Predictive Models for Screening of Postoperative Cognitive Dysfunction in Older Surgical Patients
DOI:
https://doi.org/10.33192/smj.v78i3.279441Keywords:
Cognitive impairment, frailty, functional impairment, postoperative neurocognitive disorders, predictive factorsAbstract
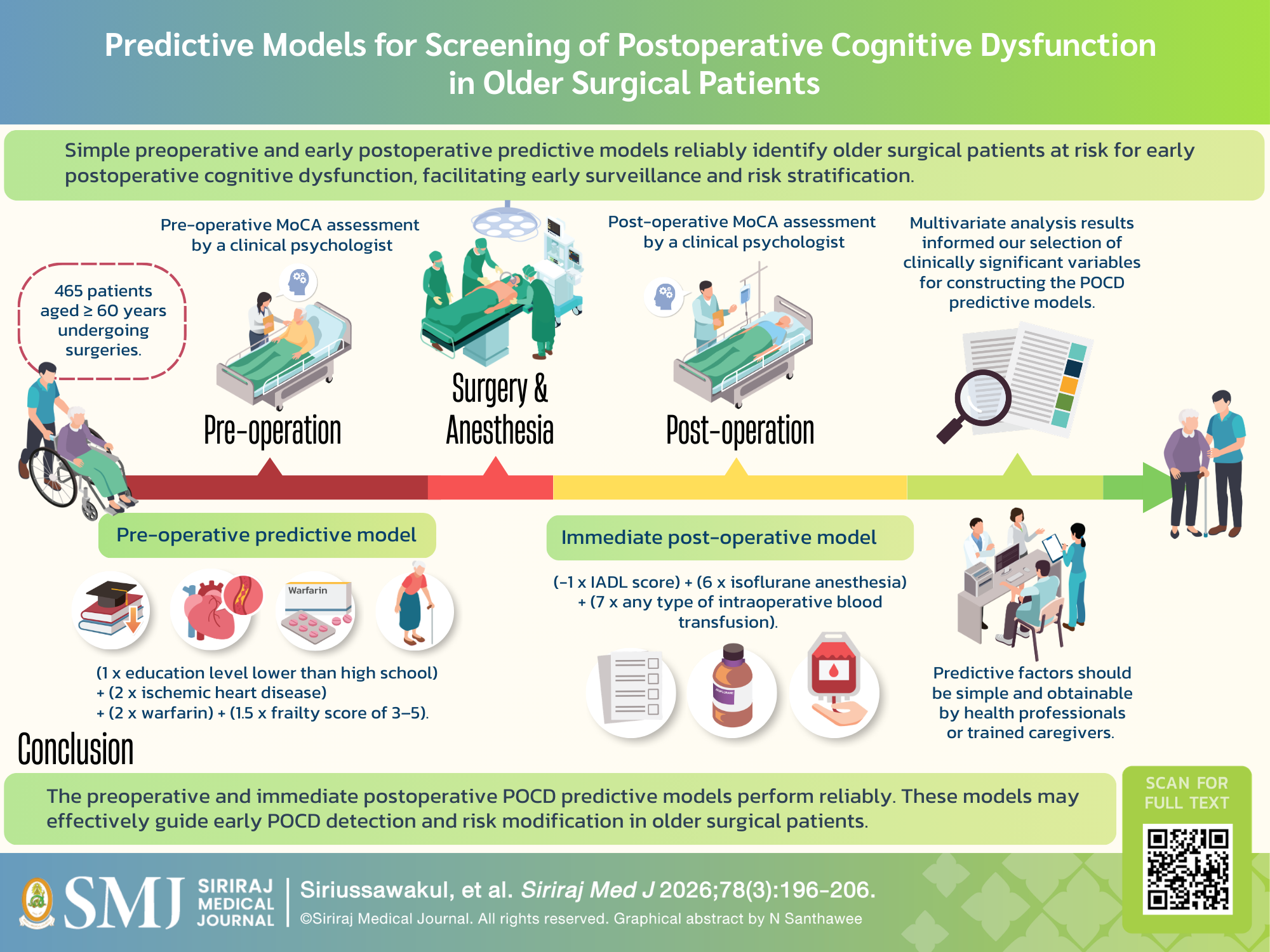
Objective: Postoperative cognitive dysfunction (POCD) substantially impacts the long-term quality of life of patients and caregivers. Early detection of POCD is essential. We devised quick vigilance screening models for application preoperatively (model one) and during the postoperative period (model two) to predict the development of early POCD (one week after surgery).
Materials and Methods: We conducted a cohort study on patients aged ≥ 60 years undergoing cardiac or noncardiac surgeries. POCD was defined as a postoperative Montreal Cognitive Assessment decrease of ≥ two points from the baseline preoperative score. We stipulated that predictive factors should be simple and obtainable by health professionals or trained caregivers. Multivariate analysis results informed our selection of clinically significant variables for constructing the POCD predictive models.
