D, Singh KL. Giant Inguinal Herniae Managed by Primary Repair: A Case Series. J Clin Diagn Res. 2017;11(2):PR01-PR02.
Fujinaka R, Urade T, Fukuoka E, Murata K, Mii Y, Sawa H, et al. Laparoscopic transabdominal preperitoneal approach for giant inguinal hernias. Asian J Surg. 2019;42(1):414-9.
Sanford Z, Weltz AS, Singh D, Hanley R, Todd D, Belyansky I. Minimally Invasive Multidisciplinary Approach to Chronic Giant Inguinoscrotal Hernias. Surg Innov. 2019;26(4):427-31.
Gonzalez-Urquijo M, Estrada-Cortinas OJ, Rodarte-Shade M, Bermea-Mendoza JH, Gil-Galindo G. Preoperative progressive pneumoperitoneum: The answer for treating giant inguinal hernias while avoiding morbidities? Hernia. 2020;24(4):781-6.
Lin R, Lu F, Lin X, Yang Y, Chen Y, Huang H. Transinguinal preperitoneal repair of giant inguinoscrotal hernias using Kugel mesh. J Visc Surg. 2020;157(5):372-7.
Morrell AC, Morrell ALG, Malcher F, Morrell AG, Morrell-Junior AC. Primary Abandon-of-the-Sac (Pas) Technique: Preliminary Results of a Novel Minimally Invasive Approach for Inguinoscrotal Hernia Repair. Arq Bras Cir Dig. 2020;33(2):e1519.
Tang FX, Zong Z, Xu JB, Ma N, Zhou TC, Chen S. Combination of Preoperative Progressive Pneumoperitoneum and Botulinum Toxin A Enables the Laparoscopic Transabdominal Preperitoneal Approach for Repairing Giant Inguinoscrotal Hernias. J Laparoendosc Adv Surg Tech A. 2020;30(3):260-6.
Basukala S, Rijal S, Pathak BD, Gupta RK, Thapa N, Mishra R. Bilateral giant inguinoscrotal hernia: A case report. Int J Surg Case Rep. 2021;88:106467.
Luo H, Zhang H, Sun J, Chen Y, Qi X, Wang H, et al. Laparoscopic transabdominal preperitoneal approach with negative pressure drainage for giant inguinal hernia. J Laparoendosc Adv Surg Tech A. 2021;31(8):931-6.
Monestiroli UM, Bondurri A, Gandini F, Lenna G, Vellini S, Danelli P. Giant inguinoscrotal hernia. Tech Coloproctol. 2007;11(3):283-4.
Tahir M, Ahmed FU, Seenu V. Giant inguinoscrotal hernia: case report and management principles. Int J Surg. 2008;6(6):495-7.
Vasiliadis K, Knaebel HP, Djakovic N, Nyarangi-Dix J, Schmidt J, Büchler M. Challenging surgical management of a giant inguinoscrotal hernia: report of a case. Surg Today. 2010;40(7):684-7.
Gaedcke J, Schüler P, Brinker J, Quintel M, Ghadimi M. Emergency repair of giant inguinoscrotal hernia in a septic patient. J Gastrointest Surg. 2013;17(4):837-9.
Karthikeyan VS, Sistla SC, Ram D, Ali SM, Rajkumar N. Giant inguinoscrotal hernia--report of a rare case with literature review. Int Surg. 2014;99(5):560-4.
Lajevardi SS, Gundara JS, Collins SA, Samra JS. Acute Gastric Rupture in a Giant Inguinoscrotal Hernia. J Gastrointest Surg. 2015;19(12):2283-5.
Tarchouli M, Ratbi MB, Bouzroud M, Aitidir B, Ait-Ali A, Bounaim A, Sair K. Giant inguinoscrotal hernia containing intestinal segments and urinary bladder successfully repaired by simple hernioplasty technique: a case report. J Med Case Rep. 2015;9:276.
Sahsamanis G, Samaras S, Basios A, Katis K, Dimitrakopoulos G. Treatment of a half century year old giant inguinoscrotal hernia. A case report. Int J Surg Case Rep.2016;25:51-4.
Prochotsky A, Dolak S, Minarovjech V, Medzo I, Hutan M, Mifkovic A. Giant inguinoscrotal hernia repair. Bratisl Lek Listy. 2017;118(8):472-8.
Staubitz JI, Gassmann P, Kauff DW, Lang H. Surgical treatment strategies for giant inguinoscrotal hernia - a case report with review of the literature. BMC Surg. 2017;17(1):135.
Aguirre JE, Ruiz-Niño H, Maria M, Jose A, Jorge JJACES. Case report: preoperative progressive pneumoperitoneum in giant inguinoscrotal hernia. Arch Clin Exp Surg. 2018;7(2):84-8.
Hever P, Dhar M, Cavale N. Loss of domain leading to intra-operative cardiorespiratory arrest during open repair of a giant inguinoscrotal hernia and hydrocele. JPRAS Open. 2018;16:1-5.
Sprunger H, Carbonell AM, Marguet CG, Cobb WS, Warren JA, Flanagan WF. Staged Management of Giant Inguinoscrotal Hernia. Am Surg. 2018;84(3):e114-e6.
Caruso R, Vicente E, Quijano Y, D’Ovidio A, Ielpo B, Ferri VJIJoSCR. Review with video of a laparoscopic transabdominal preperitoneal (TAPP) repair for giant inguinoscrotal hernia. Int J Surg Case Rep. 2020;76:549-51.
Lin M, Long G, Chen M, Chen W, Mo J, Chen N. Giant recurrent left inguinal hernia with femoral nerve injury: a report of a rare case. BMC Surg. 2020;20(1):123.
Voravisutthikul P. Case report: multi-stage operation for giant inguinoscrotal hernia repair. Mahasarakham Hospital Journal. 2020;17(2):142-8.
Porfidia R, Grimaldi S, Picarella P, Ciolli M, Romano AJAICMCA-Da. Giant Inguinoscrotal Hernia: Single-Stage Repair Using Posterior Component Separation Technique and Transversus Abdominis Release. Annals of International Clinical and Medical Case Reports. 2020;11. Available from: https://www.sergiogrimaldi.it/wp-content/uploads/2022/02/Ernia-Inguinoscrotale-2020.pdf
Brandt ASV, Tastesen J, Sværdborg M, Kirkeby HJ. Joint venture surgery of a giant inguinoscrotal hernia in a patient suffering from trisomy 21 and Eisenmenger's syndrome. Urol Case Rep. 2021;39:101757.
Cubero JÁO, Soto-Bigot M, Chaves-Sandí M, Méndez-Villalobos A, Martínez-Hoed JJIJoAW, Surgery H. Surgical treatment for inguinoscrotal hernia with loss of dominion with preoperative progressive pneumoperitoneum and botulinum toxin: Case report and systematic review of the literature. International Journal of Abdominal Wall and Hernia Surgery. 2021;4(4):156-65.
Davis T, Vivens M, Barghuthi L, Ismael H. Giant sliding inguinal hernia requiring intraoperative aspiration of fluid: a case report and literature review. J Surg Case Rep. 2021;2021(8):rjab340.
Ilma W. Hernia Inguinalis Permagna: Laporan Kasus. Medula. 2021;11(1):151-6.
Olaogun JG, Ige JT, Kadiri IA, Wuraola OK. Giant Inguinal Hernia: Two Case Reports and Literature Review. 2021. Available from: https://www.researchgate.net/publication/367793887_Giant_Inguinal_Hernia_Two_Case_Reports_and_Literature_Review
Polat FR. Bilateral giant inguinoscrotal hernia with hydrocele. A case report. J Surg Arts. 2021;14(2):82-5.
Quarto G, D'Amore A, Vertaldi S, Anoldo P, Benassai G, De Palma GD, et al. A giant inguinal hernia in a patient with Ehlers-Danlos syndrome. Ann Ital Chir. 2021;10:S2239253X21034770.
Sewalia P, Chawla AS, Sangtam LT, Mandalapu H, Kumar H, Kaur A, et al. Repair of giant inguino-scrotal hernia with loss of domain using minimally invasive anterior component separation technique combined with Lichtenstein tension-free mesh hernioplasty. International Surgery Journal. 2021;8(1):406-10.
Nakamura K, Shibasaki S, Takenaka M, Serizawa A, Akimoto S, Nakauchi M, et al. Orchiectomy due to delayed severe scrotal hematocele after laparoscopic transabdominal preperitoneal repair for a giant inguinoscrotal hernia: a case report. Surg Case Rep. 2022;8(1):222.
Goroeasem S, Vijayalakshmi V, Farook M. Role of progressive preoperative pneumoperitoneum in the management of giant inguinoscrotal hernia-case report. International Surgery Journal. 2023;10(2):315-8.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6,336 patients and results of a survey. Ann Surg. 2004;240(2):205-13.
Published
How to Cite
License
Copyright (c) 2026 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