Results: Of the 465 patients in the final analysis, the early POCD incidence was 24.9%. The equation used for predictive model one was (1 x education level lower than high school) + (2 x ischemic heart disease) + (2 x warfarin) + (1.5 x frailty score of 3–5). The equation for model two was (-1 x IADL score) + (6 x isoflurane anesthesia) + (7 x any type of intraoperative blood transfusion). Both models displayed well-calibrated curves. The optimal cut-off values of model one and model two to discriminate between a high and low probability of POCD were 2 and 0, respectively.
Conclusions: The preoperative and immediate postoperative POCD predictive models perform reliably. These models may effectively guide early POCD detection and risk modification in older surgical patients.
References
Kotekar N, Shenkar A, Nagaraj R. Postoperative cognitive dysfunction - current preventive strategies. Clin Interv Aging. 2018;13:2267-73.
Monk TG, Weldon BC, Garvan CW, Dede DE, van der Aa MT, Heilman KM, Gravenstein JS. Predictors of cognitive dysfunction after major noncardiac surgery. Anesthesiology. 2008;108(1):18-30.
Steinmetz J, Christensen KB, Lund T, Lohse N, Rasmussen LS. Long-term consequences of postoperative cognitive dysfunction. Anesthesiology. 2009;110(3):548-55.
Deiner S, Liu X, Lin HM, Jacoby R, Kim J, Baxter MG, et al. Does Postoperative Cognitive Decline Result in New Disability After Surgery? Ann Surg. 2021;274(6):e1108-e14.
Suraarunsumrit P, Pathonsmith C, Srinonprasert V, Sangarunakul N, Jiraphorncharas C, Siriussawakul A. Postoperative cognitive dysfunction in older surgical patients associated with increased healthcare utilization: a prospective study from an upper-middle-income country. BMC Geriatr. 2022;22(1):213.
Shiraboina M, Ayya S, Srikanth Y, Kumar R, Durga P, Gopinath R. Predictors of postoperative cognitive dysfunction in adult patients undergoing elective cardiac surgery. Indian J Anaesth. 2014;58(3):334-6.
Huang H, Chou J, Tang Y, Ouyang W, Wu X, Le Y. Nomogram to predict postoperative cognitive dysfunction in elderly patients undergoing gastrointestinal tumor resection. Front Aging Neurosci. 2022;14:1037852.
Liu J, Huang K, Zhu B, Zhou B, Ahmad Harb AK, Liu L, Wu X. Neuropsychological Tests in Post-operative Cognitive Dysfunction: Methods and Applications. Front Psychol. 2021;12:684307.
Needham MJ, Webb CE, Bryden DC. Postoperative cognitive dysfunction and dementia: what we need to know and do. Br J Anaesth. 2017;119(suppl_1):i115-i25.
Moller JT, Cluitmans P, Rasmussen LS, Houx P, Rasmussen H, Canet J, et al. Long-term postoperative cognitive dysfunction in the elderly ISPOCD1 study. ISPOCD investigators. International Study of Post-Operative Cognitive Dysfunction. Lancet. 1998;351(9106):857-61.
Huang C, Mårtensson J, Gögenur I, Asghar MS. Exploring Postoperative Cognitive Dysfunction and Delirium in Noncardiac Surgery Using MRI: A Systematic Review. Neural Plast. 2018;2018:1281657.
Paredes S, Cortínez L, Contreras V, Silbert B. Post-operative cognitive dysfunction at 3 months in adults after non-cardiac surgery: a qualitative systematic review. Acta Anaesthesiol Scand. 2016;60(8):1043-58.
Relander K, Hietanen M, Rantanen K, Rämö J, Vento A, Saastamoinen KP, et al. Postoperative cognitive change after cardiac surgery predicts long-term cognitive outcome. Brain Behav. 2020;10(9):e01750.
Newman MF, Kirchner JL, Phillips-Bute B, Gaver V, Grocott H, Jones RH, et al. Longitudinal assessment of neurocognitive function after coronary-artery bypass surgery. N Engl J Med. 2001;344(6):395-402.
Green CM, Schaffer SD. Postoperative cognitive dysfunction in noncardiac surgery: A review. Trends in Anaesthesia and Critical Care. 2019;24:40-8.
Berger M, Terrando N, Smith SK, Browndyke JN, Newman MF, Mathew JP. Neurocognitive Function after Cardiac Surgery: From Phenotypes to Mechanisms. Anesthesiology. 2018;129(4):829-51.
Cheng H, Clymer JW, Po-Han Chen B, Sadeghirad B, Ferko NC, Cameron CG, Hinoul P. Prolonged operative duration is associated with complications: a systematic review and meta-analysis. J Surg Res. 2018;229:134-44.
Hua M, Min J. Postoperative Cognitive Dysfunction and the Protective Effects of Enriched Environment: A Systematic Review. Neurodegener Dis. 2020;20(4):113-22.
Suenghataiphorn T, Songwisit S, Tornsatitkul S, Somnuke P. An Overview on Postoperative Cognitive Dysfunction; Pathophysiology, Risk Factors, Prevention and Treatment. Siriraj Medical Journal. 2022;74(10):705-13.
Zhu S-H, Ji M-H, Gao D-P, Li W-Y, Yang J-J. Association between perioperative blood transfusion and early postoperative cognitive dysfunction in aged patients following total hip replacement surgery. Upsala Journal of Medical Sciences. 2014;119(3):262-7.
Plaschke K, Hauth S, Jansen C, Bruckner T, Schramm C, Karck M, Kopitz J. The influence of preoperative serum anticholinergic activity and other risk factors for the development of postoperative cognitive dysfunction after cardiac surgery. J Thorac Cardiovasc Surg. 2013;145(3):805-11.
Rossi A, Burkhart C, Dell-Kuster S, Pollock BG, Strebel SP, Monsch AU, et al. Serum anticholinergic activity and postoperative cognitive dysfunction in elderly patients. Anesth Analg. 2014;119(4):947-55.
Yang X, Huang X, Li M, Jiang Y, Zhang H. Identification of individuals at risk for postoperative cognitive dysfunction (POCD). Ther Adv Neurol Disord. 2022;15:17562864221114356.
Tangwongchai S, Charernboon T, Phanasathit M, Akkayagorn L, Hemrungrojn S, K P, Zs N. The validity of thai version of the montreal cognitive assessment (MoCA-T)2009. 172 p.
Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatrics. 2017;17(1):230.
Bursac Z, Gauss CH, Williams DK, Hosmer DW. Purposeful selection of variables in logistic regression. Source Code Biol Med. 2008;3:17.
Roalf DR, Moberg PJ, Xie SX, Wolk DA, Moelter ST, Arnold SE. Comparative accuracies of two common screening instruments for classification of Alzheimer's disease, mild cognitive impairment, and healthy aging. Alzheimers Dement. 2013;9(5):529-37.
Litaker D, Locala J, Franco K, Bronson DL, Tannous Z. Preoperative risk factors for postoperative delirium. Gen Hosp Psychiatry. 2001;23(2):84-9.
Bowden T, Hurt CS, Sanders J, Aitken LM. Predictors of cognitive dysfunction after cardiac surgery: a systematic review. Eur J Cardiovasc Nurs. 2022;21(3):192-204.
Prystowsky EN, Padanilam BJ. Preserve the brain: primary goal in the therapy of atrial fibrillation. J Am Coll Cardiol. 2013;62(6):540-2.
Mahanna-Gabrielli E, Zhang K, Sieber FE, Lin HM, Liu X, Sewell M, et al. Frailty Is Associated With Postoperative Delirium But Not With Postoperative Cognitive Decline in Older Noncardiac Surgery Patients. Anesth Analg. 2020;130(6):1516-23.
Nomura Y, Nakano M, Bush B, Tian J, Yamaguchi A, Walston J, et al. Observational Study Examining the Association of Baseline Frailty and Postcardiac Surgery Delirium and Cognitive Change. Anesth Analg. 2019;129(2):507-14.
Androsova G, Krause R, Winterer G, Schneider R. Biomarkers of postoperative delirium and cognitive dysfunction. Front Aging Neurosci. 2015;7:112.
Yao X, Li H, Leng SX. Inflammation and immune system alterations in frailty. Clin Geriatr Med. 2011;27(1):79-87.
Afilalo J, Mottillo S, Eisenberg MJ, Alexander KP, Noiseux N, Perrault LP, et al. Addition of frailty and disability to cardiac surgery risk scores identifies elderly patients at high risk of mortality or major morbidity. Circ Cardiovasc Qual Outcomes. 2012;5(2):222-8.
Additional Files
Published
How to Cite
License
Copyright (c) 2026 Siriraj Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Authors who publish with this journal agree to the following conditions:
Copyright Transfer
In submitting a manuscript, the authors acknowledge that the work will become the copyrighted property of Siriraj Medical Journal upon publication.
License
Articles are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0). This license allows for the sharing of the work for non-commercial purposes with proper attribution to the authors and the journal. However, it does not permit modifications or the creation of derivative works.
Sharing and Access
Authors are encouraged to share their article on their personal or institutional websites and through other non-commercial platforms. Doing so can increase readership and citations.














